Pulmonary nodules are detected in millions of patients each year, whether incidentally or through organized lung cancer screening, and many ultimately require tissue diagnosis to distinguish malignancy from benign disease. In clinical practice, two of the most widely used biopsy strategies for peripheral pulmonary nodules are navigational bronchoscopy vs transthoracic needle biopsy for lung nodules. Both are familiar to thoracic teams, but until recently, the field lacked randomized evidence directly comparing their diagnostic performance and safety.
The VERITAS trial, published in the New England Journal of Medicine, now provides that comparison. In this multicenter, randomized, noninferiority trial, investigators evaluated navigational bronchoscopy vs transthoracic needle biopsy for lung nodules measuring 10 to 30 mm in patients with an intermediate or high pretest probability of cancer. The study found that navigational bronchoscopy was noninferior to transthoracic needle biopsy for diagnostic accuracy, while also causing substantially fewer complications, especially pneumothorax (Lentz et al., 2025).
These findings are clinically important because they address one of the most common and practical questions in thoracic oncology and interventional pulmonology: when both procedures are technically feasible, which one should be preferred?
Why This Question Matters
The workup of a peripheral pulmonary nodule is often a balance between diagnostic certainty and procedural risk. Transthoracic needle biopsy has traditionally been regarded as highly accurate, with reports in prior literature suggesting diagnostic accuracy approaching 90% in some settings. However, it requires passage through the chest wall and pleura and has long been associated with substantial pneumothorax risk. Navigational bronchoscopy, by contrast, avoids pleural puncture and generally has a lower complication profile, but historically its diagnostic accuracy has been more variable, especially when older navigation platforms relied mainly on two-dimensional fluoroscopy.
Newer bronchoscopy systems that integrate navigation with digital tomosynthesis or other three-dimensional imaging methods have improved performance. Even so, before VERITAS there had been no randomized comparison robust enough to define whether navigational bronchoscopy vs transthoracic needle biopsy for lung nodules should be viewed as equivalent from a diagnostic standpoint.
Trial Design
VERITAS was an investigator-initiated, multicenter, open-label, randomized, parallel-group noninferiority trial conducted across seven centers in the United States. Eligible adults had a single peripheral indeterminate pulmonary nodule measuring 10 to 30 mm and a calculated pretest probability of cancer of at least 10%. To ensure fairness in the comparison, each case had to be centrally reviewed and deemed technically amenable to both navigational bronchoscopy and transthoracic needle biopsy before randomization (Lentz et al., 2025).
Patients were randomly assigned in a 1:1 ratio to undergo one of the two procedures. Randomization was stratified according to nodule location within the lung, pretest probability of cancer, and study site. The primary endpoint was diagnostic accuracy, defined as the percentage of patients whose biopsy yielded a specific diagnosis, either cancer or a specific benign condition, that was later confirmed to be correct through 12 months of clinical follow-up. The noninferiority margin was set at 10 percentage points (Lentz et al., 2025).
This is an important detail, because the trial was not merely comparing whether one test could obtain tissue, but whether it could provide a diagnosis that remained correct after a full year of follow-up. That makes the study especially relevant for real-world decision making around navigational bronchoscopy vs transthoracic needle biopsy for lung nodules.
Copyright © 2025 Massachusetts Medical Society
Patient Population
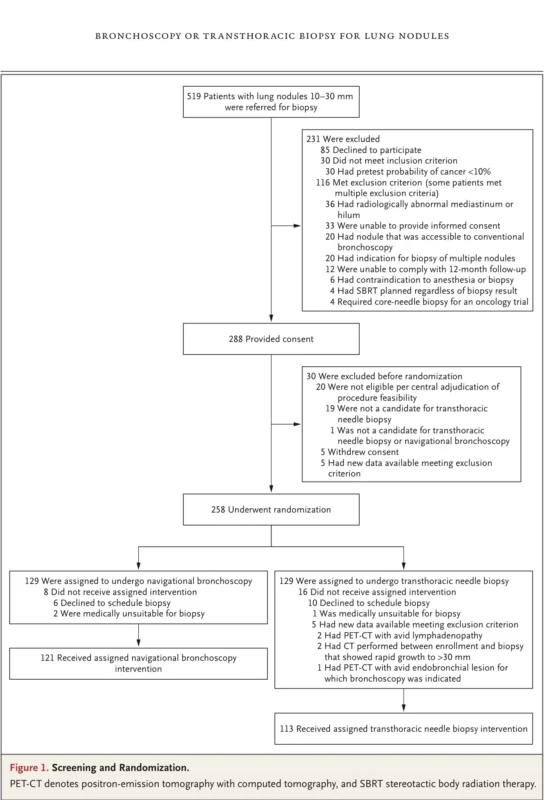
A total of 519 patients were screened, of whom 288 provided written informed consent. After exclusions before randomization, 258 patients underwent randomization, with 129 assigned to navigational bronchoscopy and 129 assigned to transthoracic needle biopsy (Lentz et al., 2025).
