A recent study published in Radiotherapy and Oncology adds meaningful evidence to the ongoing discussion around prostate-directed radiotherapy in men with de novo metastatic prostate cancer. Using data from the National Cancer Database, investigators examined whether adding prostate radiotherapy to hormonal therapy was associated with improved overall survival, and whether that association differed according to metastatic substage.
Their findings suggest that the benefit of local radiotherapy is not uniform across all patients with metastatic disease. Instead, survival outcomes appear to vary significantly depending on the extent and site of metastases.
Rethinking the Role of Local Therapy in Metastatic Prostate Cancer
The role of prostate radiotherapy in metastatic hormone-sensitive prostate cancer has evolved substantially over recent years. Earlier randomized data, including the HORRAD and STAMPEDE studies, suggested that radiotherapy to the primary tumor may provide benefit in selected patients with low metastatic burden. However, uncertainty has remained regarding which subgroups are most likely to benefit in routine clinical practice.
In particular, there has been limited contemporary evidence evaluating outcomes according to specific metastatic substages, such as non-regional nodal disease, bone metastases, and visceral involvement. This new analysis addresses that gap by focusing on the relationship between prostate radiotherapy and survival across M1a, M1b, and M1c disease.
Radiotherapy for Prostate Cancer: Types, Success Rate, Side Effects And More
A Large Contemporary Real-World Analysis
The investigators performed a retrospective cohort study using the U.S. National Cancer Database from 2004 to 2020. They identified 48,121 patients with newly diagnosed metastatic prostate cancer treated with hormonal therapy, either alone or in combination with prostate radiotherapy.
Of the total population, 42,437 patients received hormonal therapy alone, while 5,684 received hormonal therapy plus prostate radiotherapy. To reduce imbalances between the two groups, the authors used propensity score matching and multivariable Cox regression models.
The primary endpoint was overall survival.
Survival Impact of Prostate-Directed Radiotherapy
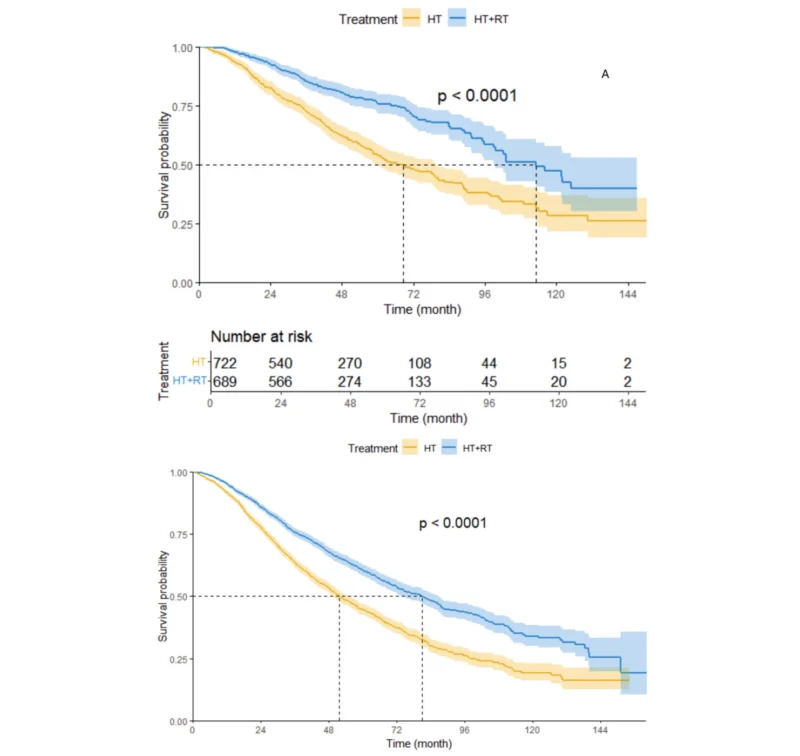
In the overall matched cohort, the addition of prostate radiotherapy was associated with improved overall survival. Median overall survival reached 84 months in patients treated with hormonal therapy plus radiotherapy, compared with 53 months in those treated with hormonal therapy alone. The adjusted hazard ratio for death was 0.62, indicating a substantial reduction in mortality risk associated with radiotherapy.
