Precision oncology in advanced hormone receptor-positive, HER2-negative breast cancer increasingly depends on knowing not only which endocrine therapy a patient has received, but also which resistance pathways are active at progression. Among these, the PI3K/AKT/mTOR pathway has become one of the most clinically relevant, because activating PIK3CA mutations can identify patients eligible for PI3K pathway-directed treatment. A new Italian expert consensus published in The Breast now provides a practical framework for bringing PIK3CA testing into routine clinical practice, with recommendations covering tissue and liquid biopsy selection, analytical methods, reporting standards, timing of testing, and integration with treatment decisions (De Angelis et al., 2026).
Why PIK3CA Testing Matters Now
Advanced HR+/HER2- breast cancer is commonly treated with endocrine therapy-based strategies, often combined with CDK4/6 inhibition. However, resistance eventually develops in many patients. Alterations in the PI3K/AKT/mTOR pathway are among the mechanisms that can support endocrine resistance, tumor cell survival, and disease progression. Within this pathway, PIK3CA mutations are detected in approximately 35–40% of HR+/HER2- breast cancers, making them one of the most frequent actionable alterations in this disease subtype (De Angelis et al., 2026).
Historically, PIK3CA mutations were viewed partly through the lens of endocrine resistance. With the development of PI3K inhibitors, including alpelisib and inavolisib, their clinical meaning has changed. The consensus emphasizes that PIK3CA mutations now function as predictive biomarkers that can guide targeted treatment selection in patients with advanced HR+/HER2- breast cancer (André et al., 2019; Turner et al., 2024; De Angelis et al., 2026).
A Delphi Consensus Built Around Daily Practice
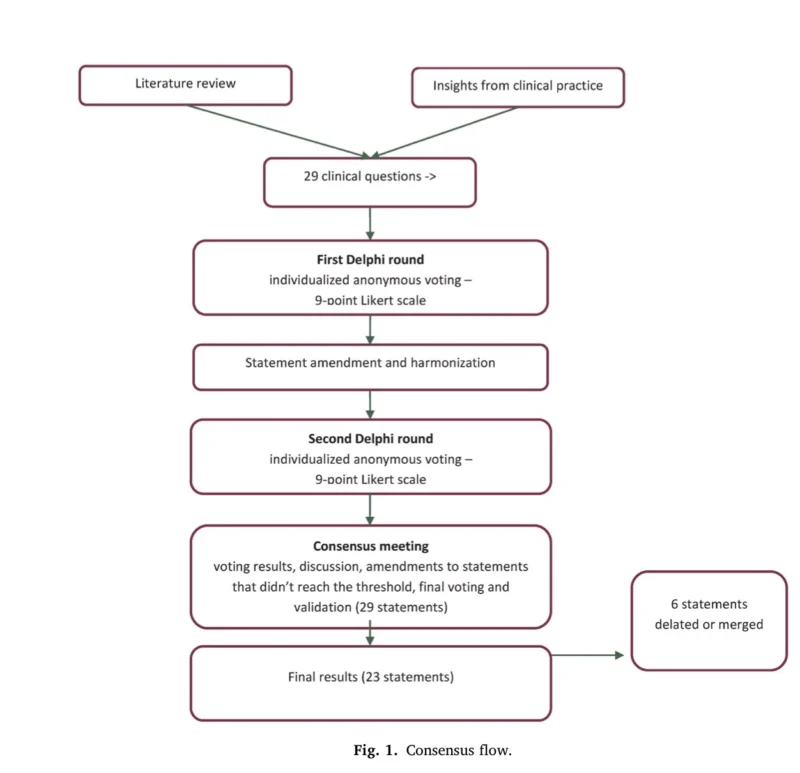
The consensus was developed using a modified Delphi method involving Italian experts in breast oncology, pathology, and molecular biology. The group included two supervisors, a steering committee, and 11 breast cancer experts from tertiary care centers. The process began in March 2025, followed by two Delphi voting rounds between June and September 2025 and a virtual consensus meeting on October 1, 2025 (De Angelis et al., 2026).
Consensus was predefined as at least 80% agreement or strong agreement on a 9-point Likert scale. Of the 29 preliminary statements, 23 reached complete agreement. Some statements were removed because they were redundant or overlapping, but none were excluded because of failure to reach consensus. The final recommendations address three major areas: preanalytical handling, analytical testing, and clinical interpretation.
