The relationship between cannabis smoking and lung cancer has remained difficult to define for decades. Much of that uncertainty comes from two major issues: cannabis has historically been illegal in many countries, limiting high-quality prospective research, and most people who smoke cannabis also smoke tobacco, making it difficult to separate the effects of one exposure from the other. As cannabis use becomes more common worldwide, especially among younger adults, this gap in knowledge is becoming increasingly important in thoracic oncology.
A new prospective multicenter French study now offers some of the clearest data yet on dual cannabis and tobacco smoking in young patients with lung cancer. By combining self-reported smoking history with hair toxicology analysis, investigators evaluated 150 patients aged 60 years or younger who were consecutively diagnosed with primary lung cancer between 2021 and 2023. The findings show that dual cannabis and tobacco smoking in young patients with lung cancer is common and is associated with a distinct clinical pattern, including more emphysema, poorer gas exchange, and a higher proportion of rare and aggressive tumor subtypes compared with patients who smoked tobacco alone (Pradère et al., 2026).
Why This Study Matters
Cannabis smoke contains known carcinogens, including benzopyrene, benzanthracene, and fine particulate matter, and prior research has suggested that smoking cannabis may induce bronchial molecular and histopathologic changes linked to carcinogenesis (Pradère et al., 2026). At the same time, older meta-analyses failed to establish a clear association between cannabis smoking and lung cancer, largely because of inconsistent exposure assessment and heavy overlap with tobacco smoking (Pradère et al., 2026). That has contributed to a persistent perception that cannabis is safer than tobacco, even though combustion of any inhaled material carries pulmonary risk.
This study is important because it addresses that problem more rigorously than many earlier reports. The investigators did not rely only on questionnaires. They also measured nicotine, cotinine, tetrahydrocannabinol, and cannabidiol in hair samples, allowing them to biologically validate smoking exposure. That makes this one of the more informative datasets on dual cannabis and tobacco smoking in young patients with lung cancer currently available (Pradère et al., 2026).
Study Population And Exposure Groups
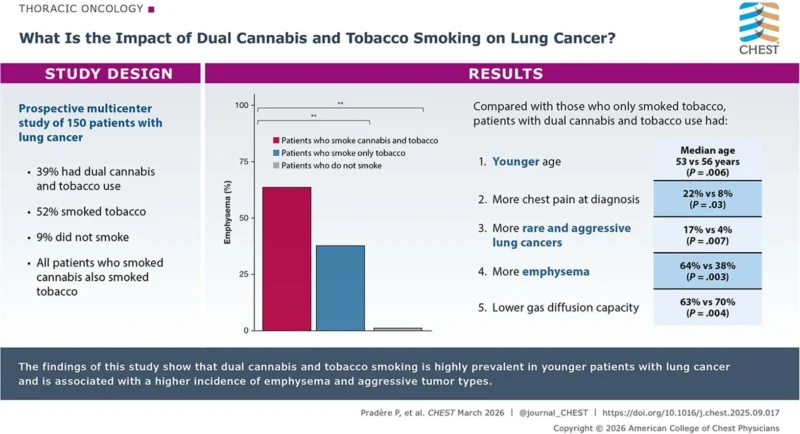
The study included 150 patients aged 18 to 60 years with primary lung cancer treated at three French hospitals. Two patients did not complete the smoking questionnaire and were excluded from statistical analysis, leaving 148 evaluable patients (Pradère et al., 2026).
Patients were divided into three groups. The first group included patients who smoked both cannabis and tobacco, defined as smoking at least 10 joints per month for at least 1 year and at least 1 pack-year of tobacco. The second group included patients who smoked only tobacco. The third group included patients who essentially never smoked either product (Pradère et al., 2026).
