Breast cancer care has changed dramatically over the past few decades. Earlier detection, more refined surgery, improved radiotherapy, endocrine therapy, chemotherapy, anti-HER2 treatment, and immunotherapy have all contributed to better outcomes and lower treatment-related morbidity. Yet even in this modern era, some patients still turn to complementary and alternative medicine, often hoping for a more “natural” path or less toxic approach.
A new cohort study examines what that choice may mean for survival in breast cancer on a national scale (Ayoade et al., 2026). Using data from more than 2.1 million women in the US National Cancer Database, the authors found that the use of complementary and alternative medicine, especially when used instead of standard treatment, was associated with worse survival.
Why This Question Still Matters
Interest in complementary and alternative medicine, often shortened to Complementary and Alternative Medicine, has persisted for years in oncology. Patients may pursue it for symptom relief, immune support, fear of treatment toxicity, distrust of the healthcare system, or the hope of avoiding surgery, radiation, chemotherapy, or endocrine therapy. The challenge is that “CAM” is a broad term, and conversations around it often blur the line between supportive integrative care and the rejection of evidence-based treatment.
That distinction is central to this study. In the National Cancer Database,Complementary and Alternative Medicine was defined as treatment administered by nonmedical personnel. This means the paper is not really evaluating carefully integrated supportive strategies delivered alongside oncology care. It is much more relevant to the question of what happens when patients use alternative therapies instead of, or in a way that displaces, standard breast cancer treatment.
A National-Scale Look at Breast Cancer Treatment Choices
The investigators analyzed female patients diagnosed with breast cancer between 2011 and 2021 in the National Cancer Database. After excluding patients with missing treatment information, the final study population included 2,157,219 women, with a median age of 62 years (Ayoade et al., 2026).
Patients were grouped into four categories: those who received traditional therapy only, those who received Complementary and Alternative Medicine only, those who received both CAM and traditional therapy, and those who received no treatment. Traditional therapy included surgery, chemotherapy, radiation, endocrine therapy, and immunotherapy.
The numbers themselves tell an important story. Nearly all patients, 97.6%, received only traditional therapy. CAM-only use was rare, accounting for fewer than 0.1% of patients. Another fewer than 0.1% received a combination of CAM and traditional therapy. About 2.3% received no treatment at all. So while the use of Complementary and Alternative Medicine in place of conventional treatment was uncommon, it was still measurable at a national level and important enough to study because of its potential consequences.
The Survival Signal Was Hard to Ignore
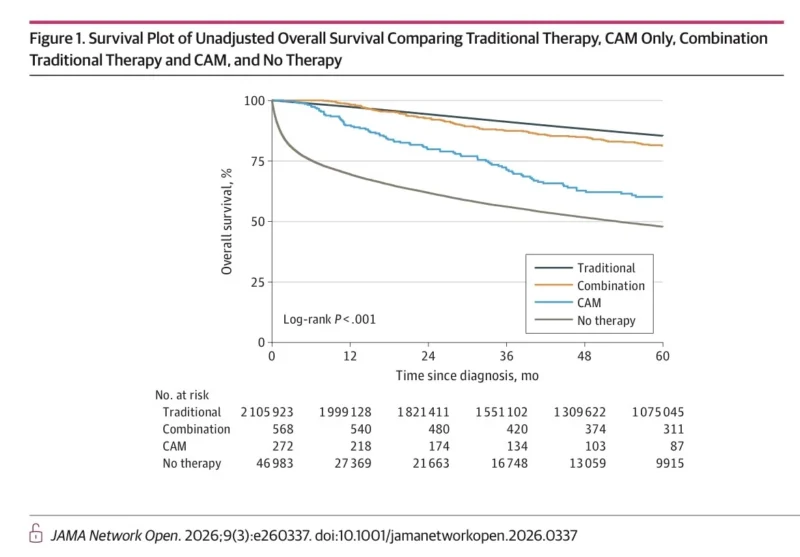
The central finding of the study was straightforward: patients treated with traditional therapy had the best outcomes, while those receiving Complementary and Alternative Medicine alone or no treatment had the worst.
