Muna Al-Khaifi, Lead of Breast Cancer Survivorship Program and GP Oncologist at the Mount Sinai Hospital (Toronto), Sinai Health, presents this article on the development of a system-level framework aimed at standardizing survivorship care across Ontario. This piece outlines the need to reduce variability in care delivery and strengthen coordinated, evidence-informed survivorship services for individuals living with and beyond cancer.
Improving Cancer Survivorship Care in Ontario, Canada – Development and Launch of a New Quality Standard for Cancer Survivorship
Despite major advances in cancer treatment, survivorship care remains inconsistent-varying across providers, institutions, and regions. This variability reflects a fundamental gap: we have strong evidence, yet we have not consistently translated it into standardized, system-wide care. To address this, Ontario Health developed a Cancer Survivorship Quality Standard, designed to define what high-quality survivorship care should look like across Ontario.
It was a privilege to serve as a co-chair of this initiative, working alongside a multidisciplinary advisory committee of clinicians, allied health professionals, and individuals with lived experience. This work reinforced a critical reality: survivorship care is not a single intervention-it is a coordinated, system-level responsibility.
Improving Cancer Survivorship Care in Ontario, Canada – Development and Launch of a New Quality Standard for Cancer Survivorship.
Why a Quality Standard Matters
Quality standards are designed to define what high-quality care looks like, reduce variation in care delivery, and support measurement and accountability across the health system.
In survivorship, this is particularly important. As more individuals live longer after cancer, many continue to experience long-term and late effects of treatment-including physical symptoms, psychological challenges, and functional limitations. Yet care has historically been fragmented, reactive, and inconsistent.
A quality standard provides a shared framework to align care delivery across providers and settings-ensuring that survivorship care is not dependent on where a patient is seen, but guided by consistent expectations of quality.
A Rigorous, Evidence-Informed Process
The development of this quality standard followed a structured, multi-phase, evidence-informed approach.
This included a multidisciplinary advisory committee, a comprehensive review of the literature and existing data, expert consultation to identify priority areas, and multiple structured consensus meetings to refine quality statements and indicators. Public consultation-through surveys, written feedback, and focus groups-ensured that patient, caregiver, and clinician perspectives were incorporated.
Strong consensus was achieved across stakeholders, ensuring that the final standard reflects both evidence and real-world practice.
Scope of the Quality Standard
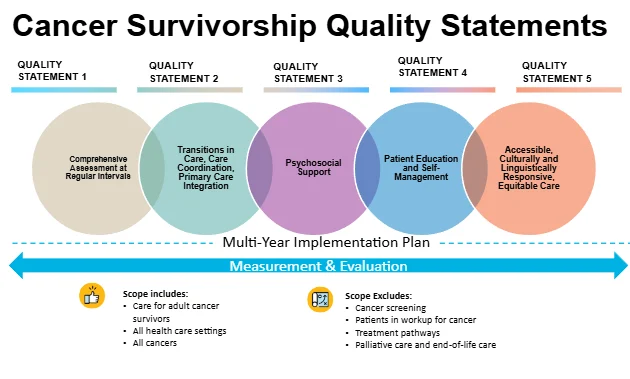
This quality standard applies to adults living with, through, and beyond a cancer diagnosis across all cancer types and all healthcare settings in Ontario, including oncology, primary care, emergency departments, long-term care, and home and community care. It is inclusive of individuals receiving prolonged therapy, those living with chronic or metastatic disease, and long-term survivors.
The standard focuses on the assessment, management, and follow-up care of cancer survivors, with the goal of supporting overall health, function, and quality of life across the continuum.
It does not address cancer screening, diagnostic workup, active treatment pathways, palliative care, or end-of-life care. Instead, it complements these areas by emphasizing the early and ongoing integration of survivorship care to support long-term wellness and proactive management of physical, psychological, and social needs.
Five Focus Areas That Define High-Quality Survivorship Care
The quality standard identifies five core domains that together define high-quality survivorship care across the cancer continuum.
1-Comprehensive Assessment at Regular Intervals
Survivorship care should include structured and ongoing assessment of physical, psychological, and functional needs, as well as late and long-term effects of cancer and its treatment. This reflects a shift from reactive symptom management to proactive, needs-based care embedded within routine follow-up.
2-Transitions in Care, Care Coordination, and Primary Care Integration
Effective survivorship care depends on seamless transitions between oncology, primary care, and community-based services. This domain emphasizes the importance of clear communication, defined roles, and coordinated care pathways to reduce fragmentation and ensure continuity.
3-Psychosocial Support
Psychological and social well-being are central components of survivorship care. Many individuals experience distress, anxiety, depression, and fear of recurrence, yet these needs often remain under-recognized. This domain highlights the importance of proactively identifying and addressing psychosocial needs.
4-Patient Education and Self-Management
Patients should be supported with clear, accessible information about their condition, expected symptoms, and when to seek care. Education enables individuals to engage in self-management and participate more actively in their care, improving both experience and outcomes.
5-Accessible, Culturally and Linguistically Responsive, Equitable Care
High-quality survivorship care must be inclusive and responsive to diverse populations. This includes addressing disparities in access, ensuring care is culturally and linguistically appropriate, and designing systems that support equitable outcomes for all patients.
From Framework to Practice: A Multi-Year Implementation Approach
The Cancer Survivorship Quality Standard is designed not as a single intervention, but as a multi-year implementation effort supported by ongoing measurement and evaluation.
Implementation will involve translating quality statements into practice across diverse care settings, supported by clinician guidance, patient resources, and system-level tools. A structured measurement framework-combining overarching measures and statement-specific indicators-will enable monitoring of progress, identification of variation, and continuous quality improvement.
This approach recognizes that meaningful change in survivorship care requires time, coordination, and alignment across providers and organizations. Progress will depend on integrating these standards into existing workflows, strengthening collaboration between oncology and primary care, and leveraging community-based resources.
Ultimately, the goal is to move from defining high-quality survivorship care to consistently delivering it across the health system.
The Cancer Survivorship Quality Standard provides a critical foundation for improving care.
But defining quality is only the beginning.
The future of survivorship care will depend on how these principles are implemented, sustained, and integrated into everyday practice—ensuring that every individual living with and beyond cancer receives care that is comprehensive, coordinated, and equitable.
You can also read: Muna Al-Khaifi: Vasomotor Symptoms and Treatment Adherence in Cancer Survivorship