However, the most important finding of the study was that this association differed significantly by metastatic substage.
Among patients with M1a disease, defined as non-regional lymph node metastases, prostate radiotherapy was associated with the greatest apparent benefit. Median overall survival was 113.0 months with radiotherapy versus 68.4 months without it, with a hazard ratio of 0.48.
In patients with M1b disease, or bone metastases, radiotherapy was also associated with improved survival. Median overall survival was 81.0 months in the radiotherapy group compared with 51.8 months in the hormonal therapy alone group, with a hazard ratio of 0.60.
By contrast, among patients with M1c disease, meaning visceral metastases, no significant survival benefit was observed. Median overall survival was 40.3 months in the radiotherapy group and 43.4 months in the non-radiotherapy group, with a hazard ratio of 0.91.
These data suggest that prostate radiotherapy may be most relevant in patients with limited metastatic burden, particularly those with nodal-only metastatic spread.
Disease Burden as a Determinant of Therapeutic Benefit
This study is notable because it moves beyond the traditional broad distinction of “low-volume” versus “high-volume” metastatic disease. Instead, it highlights the potential clinical relevance of metastatic substage as a more refined way of identifying patients who may benefit from local treatment of the primary tumor.
The especially strong association seen in M1a disease is of particular interest. Patients with non-regional nodal metastases may represent an under-recognized population in whom prostate radiotherapy offers meaningful benefit. At the same time, the absence of a clear advantage in M1c disease suggests that local therapy is less likely to influence outcomes when visceral spread is present.
In the modern era of PSMA PET/CT imaging and intensified systemic therapy, these distinctions may become even more important. More precise staging is likely to improve patient selection and help clinicians decide when local treatment should be incorporated into a broader metastatic treatment strategy.
Evolving Adoption of Prostate Radiotherapy in Clinical Practice
The study also showed that the use of prostate radiotherapy increased over time. Between 2004 and 2020, radiotherapy utilization rose from 9.3% to 18.3%, with the sharpest increase occurring after 2018.
This trend likely reflects growing acceptance of prostate-directed radiotherapy following publication of key trial data and updates in clinical guidelines. It also mirrors increasing recognition that management of metastatic prostate cancer is becoming more individualized, rather than relying on systemic therapy alone for all patients.
Side Effects of Radiotherapy for Prostate Cancer: Risks and What to Know
Interpreting Observational Evidence: Strengths and Limitations
Despite its large scale and national scope, the study has the limitations inherent to retrospective observational research. The National Cancer Database does not capture all potentially relevant clinical details, including performance status, use of androgen receptor pathway inhibitors, PSMA PET/CT findings, cancer-specific survival, or exact extent of metastatic burden within each substage.
Although the authors used propensity score matching to reduce baseline differences, the possibility of residual confounding remains. Therefore, the results should be interpreted as showing association rather than definitive proof of causation.
Implications for Patient Selection and Future Research
This national analysis supports the growing body of evidence that prostate-directed radiotherapy may improve survival in selected patients with newly diagnosed metastatic prostate cancer. The benefit appears most pronounced in men with non-regional lymph node metastases and remains significant in those with bone metastases, while no meaningful survival improvement was observed in visceral metastatic disease.
The findings reinforce the importance of better patient selection and suggest that metastatic substage may be an important tool in refining treatment decisions. As imaging and systemic therapies continue to evolve, future prospective studies will be essential to clarify which patients are most likely to derive meaningful benefit from local radiotherapy.
Stay informed with more articles like this on OncoDaily.
Written by Nare Hovhannisyan, MD