Among the 148 evaluable patients, 56 initially reported regular cannabis smoking. Hair testing then identified two additional patients with tetrahydrocannabinol concentrations incompatible with passive exposure, leading to reclassification. The final distribution was 39% patients who smoked cannabis and tobacco, 52% patients who smoked only tobacco, and 9% patients who did not smoke (Pradère et al., 2026). In other words, nearly four in ten cases in this young cohort involved dual cannabis and tobacco smoking in young patients with lung cancer.
All cannabis users in this study also smoked tobacco. There were no cannabis-only smokers, which reflects current real-world smoking patterns in the studied population but also limits the ability to isolate the independent effect of cannabis.
Cannabis Exposure Was Heavy And Longstanding
Cannabis use in the combined-smoking group was substantial. Median cannabis use duration was 26 years, and median consumption was 4 joints per day. Among these patients, 14% smoked cannabis leaves only, 30% smoked resin, and 56% smoked a mixture of both, all combined with tobacco in spliffs (Pradère et al., 2026).
Importantly, tobacco exposure appeared similar between patients who smoked cannabis and tobacco and those who smoked tobacco alone. Median tobacco smoking duration was 35 years in the combined-smoking group and 34 years in the tobacco-only group. Median pack-years were also close, 31 versus 29, respectively (Pradère et al., 2026). That point matters because it suggests the differences observed in dual cannabis and tobacco smoking in young patients with lung cancer may not simply be explained by heavier tobacco exposure.
Hair Toxicology Strengthened Exposure Assessment
Hair analysis supported the smoking history data. Tetrahydrocannabinol was detected in 57% of patients who smoked cannabis and tobacco, compared with 8% of tobacco-only smokers and none of the never-smokers. Cannabidiol was detected in 47% of patients who smoked cannabis and tobacco, 3% of tobacco-only smokers, and 8% of never-smokers (Pradère et al., 2026).
For tobacco-related compounds, nicotine was detected in 83% of combined smokers, 79% of tobacco-only smokers, and 69% of never-smokers. Cotinine, which is more informative for active tobacco exposure, was detected in 81% of combined smokers, 60% of tobacco-only smokers, and 31% of never-smokers. Median cotinine concentrations did not significantly differ between the combined-smoking group and the tobacco-only group, again supporting the idea that tobacco exposure was broadly comparable (Pradère et al., 2026).
This is one of the most useful aspects of the paper. The data suggest that the distinct features seen in dual cannabis and tobacco smoking in young patients with lung cancer are unlikely to be explained only by higher nicotine exposure.
Patients Were Younger And More Symptomatic
The clinical profile of patients with combined smoking differed meaningfully from that of tobacco-only smokers. Median age at diagnosis was 53 years in the combined-smoking group versus 56 years in the tobacco-only group, a statistically significant difference (Pradère et al., 2026).
Thoracic pain at diagnosis was also more common in combined smokers, reported by 22% of patients compared with 8% in tobacco-only smokers and 8% in never-smokers (Pradère et al., 2026). The authors suggest that this could reflect either delayed diagnosis or a more aggressive disease phenotype.
Body mass index was lower in the combined-smoking group, and inflammatory markers also showed some differences. Median leukocyte count was 9.7 G/L in combined smokers, 8.7 G/L in tobacco-only smokers, and 5.7 G/L in never-smokers. Median neutrophil counts followed a similar pattern, although the clinical meaning of these differences remains uncertain.