For the primary outcome analysis, 121 patients in the bronchoscopy group and 113 patients in the transthoracic group were included. Five patients overall were lost to follow-up before complete primary outcome assessment, 2 in the bronchoscopy group and 3 in the transthoracic group (Lentz et al., 2025).
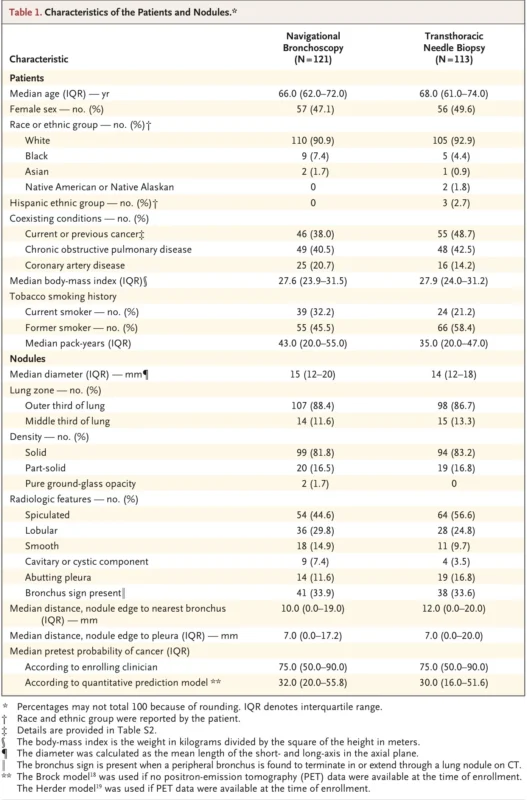
The baseline characteristics were well balanced. Median age was 66.0 years in the navigational bronchoscopy group and 68.0 years in the transthoracic needle biopsy group. Women represented 47.1% and 49.6% of the two groups, respectively. The median nodule size was 15 mm in the bronchoscopy group and 14 mm in the transthoracic group. Most nodules were solid, 81.8% and 83.2%, and most were located in the outer third of the lung, 88.4% and 86.7%, respectively (Lentz et al., 2025).
The bronchus sign was present in one third of patients in both groups, 33.9% versus 33.6%. Median clinician-estimated pretest probability of cancer was 75% in both groups, whereas median model-based pretest probability was 32.0% in the bronchoscopy group and 30.0% in the transthoracic group (Lentz et al., 2025).
Primary Outcome: Diagnostic Accuracy
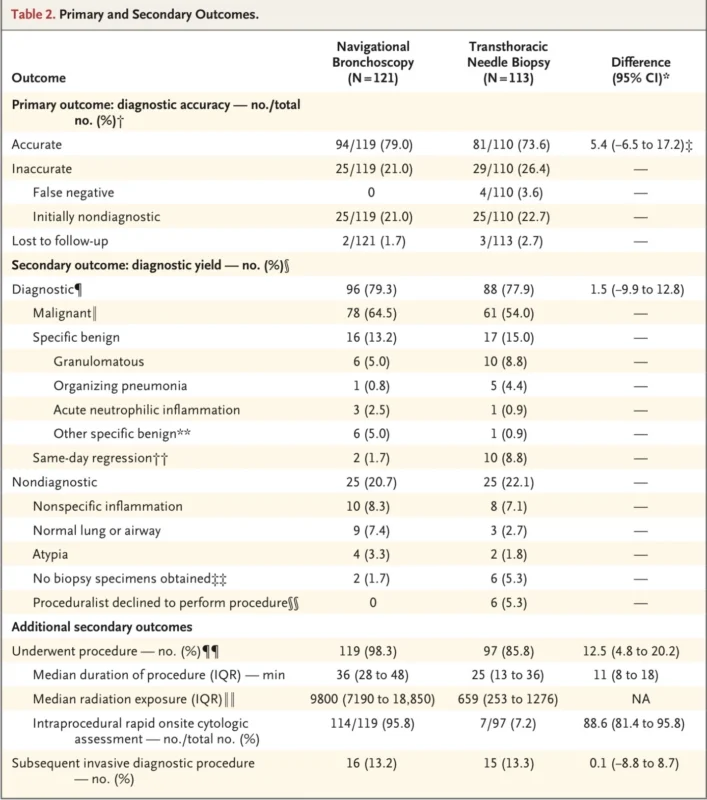
The central result of the study was straightforward. In the analysis of navigational bronchoscopy vs transthoracic needle biopsy for lung nodules, diagnostic accuracy was 79.0% in the navigational bronchoscopy group and 73.6% in the transthoracic needle biopsy group. The absolute difference was 5.4 percentage points, with a 95% confidence interval of −6.5 to 17.2. This met the criterion for noninferiority, with a P value of 0.003 for noninferiority, while superiority was not shown, with a P value of 0.17 (Lentz et al., 2025).