Tissue Remains Preferred, But Liquid Biopsy Has a Clear Role
One of the most practical recommendations concerns the choice of biological material. The panel states that tumor tissue remains the preferred matrix for PIK3CA testing, mainly because it often provides better DNA quantity and quality. However, liquid biopsy is recognized as a valid alternative, especially when tissue is unavailable, inadequate, or unlikely to reflect current disease biology (De Angelis et al., 2026).
The recommendation is especially important for metastatic disease, where tissue acquisition can be challenging and tumor biology can evolve under treatment pressure. Liquid biopsy, through circulating tumor DNA, offers a minimally invasive way to assess molecular alterations and can be repeated over time. However, the consensus is clear on one critical point: a negative liquid biopsy result does not exclude a PIK3CA mutation. When plasma testing is negative, tissue-based analysis is recommended whenever possible (Pascual et al., 2022; De Angelis et al., 2026).
If an activating PIK3CA mutation is detected in either tissue or plasma, the result is considered clinically valid. In cases of discordance between tissue and liquid biopsy, a positive result from either matrix can guide therapeutic decision-making. This approach aims to avoid excluding patients who may benefit from PI3K pathway inhibition because of tumor heterogeneity or low circulating tumor DNA levels.
NGS Is Preferred Over Narrow Hotspot Testing
The consensus strongly supports next-generation sequencing as the preferred analytical method for PIK3CA testing. Although activating mutations commonly occur in exon 9, such as E542K and E545K, and exon 20, such as H1047R or H1047L, clinically relevant activating variants can also occur outside these canonical regions. For this reason, the panel recommends assays that cover the entire coding sequence of PIK3CA, from exons 1 to 20 (De Angelis et al., 2026).
This has direct clinical relevance. Non-canonical PIK3CA variants such as p.R88Q, p.N345K, and p.C420R may also be functionally activating and can support eligibility for PI3K pathway inhibitors when properly classified. The panel therefore recommends that therapeutic decisions be based on the functional significance of the variant rather than its position in the gene.
For liquid biopsy, analytical sensitivity is a key issue. The consensus recommends an assay limit of detection of ≤0.5% to reliably identify low-frequency variants. Even low variant allele frequency activating mutations are considered clinically relevant, because no validated VAF threshold currently determines eligibility for treatment (De Angelis et al., 2026).
Testing Should Be Timed Around Treatment Decisions
The panel recommends PIK3CA testing in all patients who are candidates for PI3K pathway inhibitors. Testing is particularly important in patients with advanced HR+/HER2- breast cancer who progress during or after endocrine therapy and CDK4/6 inhibitor treatment. The consensus also highlights a specific population informed by the INAVO120 trial: patients who develop advanced disease during or within 12 months after completing adjuvant endocrine therapy should undergo PIK3CA testing (Turner et al., 2024; De Angelis et al., 2026).
For patients with no previously detected pathway alteration, repeat molecular testing at progression may be useful. This reflects the dynamic nature of metastatic breast cancer, where new alterations can emerge under treatment pressure. At the same time, the consensus states that an activating PIK3CA mutation documented at any point in the disease course remains sufficient to consider PI3K pathway inhibitor therapy, since PIK3CA mutations are generally early and stable molecular events.
How Testing Connects To Treatment Selection
The most treatment-specific recommendation concerns patients with activating PIK3CA mutations who experience progression during or within 12 months after adjuvant endocrine therapy. In patients with appropriate clinical characteristics, the consensus identifies inavolisib plus palbociclib and fulvestrant as a first-line treatment option (De Angelis et al., 2026).
This recommendation is supported by the phase III INAVO120 trial, which enrolled patients with PIK3CA-mutated, HR+/HER2- locally advanced or metastatic breast cancer. The combination of inavolisib, palbociclib, and fulvestrant improved progression-free survival compared with placebo plus palbociclib and fulvestrant, with a hazard ratio of 0.42. The regimen also showed an overall survival benefit, with a hazard ratio of 0.67, and improved objective response rate, 62.7% versus 28% (Turner et al., 2024).
The consensus notes that inavolisib received FDA approval in October 2024, followed by approval from China’s National Medical Products Administration in March 2025 and the European Commission in July 2025. These details position PIK3CA testing as a practical requirement for identifying patients who may be eligible for this biomarker-driven approach.
The document also recognizes alpelisib as an established PI3K-targeted option in PIK3CA-mutated HR+/HER2- advanced breast cancer, supported by prior clinical evidence (André et al., 2019; De Angelis et al., 2026).