Emphysema And Impaired Gas Exchange Were More Common
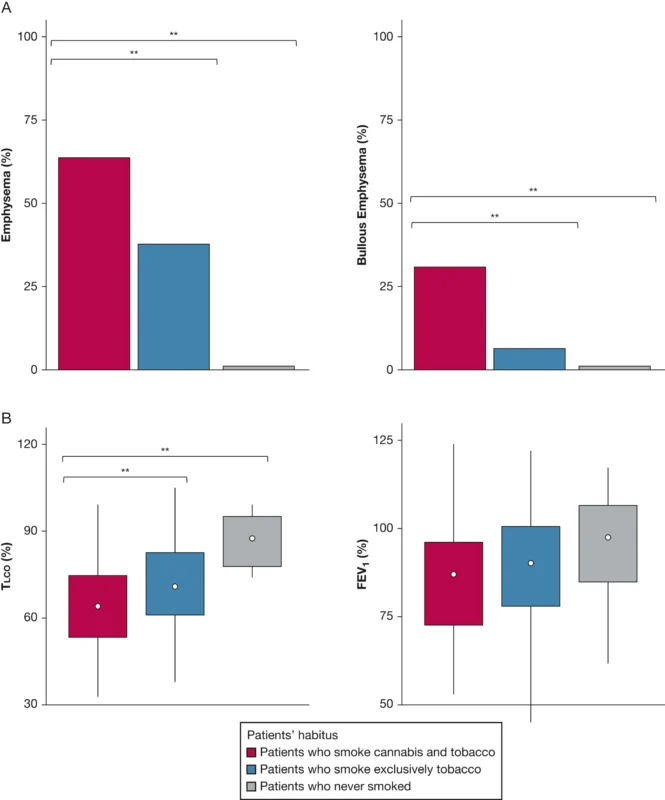
One of the strongest findings was the much higher burden of emphysema in the combined-smoking group. Emphysema was present in 64% of patients who smoked cannabis and tobacco, compared with 38% of tobacco-only smokers and none of the never-smokers. Bullous emphysema was identified in 31% of combined smokers but only 7% of tobacco-only smokers (Pradère et al., 2026).
Upper-lobe predominance of emphysema was also more common in combined smokers, seen in 55% of them versus 32% in tobacco-only smokers (Pradère et al., 2026). These radiologic differences are highly relevant because they suggest that dual cannabis and tobacco smoking in young patients with lung cancer may be associated with more severe structural lung damage than tobacco smoking alone.
Pulmonary function findings supported that impression. Median transfer capacity for carbon monoxide was 63% in combined smokers, compared with 71% in tobacco-only smokers and 88% in never-smokers. In contrast, FEV1 did not significantly differ between groups, with medians of 85%, 88%, and 98%, respectively (Pradère et al., 2026). This pattern suggests that the major difference may lie more in gas exchange impairment than in airflow limitation.
Tumor Histology Appeared More Aggressive
The study also found differences in tumor type. Adenocarcinoma remained the most common histology overall, but it was less frequent in combined smokers and tobacco-only smokers than in never-smokers, occurring in 72%, 71%, and 92% of cases, respectively (Pradère et al., 2026).
Most importantly, rare histologic subtypes were significantly more common in combined smokers. Sarcomatoid carcinoma and poorly differentiated large cell carcinoma together accounted for 17% of tumors in the combined-smoking group, compared with 4% in tobacco-only smokers and none in never-smokers (Pradère et al., 2026). These are generally considered more aggressive histologies, and this may be one of the strongest signals that dual cannabis and tobacco smoking in young patients with lung cancer is associated with a different oncologic phenotype.
Programmed death-ligand 1 expression did not significantly differ between groups (Pradère et al., 2026).
Molecular Findings Suggest A Distinct Genomic Pattern
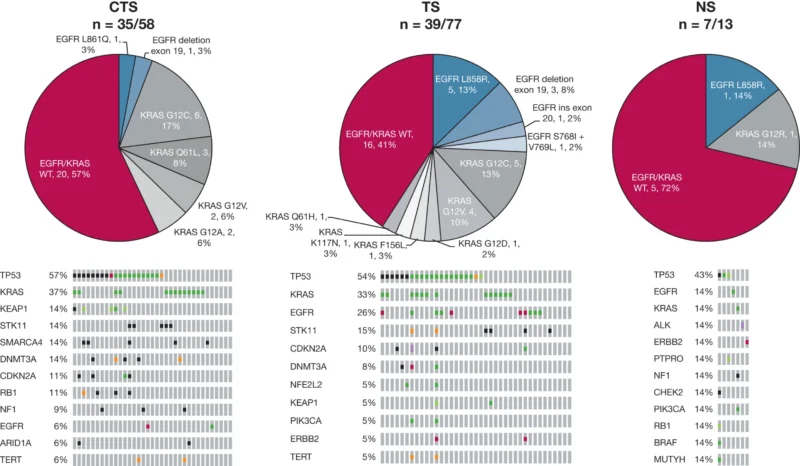
Molecular profiling was available in a subset of patients. Among those profiled, EGFR mutations were less frequent in combined smokers than in tobacco-only smokers, 5.7% versus 25.6%. By contrast, SMARCA4 mutations were more frequent in combined smokers, 14% versus 0% (Pradère et al., 2026). KRAS mutation frequency appeared similar between the two groups.