This means navigational bronchoscopy was not worse than transthoracic needle biopsy by more than the prespecified margin. In fact, the point estimate numerically favored bronchoscopy.
Through 12 months of follow-up, false-negative results occurred only in the transthoracic needle biopsy group, affecting 4 of 110 patients, or 3.6%. No patients in the navigational bronchoscopy group whose biopsy showed a specific benign diagnosis were later reclassified as malignant (Lentz et al., 2025).
The prevalence of cancer during follow-up was high in both groups, 74.8% in the bronchoscopy group and 69.1% in the transthoracic group, for an overall prevalence of 72.1% (Lentz et al., 2025).
Copyright © 2025 Massachusetts Medical Society
Secondary Outcomes
Diagnostic yield, which was defined without requiring follow-up confirmation, was also similar between the two procedures. It was 79.3% with navigational bronchoscopy and 77.9% with transthoracic needle biopsy, a difference of 1.5 percentage points (Lentz et al., 2025).
Among diagnostic results, malignant findings were reported in 64.5% of patients in the bronchoscopy group and 54.0% in the transthoracic group. Specific benign diagnoses were obtained in 13.2% and 15.0%, respectively. Nondiagnostic results occurred in 20.7% of the bronchoscopy group and 22.1% of the transthoracic group (Lentz et al., 2025).
An additional invasive diagnostic procedure after the trial biopsy was required in 13.2% of patients in the bronchoscopy group and 13.3% in the transthoracic group. Subsequent invasive staging procedures were uncommon in both groups, 0% and 2.7%, respectively (Lentz et al., 2025).
Procedure time was longer for bronchoscopy, with a median duration of 36 minutes compared with 25 minutes for transthoracic biopsy. Rapid on-site cytologic assessment was used in 95.8% of bronchoscopy procedures but in only 7.2% of transthoracic biopsies (Lentz et al., 2025).
Copyright © 2025 Massachusetts Medical Society
Safety: A Major Difference Between The Two Approaches
The most striking separation in navigational bronchoscopy vs transthoracic needle biopsy for lung nodules was safety.
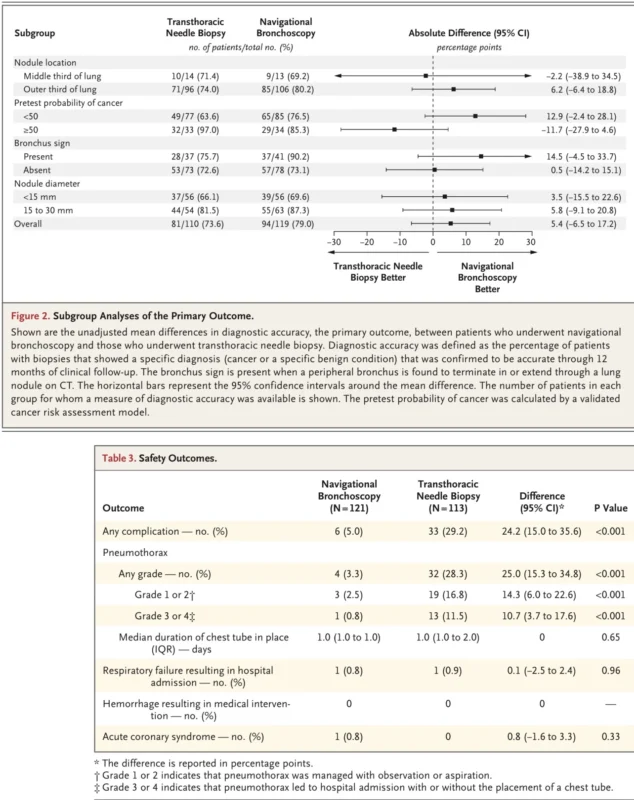
Any procedural complication occurred in 5.0% of patients undergoing navigational bronchoscopy versus 29.2% of those undergoing transthoracic needle biopsy. That corresponds to an absolute risk difference of 24.2 percentage points (95% CI, 15.0 to 35.6; P<0.001) (Lentz et al., 2025).
