Breast Cancer in Young Women Foundation (BCYW Foundation) shared a post on LinkedIn:
“Breaking the Myths is a new science-centered educational series from the Breast Cancer in Young Women Foundation (BCYW Foundation) that sets out to separate fact from myths about breast cancer in young women.
Each article addresses a common myth, provides evidence-based information, highlights the value of early detection, and serves as a resource for proactive self-breast health care. This series aims to empower young women with accurate knowledge, encourage proactive screening, and foster conversations that can save lives.
In Article 7, we examine the myth about inflammatory breast cancer in young women: why this fast-spreading disease is often missed and misdiagnosed.
Inflammatory Breast Cancer in Young Women: Why This Fast-Spreading Disease Is Often Missed and Misdiagnosed
Reframing rapid progression, aggressive biology, and diagnostic delays in one of the most aggressive forms of breast cancer
Rakesh Kumar, PhD¹; Naoto T. Ueno, MD, PhD, FACP²
¹ Founder and CEO, Breast Cancer in Young Women Foundation, USA; ² Professor and Director, NCI-Designated University of Hawaii Cancer Center, USA. Author details are provided at the end of this article.
Breast cancer awareness has long been built around a simple narrative: A lump appears. It grows slowly. It is detected. It is treated.
This model has saved lives, but it does not apply to all cases of breast cancer.
Core Misunderstandings
- Breast cancer typically presents as a lump
- If it resembles an infection, it is not cancer
- Young women are not at a meaningful risk
- Cancer develops slowly
Inflammatory Breast Cancer (IBC) Does not Follow the Rules
In young women, this mismatch between biology and expectations is one of the most important reasons for the continued oversight of the disease.
Inflammatory breast cancer accounts for only 1–5% of all breast cancers; however, it contributes disproportionately to mortality due to its aggressive progression and early tendency to metastasize (1-4). It is now more widely understood not only as a clinical presentation but also as a unique clinicopathological and molecular entity (5, 6). Unlike typical breast cancers, IBC presents as:
- Often presents without a discrete lump
- Manifests as skin changes rather than a palpable mass
- Disseminates early via lymphovascular channels
- Tumor emboli within dermal lymphatic vessels
- Progresses over weeks rather than months or years
These are not late features but are essential for disease initiation and progression (5-8). Common symptoms fundamental to the disease’s biology include:
- Diffuse redness (erythema)
- Swelling (edema)
- Skin thickening (peau d’orange)
- Warmth and tenderness

Why Is Inflammatory Breast Cancer Often Missed in Young Women?
It does not present as a lump; most awareness messages still focus on feeling a lump. Because there is no distinct mass, both patients and clinicians may not immediately suspect cancer. It mimics common benign conditions, resembling the following:
- Mastitis
- Allergic reactions
- Dermatologic conditions
- Skin infections
These diagnoses are far more common in young women, especially those who are pregnant, postpartum, or breastfeeding. Hence, IBC is often initially treated as lactational changes or an infection, delaying the correct diagnosis.
There is a longstanding assumption that breast cancer is uncommon in young women, which results in the following:
Age bias in clinical decision-making
Lower initial suspicion
Delayed imaging or biopsy
Reassurance instead of escalation
Clinical evaluation should not always be age-driven but rather symptom-driven.
Rapid Disease Progression Creates A False Timeline — the Biology Behind the Illusion
Inflammatory breast cancer progresses rapidly, often within weeks rather than months. However, this swift progression is not coincidental; it indicates a specific tumor biology and underlying pathophysiology (2-7).
- High proliferative index (often elevated Ki-67), indicating rapid tumor cell division
- Frequent association with aggressive molecular subtypes (HER2-positive or triple-negative)
- Early and extensive dermal lymphatic invasion, with tumor emboli obstructing lymphatic channels in the skin
This lymphovascular obstruction leads to:
- Rapid onset of erythema, edema, and skin thickening
- Increased interstitial fluid pressure and inflammatory signaling
- IBC behaves more like a localized tumor than an infection.
- A clinical picture that mimics infection but is actually due to tumor-driven lymphatic dysfunction
Rapid progression is a biological signature—not incidental, and a clinical anomaly
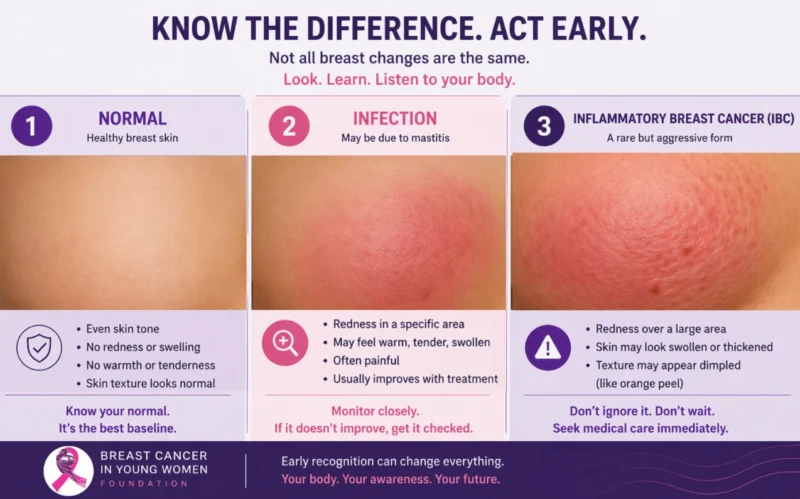
Inflammation Without Infection
The “inflammatory” phenotype of IBC is frequently misinterpreted. The “inflammatory” phenotype of IBC results from tumor-induced lymphatic obstruction as well as cytokine signaling; thus, the inflamed appearance is caused not only by obstruction but also by these signaling processes. Dermal lymphatic invasion contributes to many of these features. (5-9):
- Impaired lymphatic drainage
- Interstitial fluid accumulation
- Increased hydrostatic pressure
- Tumor cells activate cellular molecules that promote inflammation and invasion
The net result is a clinical picture that resembles inflammation but is actually caused by dysregulation of the vascular and immune systems associated with malignancy.
