Mali Barbi, Medical Oncologist at Northwell Health, shared a post on X:
“ctDNA vs second-look laparoscopy for MRD detection in ovarian cancer. Clark et al. Abstract N207.
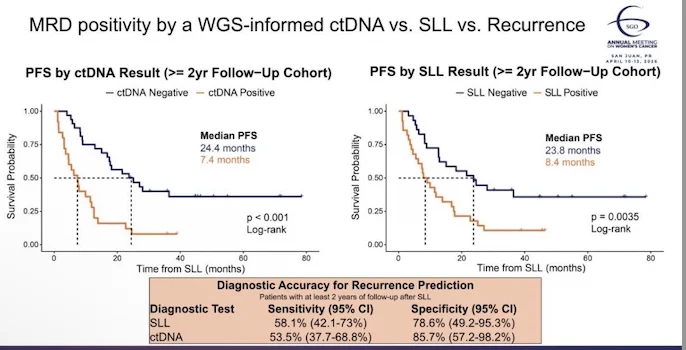
ctDNA positive: median PFS 7.4 months.
ctDNA negative: 24.4 months.
SLL positive: median PFS 8.4 months.
SLL negative: 23.8 months. Both are prognostic.
The survival separation is nearly identical. But the diagnostic properties are not.
SLL sensitivity 58.1%, specificity 78.6%.
ctDNA sensitivity 53.5%, specificity 85.7%.
SLL finds more disease. ctDNA is more specific – fewer false positives.
This matters because these tools are not competing for the same job anymore. Second-look laparoscopy was abandoned because detecting residual disease did not change outcomes. There was nothing to do with the information. That calculus has changed.
We now have maintenance strategies, PARP inhibitors, bevacizumab, immunotherapy, that may perform differently depending on MRD status. The question is no longer just whether disease is present. It is whether the answer should change what you do next. ctDNA cannot replace SLL on sensitivity. But it is non-invasive, repeatable, and longitudinal-exactly what we need to embed in clinical trial designs and escalation/de-escalation strategies.
Pre-test probability in gynecologic cancers is distinct. Do not import ctDNA interpretation frameworks from breast or colorectal cancer and apply them here. The field needs prospective trials that treat ctDNA status as a decision node, not just a prognostic marker. That is the next step.”
More posts featuring Mali Barbi.


