Early-onset colorectal cancer (EO-CRC; ≤50 years) is increasing in incidence and is frequently diagnosed at an advanced stage. In metastatic colorectal cancer with liver metastases, liver metastasectomy can be performed with curative intent, yet it remains unclear whether EO-CRC derives the same long-term benefit as average-onset colorectal cancer (AO-CRC; >50 years).
This multicenter Italian real-world study evaluated overall survival and progression-free survival in EO-CRC versus AO-CRC patients with liver metastases, stratified by whether they underwent curative-intent liver metastasectomy, and explored outcomes across key molecular subgroups.
The article was published in Clinical Colorectal Cancer (Articles in Press, Open Access) on February 16, 2026
Title: The impact of surgical resection in early onset colorectal cancer patients with liver limited disease
Authors: Andrea Pretta, Pina Ziranu, Francesca Bergamo, Andrea Bottelli, Federica Marmorino, Mariapaola Masiello, Stefano Mariani, Krisida Cerma, Filippo Ghelardi, Paolo Ciracì, Alessia Lancianese, Valeria Pusceddu, Eleonora Perissinotto, Alberto Giovanni Leone, Ada Taravella, Erika Cimbro, Gianluca Pretta, Riccardo Cerantola, Luca Papini, Clelia Donisi, Gianmarco Ricagno, Raffaele Squitieri, Riccardo Giampieri, Chiara Cremolini, Sara Lonardi, Filippo Pietrantonio, Mario Scartozzi.
Methods
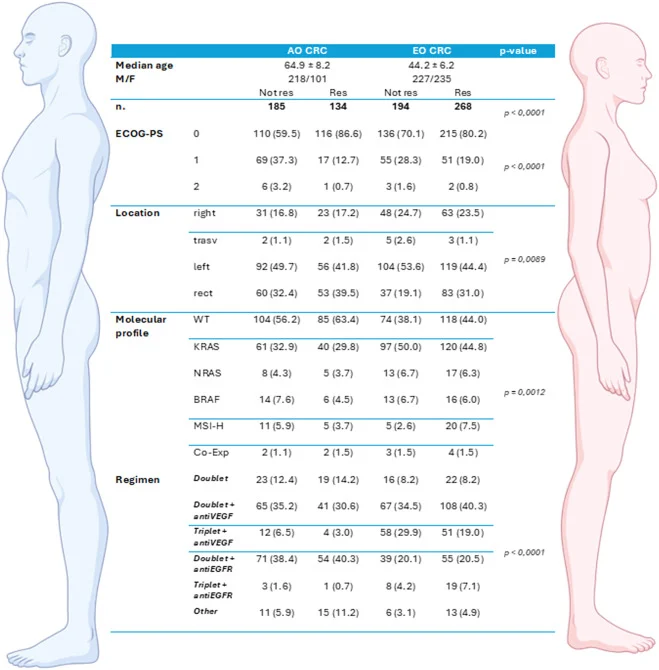
Investigators retrospectively collected data from five Italian institutions on 1,123 metastatic CRC patients diagnosed between 2008 and 2019, including 782 with liver-limited disease. Patients had ECOG performance status 0–2 and molecular profiling including KRAS/NRAS, BRAF, and dMMR/MSI-H (NGS available in 252 patients).
The main objective was to compare overall survival (OS) in EO-CRC versus AO-CRC patients with liver metastases, stratified by whether patients underwent curative-intent (R0) liver metastasectomy versus no resection.
Secondary analyses assessed progression-free survival (PFS) and outcomes within molecular subgroups (RAS-mutated, RAS/BRAF wild-type, and BRAF V600E). Survival was evaluated using Kaplan–Meier and log-rank testing, with Cox proportional hazards models including propensity-score inverse probability weighting (IPW) to address baseline imbalances.
Epidemiologic Context of Early-Onset Colorectal Cancer
Recent analyses of U.S. mortality data from 1990 to 2023 underscore a concerning trend in early-onset colorectal cancer (EO-CRC). Although overall cancer mortality among adults younger than 50 declined significantly over the past three decades, colorectal cancer emerged as the only major malignancy in this age group with rising death rates. Since 2005, colorectal cancer mortality has increased by approximately 1.1% annually, and by 2023 it had become the leading cause of cancer-related death in adults under 50.
Key signals highlighted in the report include:
- A 44% overall decline in cancer mortality among individuals under 50 — with colorectal cancer as the exception.
- A steady annual rise in colorectal cancer deaths since 2005 in this age group.