These data should be interpreted carefully because the profiled subgroup was limited and testing methods were not fully uniform, but they raise the possibility that dual cannabis and tobacco smoking in young patients with lung cancer may also be associated with a distinct molecular landscape.
Surgery Appeared More Complex
Among patients who underwent surgery as first-line treatment, combined smokers had longer operative times, with a significant difference compared with tobacco-only smokers. They also showed a trend toward more extended resections, longer hospital stay, and more frequent nosocomial infections, although not all of these comparisons reached statistical significance (Pradère et al., 2026).
Median hospital stay after surgery was 7 days in combined smokers compared with 5 days in both tobacco-only smokers and never-smokers. Nosocomial infection occurred in 14% of combined smokers versus 5% of tobacco-only smokers and none of the never-smokers (Pradère et al., 2026). These results suggest that dual cannabis and tobacco smoking in young patients with lung cancer may influence perioperative complexity as well.
One-Year Follow-Up And Smoking Cessation
At one year after diagnosis, survival was similar across groups: 83% in combined smokers, 83% in tobacco-only smokers, and 92% in never-smokers, with no statistically significant difference (Pradère et al., 2026). Given the modest sample size and short follow-up, this result should not be interpreted as evidence of equal long-term prognosis.
Smoking cessation outcomes were more revealing. Among patients who were actively smoking at diagnosis, tobacco cessation at one year was achieved in 59% of combined smokers compared with 82% of tobacco-only smokers. Among combined smokers, 68% also reported quitting cannabis (Pradère et al., 2026). This suggests that dual cannabis and tobacco smoking in young patients with lung cancer may represent a particularly challenging group for addiction management after diagnosis.
What This Study Suggests
This prospective study does not definitively prove that cannabis independently causes lung cancer. The absence of a cannabis-only group means the effects of cannabis cannot be fully disentangled from those of tobacco. However, the findings do strongly suggest that dual cannabis and tobacco smoking in young patients with lung cancer is associated with a recognizable and clinically important phenotype: younger age at diagnosis, more emphysema, lower diffusing capacity, more rare aggressive histologies, and more complex surgical courses (Pradère et al., 2026).
The fact that tobacco exposure appeared similar between combined smokers and tobacco-only smokers strengthens the argument that cannabis may be contributing something beyond tobacco alone, whether through its own direct carcinogenic effect or through additive pulmonary toxicity.
Conclusion
The French prospective “Environment and Lung Cancer” study offers one of the clearest descriptions to date of dual cannabis and tobacco smoking in young patients with lung cancer. In this cohort of patients aged 60 years or younger, 39% had a history of regular combined smoking. Compared with tobacco-only smokers, these patients were younger at diagnosis, more likely to report chest pain, had more emphysema and bullous changes, lower transfer capacity, and a greater proportion of rare and aggressive tumor types (Pradère et al., 2026).
For thoracic oncology, the message is increasingly difficult to ignore. Cannabis smoking should no longer be treated as an anecdotal detail in young patients with lung cancer. It deserves systematic assessment, more rigorous prospective study, and greater attention in clinical counseling and multidisciplinary care.
Read full article here