Pneumothorax was the dominant complication. It occurred in 3.3% of the bronchoscopy group and 28.3% of the transthoracic group, a 25.0 percentage point difference. Pneumothorax severe enough to require a chest tube, hospital admission, or both occurred in 0.8% of bronchoscopy patients and 11.5% of transthoracic patients, for an absolute difference of 10.7 percentage points.
These are not small differences. They represent a clinically meaningful safety advantage for navigational bronchoscopy. No hemorrhage requiring medical intervention occurred in either group, and there were no deaths during the 12-month follow-up period.
Subgroup Findings
The investigators also explored whether the effect of biopsy method differed according to prespecified baseline features. These included nodule location, pretest probability of cancer, nodule diameter, and the presence or absence of a bronchus sign.
No subgroup clearly modified the main effect. For example, among nodules in the outer third of the lung, diagnostic accuracy was 80.2% with navigational bronchoscopy and 74.0% with transthoracic needle biopsy. Among nodules 15 to 30 mm in size, diagnostic accuracy was 87.3% versus 81.5%. In nodules with a bronchus sign, diagnostic accuracy was 90.2% versus 75.7%. Although these differences numerically favored bronchoscopy in several subgroups, the trial was not powered for definitive subgroup superiority conclusions, and no interaction clearly changed the overall interpretation (Lentz et al., 2025).
How To Interpret These Results
The VERITAS trial changes the discussion around navigational bronchoscopy vs transthoracic needle biopsy for lung nodules because it replaces indirect comparison with randomized evidence. The key message is not that transthoracic biopsy is ineffective. Rather, it is that modern navigational bronchoscopy, when performed in experienced centers and with contemporary imaging support, can achieve similar diagnostic accuracy while exposing patients to far fewer complications.
This matters most in the setting studied here: peripheral pulmonary nodules measuring 10 to 30 mm that are technically suitable for either procedure. In that situation, the older assumption that transthoracic biopsy is the more accurate default option becomes less convincing when weighed against its substantially higher pneumothorax burden.
The authors also point out that prior transthoracic biopsy series often reported higher performance, but those estimates came largely from retrospective or noncomparative studies with greater potential for bias. The relatively small median nodule size in VERITAS, 15 mm, may also have contributed to somewhat lower accuracy in the transthoracic arm compared with historical data (Lentz et al., 2025).
Copyright © 2025 Massachusetts Medical Society
Limitations
Several limitations should be acknowledged. Navigational bronchoscopy was performed by experienced interventional pulmonologists, so results may not translate directly to settings with less expertise. The study was open label, although outcome adjudication was blinded. Patients with nodules not amenable to both procedures were excluded, as were nodules in the inner third of the lung, so the findings apply primarily to lesions technically feasible for either approach. Rapid on-site cytology was much more common in the bronchoscopy arm, which may have influenced results, although the magnitude of that effect is uncertain (Lentz et al., 2025).
Even with these limitations, the randomized design, low loss to follow-up, central adjudication of procedural feasibility, and 12-month confirmation of diagnosis make VERITAS a highly influential trial.
Conclusion
The VERITAS trial provides the strongest evidence to date on navigational bronchoscopy vs transthoracic needle biopsy for lung nodules. Among patients with peripheral pulmonary nodules 10 to 30 mm in size that were suitable for both procedures, navigational bronchoscopy achieved diagnostic accuracy of 79.0%, compared with 73.6% for transthoracic needle biopsy, meeting criteria for noninferiority. At the same time, complications were far less frequent with bronchoscopy, especially pneumothorax, which occurred in 3.3% versus 28.3% of patients, respectively.
For thoracic oncology and pulmonary teams, the practical implication is clear: when both procedures are technically feasible, navigational bronchoscopy deserves serious consideration as the preferred first diagnostic approach because it preserves accuracy while markedly improving safety.