ESR1 Mutations Do Not Replace PIK3CA Testing
The consensus also addresses a frequent clinical scenario: the coexistence of ESR1 mutations and PI3K pathway alterations. The panel recommends PIK3CA testing even when an ESR1 mutation has already been identified, because the two alterations represent distinct and non-mutually exclusive mechanisms of endocrine resistance (De Angelis et al., 2026).
ESR1 mutations support ligand-independent estrogen receptor activation, while PIK3CA mutations activate downstream survival and proliferation signaling. The consensus notes that ESR1 and PIK3CA co-mutations are detected in approximately 10–15% of HR+/HER2- metastatic breast cancer cases, with potentially higher overlap after multiple lines of endocrine therapy. This reinforces the value of longitudinal molecular profiling rather than single-marker decision-making.
Importantly, the consensus remains cautious about future strategies. It notes that combinations such as next-generation SERDs plus PI3K inhibitors are biologically rational but remain investigational in the absence of clinical data supporting their routine use.
PTEN And AKT1 Expand The Molecular Picture
The panel recommends broader molecular profiling of the PI3K/AKT/mTOR pathway, including PIK3CA, AKT1, and PTEN, especially after progression on aromatase inhibitors and CDK4/6 inhibitors. Multigene NGS panels allow these alterations to be assessed in a single analysis and can provide a more complete view of pathway activation (De Angelis et al., 2026).
However, the consensus makes an important distinction for PTEN. NGS can identify PTEN mutations and copy number variations, but it cannot directly assess loss of PTEN protein expression. For that, immunohistochemistry remains necessary. Similarly, liquid biopsy can detect PTEN genomic alterations through circulating cell-free DNA, but it cannot directly determine protein loss. A comprehensive interpretation therefore requires integration of genomic and tissue-based protein expression data when PTEN status is clinically relevant.
Reporting Standards Are Part Of Precision Care
The consensus emphasizes that molecular reports should be standardized and clinically interpretable. PIK3CA variants should be reported according to HGNC and HGVS nomenclature, with clear documentation of the variant allele frequency, functional effect, and clinical significance using the ESMO Scale for Clinical Actionability of Molecular Targets, or ESCAT (Mateo et al., 2018; De Angelis et al., 2026).
This recommendation is not just technical. Standardized reporting improves communication between molecular laboratories and oncologists, reduces ambiguity, and supports consistent treatment decisions across institutions. The panel also stresses the importance of validated assays, interlaboratory quality control, and strict preanalytical standards, especially for circulating tumor DNA testing.
For liquid biopsy, the preanalytical phase is particularly important. When EDTA tubes are used, plasma separation should occur within 2 hours. Specialized cfDNA preservation tubes can extend this window up to 72 hours. Plasma storage conditions also matter, with short-term storage at −20°C and longer storage at −80°C described in the consensus (De Angelis et al., 2026).
What The Consensus Does Not Answer
This document provides operational guidance, not new prospective trial efficacy or safety data. The safety profile of PI3K pathway inhibitors is not the focus of the consensus, and detailed adverse event outcomes are not reported in the provided article text. The recommendations also reflect a national Italian expert consensus, meaning implementation may vary depending on local access to NGS, liquid biopsy platforms, tissue availability, reimbursement, and regulatory context.
The panel also acknowledges that several areas require continued evidence generation. These include the clinical impact of concurrent ESR1 and PIK3CA mutations, the role of serial testing, how best to integrate PTEN protein loss into treatment selection, and whether future combinations of SERDs and PI3K pathway inhibitors can improve outcomes.
Clinical Meaning For Advanced HR+/HER2- Breast Cancer
The central message of this consensus is that PIK3CA testing is no longer a purely molecular pathology question. It is becoming an operational part of treatment planning in advanced HR+/HER2- breast cancer. Testing can identify patients eligible for PI3K pathway inhibitors, inform sequencing after endocrine therapy resistance, and support more precise interpretation of resistance biology.
For daily practice, the recommendations are clear: use tissue when available, use liquid biopsy when appropriate, confirm negative plasma results with tissue when possible, prefer NGS over narrow testing, report variants in a standardized way, and treat any validated activating PIK3CA mutation as clinically actionable. As PI3K pathway-directed strategies expand, the quality, timing, and interpretation of molecular testing will increasingly influence how clinicians personalize care for patients with advanced HR+/HER2- breast cancer.
Read full article here