- Three in four younger patients diagnosed at an advanced stage.
- U.S. guidelines now recommend average-risk colorectal cancer screening starting at age 45, a relatively recent change.
- The possibility that early-onset colorectal cancer may represent a biologically distinct entity.
- The recognition that mortality trends are less susceptible to detection bias, reinforcing the validity of this signal.
Within this broader epidemiologic shift, evaluating outcomes after aggressive treatment strategies — including liver metastasectomy — becomes particularly relevant when interpreting survival patterns in early-onset colorectal cancer.
Results
Among patients with liver-limited disease, EO-CRC patients underwent metastasectomy more frequently than AO-CRC patients (268/462, 58% vs 134/319, 42%).
Metastasectomy was associated with longer survival in both age groups compared with no resection. However, EO-CRC consistently demonstrated inferior outcomes compared with AO-CRC after resection.
In resected patients:
- Median OS was 44.0 months in EO-CRC versus 64.0 months in AO-CRC (p < 0.0001).
- Median PFS was 13.0 months in EO-CRC versus 17.0 months in AO-CRC (p < 0.0001).
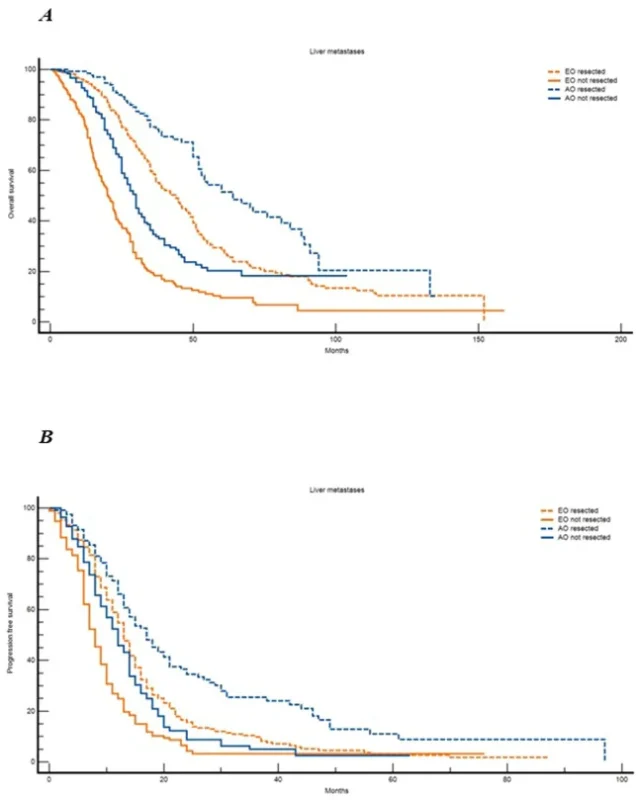
This survival gap persisted across molecular subgroups:
- RAS-mutated: mOS 37.0 vs 52.0 months (p < 0.0001), with mPFS 11.0 vs 13.0 months (p < 0.0001)
- RAS/BRAF wild-type: mOS 50.0 vs 81.0 months (p < 0.0001)
In the BRAF V600E subgroup (n = 49), EO-CRC patients who underwent metastasectomy showed longer OS than non-resected EO-CRC patients (17.1 vs 13.0 months, p = 0.047). In contrast, AO-CRC patients with BRAF mutation did not demonstrate a survival difference according to resection status (26.0 vs 27.0 months, p = 0.74).
Multivariable analysis confirmed early-onset disease as an independent adverse prognostic factor (adjusted HR 1.62, 95% CI 1.33–1.98). This association remained consistent after IPW adjustment (marginal HR 1.42; doubly robust HR 1.38). No significant interaction was observed between age group and RAS or BRAF status, with a borderline signal for MSI.
Genomic profiling further supported biological distinctions. EO-CRC tumors more frequently harbored TP53 alterations (56.2%) and less frequently APC mutations (29.9%) compared with AO-CRC (APC 54.0%, TP53 46.9%), and showed higher rates of ARID1A and CTNNB1 alterations.
Conclusion
In liver-limited metastatic colorectal cancer, liver metastasectomy was associated with longer survival in both EO-CRC and AO-CRC patients. However, early-onset disease remained consistently associated with inferior survival, even after curative-intent resection and across key molecular subgroups.
These findings suggest that EO-CRC may represent a more aggressive clinical and biological phenotype in the liver-limited metastatic setting and highlight the need for dedicated translational research and optimized multimodal strategies for younger patients.
The full article is available in Clinical Colorectal Cancer.