The unadjusted 5-year overall survival rate was 85.4% for patients treated with traditional therapy alone. It was lower, 81.2%, in the group receiving both traditional therapy and CAM. It dropped sharply to 60.1% in the CAM-only group and to 47.8% in the no-treatment group (Ayoade et al., 2026).
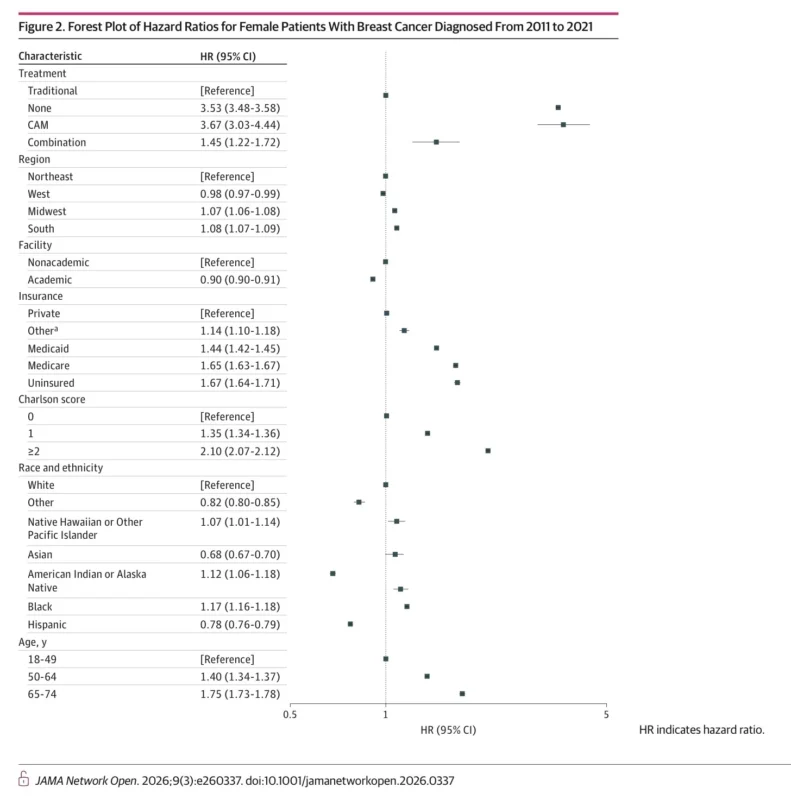
The adjusted analysis, which accounted for age, race and ethnicity, comorbidity burden, insurance, facility type, region, year of diagnosis, cancer stage, and income, reinforced the same message. Compared with patients treated with traditional therapy alone, those receiving CAM alone had the highest mortality risk, with an adjusted hazard ratio of 3.67. Patients who received no treatment had a similarly elevated mortality risk, with an adjusted hazard ratio of 3.53. Even the group receiving both traditional therapy and CAM had worse survival than the traditional-treatment group, with an adjusted hazard ratio of 1.45 (Ayoade et al., 2026).
That is the key clinical message of the paper. In this dataset, CAM was not associated with better outcomes. Used alone, it tracked with markedly worse survival. Used alongside standard care, it was still associated with higher mortality than receiving standard care alone.
What May Be Happening in the “Combination” Group?
One of the most interesting parts of the study is that the worse survival seen in the combined CAM-plus-traditional-treatment group may not mean CAM itself directly caused harm. Instead, it may reflect something else: patients in that group appeared less likely to receive important components of standard breast cancer treatment.