Understanding Why This Causes The False Timeline Bias and Adds To Diagnostic Confusion
Ironically, this aggressive biology produces a timeline that contradicts the traditional expectations of cancer.
- Patients think that cancer does not develop this quickly.
- Providers think: let us treat this as an allergic reaction, infection, or mastitis first, and then reassess.
- Disseminates early through lymphatics rather than forming a localized tumor
- May bypass the “detectable lump phase” entirely
- Can progress significantly within short periods, while under clinical observation
The assumption that serious diseases must evolve slowly. The opposite holds.
Potential Imaging Limitations
Traditional imaging methods may have limitations in detecting IBC (11, 12), and may not be clearly visible on mammography, and may fail to identify a discrete mass, instead showing the following:
- Skin thickening
- Trabecular distortion
- Diffuse density
Thus, MRI mammography and breast US, in addition to mammography, may be needed. A definitive diagnosis may require a core biopsy and skin punch biopsy to show dermal lymphatic invasion.
IBC diagnosis often requires clinical suspicion and biopsy, rather than imaging alone.
Reframing the Myth
One of the most persistent myths in breast cancer awareness is that breast cancer always develops slowly. Inflammatory breast cancer challenges this assumption at its core.
- It is not simply a slow-growing disease that was overlooked
- It is a rapidly progressing disease that is often misunderstood.
- IBC can evolve differently, more aggressively, and faster than expected.
For young women, inflammatory breast cancer is often missed, not because it is invisible, but because it does not always match the traditional image of breast cancer. Its symptoms can appear suddenly, progress quickly, and resemble infection or inflammation rather than a typical breast lump. This is why awareness, timely evaluation, and clinical suspicion are so important.
A Thought to Carry
Inflammatory breast cancer is not invisible. It is misinterpreted. It is neither slow nor silent. It is fast and deceptive. When breast cancer progresses too quickly to be believed, it is often because our models of disease have not kept pace with its biology.
About the Authors
Rakesh Kumar, PhD, is the founder and CEO of the Breast Cancer in Young Women Foundation (USA) and holds an International Endowed Chair Professorship at the Cancer Research Institute, SRHU, India. He also holds Adjunct and Visiting Professorships at Rutgers NJ Medical School, VCU School of Medicine, USA, and Medanta Cancer Institute, India. Throughout his 40-year career, he has held multiple roles, including tenured professor, endowed distinguished professor, department vice chair and chair, endowed chair, and various institutional research and academic leadership positions at leading institutions in the USA, including about 20 years at the University of Texas MD Anderson Cancer Center and Memorial Sloan-Kettering Cancer Center. He has also held the Govt of India DBT National Chair in Cancer Research with a Distinguished Professorship. He has contributed significantly to cancer biology, particularly in estrogen, growth factors, and kinase signaling.
Naoto T. Ueno, MD, PhD, FACP, serves as Director and Professor of Medicine at the University of Hawaii Cancer Center, which is designated by the NCI. He previously led the MD Anderson Inflammatory Breast Cancer (IBC) Research Program and Clinic, establishing the world’s largest and most well-known program for this rare and aggressive disease. His leadership promotes collaborative, multidisciplinary innovation and fosters diversity, psychological safety, and high productivity in clinical care, research, and education. Dr. Ueno’s research concentrates on the molecular mechanisms driving aggressive breast cancers, especially triple-negative breast cancer (TNBC) and IBC. An esteemed educator and mentor, he teaches leadership and clinical research worldwide, has spoken at TEDx, and authored books on patient empowerment.
About the Series
Breaking the Myths is a new educational series from the Breast Cancer in Young Women Foundation (BCYW Foundation) that sets out to separate fact from myths about breast cancer in young women. Each article addresses a common myth, provides evidence-based information, highlights the value of early detection, and serves as a resource for proactive self-breast health care. This series aims to empower young women with accurate knowledge, encourage proactive screening, and foster conversations that can save lives.
About the BCYW Foundation
The BCYW Foundation is a leading global organization dedicated solely to breast cancer in young women. Founded three years ago, it brings together a diverse network of scientists, oncologists, surgeons, survivors, NGOs, and partners from 35 countries. The foundation is expanding its targeted awareness and research efforts and sharing emerging BCYW advances through its peer-reviewed, open-access Journal of Young Women Breast Cancer and Health.
Adrian Waller Keshav K Singh, PhD Michael Gnant Miguel Martín Dr. Shelly Sharma Marie-Jeanne Vrancken Peeters”
Other articles featuring BCYW Foundation on OncoDaily.