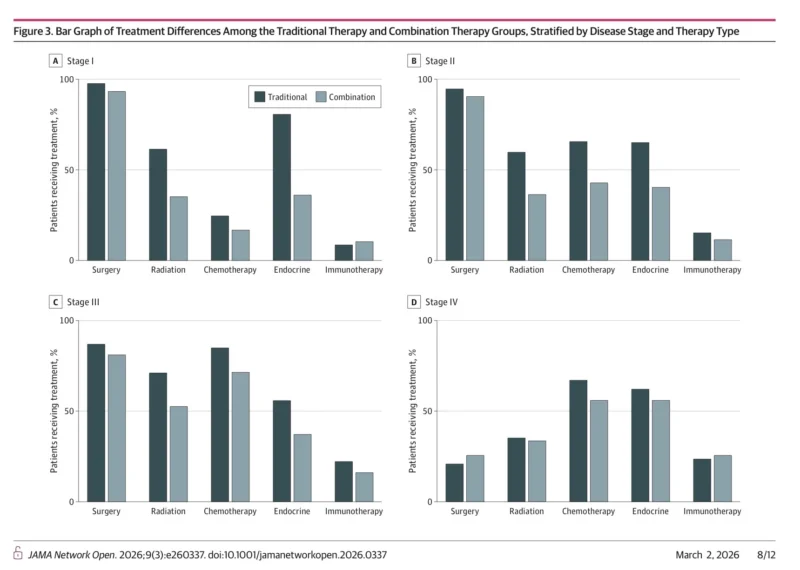
Compared with women treated exclusively with traditional therapy, those in the combination group were less likely to receive radiation and endocrine therapy in stages I through III. In stage II disease, for example, radiation was used in 59.5% of the traditional-therapy group versus 36.6% of the combination group. Endocrine therapy was also notably less common in the combination group in stage II disease, at 40.7% versus 65.2% (Ayoade et al., 2026). Surgery was also modestly less frequent in some earlier-stage settings.
This matters because the omission of endocrine therapy, radiation, or surgery can affect recurrence risk and survival. The study’s sensitivity analysis in stage II disease suggested that patients in the combination group had lower survival when they omitted radiation, endocrine therapy, or surgery. Chemotherapy omission did not show the same statistically significant effect in that particular analysis, but the broader pattern remained clear: Complementary and Alternative Medicine use in this database seemed to coincide with undertreatment.
So the takeaway is not simply that “CAM is dangerous.” It is that patients who turn to alternative therapy may also be more likely to decline or discontinue effective conventional care, and that treatment gap may help explain the worse outcomes.
Who Was More Likely to Choose CAM?
The paper also provides a socioclinical snapshot of the patients involved. Those who received no treatment tended to be older, with a median age of 67 years. The combination group was younger, with a median age of 54 years. Patients receiving CAM only were more likely to have a Charlson Comorbidity Index of 0, suggesting they were often relatively healthy otherwise. Private insurance was more common in the combination cohort than in the traditional-treatment or no-treatment groups (Ayoade et al., 2026).
These findings suggest that alternative treatment choices are not limited to one simple patient profile. They likely reflect a mix of personal beliefs, access issues, treatment fears, and cultural or social influences.
An Important Nuance: This Is Not a Rejection of Supportive Integrative Oncology
One of the most important nuances in the paper is that these findings should not be used to dismiss all integrative approaches in breast cancer care. The authors explicitly note that some therapies commonly grouped under CAM, such as acupuncture, massage, and mindfulness-based approaches, may improve symptoms and quality of life when used as adjuncts to conventional care, not substitutes for it (Ayoade et al., 2026).
That is a critical distinction. Supportive therapies aimed at helping patients tolerate treatment are very different from replacing surgery, radiation, endocrine therapy, or systemic treatment with unproven alternatives. This paper is a warning about the latter.
What Oncologists Should Take From This
This study is a reminder that conversations about alternative medicine need to happen openly and early. Many patients may never tell their oncology team that they are considering nonmedical treatments, especially if they fear judgment or assume clinicians will dismiss their concerns. But silence can be dangerous. If a patient is quietly substituting alternative therapy for evidence-based treatment, the consequences may be profound.
The data from Ayoade et al. suggest that standard breast cancer treatment remains the strongest path to long-term survival. The closer patients stay to that pathway, the better they do. Once effective therapy is omitted or replaced, outcomes worsen quickly.
The Bottom Line
In this large National Cancer Database study, the use of complementary and alternative medicine instead of standard breast cancer treatment was rare but associated with significantly worse survival. Even when CAM was used alongside traditional therapy, outcomes were poorer, likely because patients in that group were less likely to receive key treatment components such as radiation and endocrine therapy (Ayoade et al., 2026).
The message is not that symptom-supportive integrative care has no place in oncology. It does. The message is that breast cancer outcomes suffer when unproven alternative approaches replace evidence-based treatment.
Read full article here


