For young women with early breast cancer and a germline BRCA1 or BRCA2 pathogenic variant, the choice between breast-conserving surgery followed by radiation therapy and mastectomy remains one of the most difficult local-treatment decisions in modern breast oncology. The question is not only oncologic safety, but also timing of genetic testing, future risk-reducing surgery, body image, fertility plans, and long-term survivorship.
A new international cohort study now adds important real-world evidence to that discussion, suggesting that breast-conserving surgery plus radiation therapy was not associated with worse overall survival compared with mastectomy alone, even though second primary breast cancer events were more frequent.
The study analyzed outcomes from the BRCA BCY Collaboration, an international retrospective multicenter cohort of women diagnosed with invasive breast cancer at 40 years or younger and carrying confirmed germline BRCA1/2 variants. According to the authors, this represents the largest international cohort of young BRCA1/2 carriers diagnosed with breast cancer evaluated for this specific loco-regional question.
Why This Question Still Matters
Randomized trials established long ago that, in the general early breast cancer population, breast-conserving therapy can achieve survival outcomes comparable to mastectomy. But BRCA1/2 carriers have always complicated that conversation because they face a substantially higher lifetime risk of both ipsilateral breast events and contralateral breast cancer.
As a result, many patients and clinicians have historically leaned toward mastectomy, and often bilateral mastectomy, even when breast conservation was technically feasible. Current hereditary breast cancer guidelines, however, state that BRCA status alone should not automatically preclude breast-conserving therapy when it is otherwise clinically appropriate. What has been missing is large, contemporary, comparative real-world evidence focused specifically on young carriers.
That is why this analysis is important. It does not argue that every young BRCA carrier should undergo breast conservation. It addresses a narrower and more practical question: if a young BRCA1/2 carrier receives breast-conserving surgery plus radiation, is survival compromised compared with mastectomy-based treatment?
How The Study Was Designed
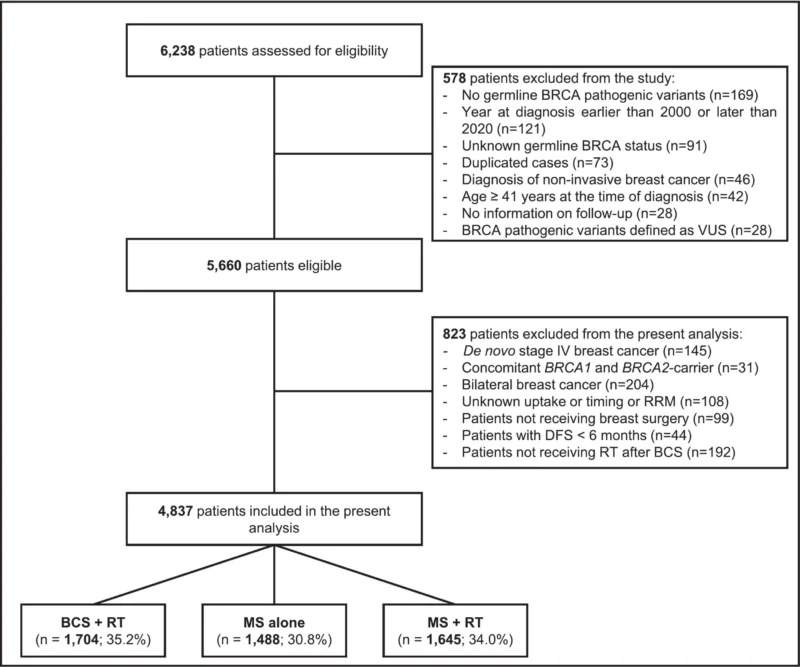
The BRCA BCY Collaboration included women diagnosed between 2000 and 2020 with invasive breast cancer at age 40 years or younger and confirmed germline BRCA1/2 pathogenic variants. For this analysis, the investigators excluded patients with bilateral disease at presentation, de novo stage IV disease, omission of radiation after breast-conserving surgery, unknown timing of key risk-reducing procedures, and very early recurrence events within six months of diagnosis.
Among 4,837 eligible patients, 1,704 received breast-conserving surgery plus radiation therapy, 1,488 underwent mastectomy alone, and 1,645 received mastectomy plus radiation therapy. Median age at diagnosis was 35 years, and most patients were BRCA1 carriers. Importantly, BRCA testing timing differed across groups. In nearly half of the full cohort, genetic testing occurred after diagnosis, and the delay to BRCA testing was longest in the breast-conserving group.
That detail matters, because knowledge of BRCA status at diagnosis can strongly influence surgical choice. To address this, the investigators used left truncation at the time of BRCA testing in their primary statistical models to reduce immortal time bias linked to delayed genetic diagnosis.
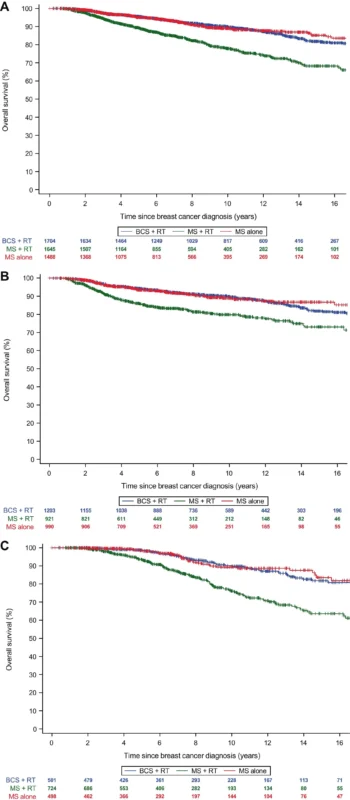
Overall Survival Was Similar After Breast Conservation Plus Radiation and Mastectomy Alone
The main survival message is clear. After a median follow-up of 8.2 years, overall survival did not differ between breast-conserving surgery plus radiation and mastectomy alone. In adjusted analyses, the hazard ratio for overall survival was 1.02 with a 95% confidence interval of 0.78 to 1.34, indicating no meaningful survival disadvantage for breast conservation in this young BRCA1/2 population.
That finding is clinically important because it aligns with current guideline language and offers reassurance in a group where treatment decisions are often heavily influenced by fear of future events. It also means that a young BRCA carrier who strongly prioritizes breast preservation can be counseled that, based on this large real-world dataset, choosing breast-conserving surgery plus radiation did not translate into worse overall survival compared with mastectomy alone.
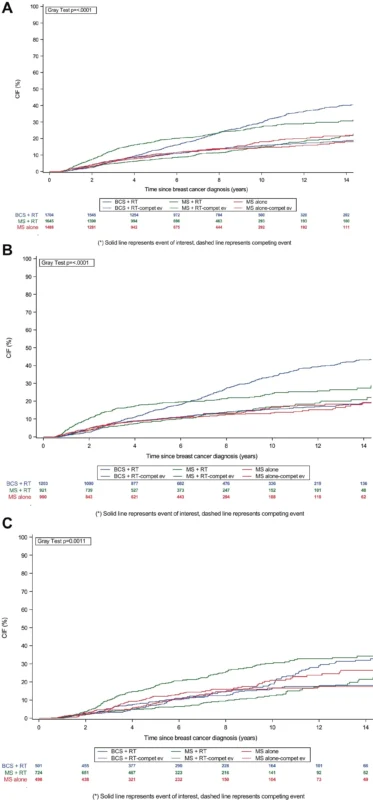
The Trade-Off Was a Higher Risk of Second Primary Breast Events
The survival neutrality does not mean the treatment strategies were interchangeable in every other respect. The study found that breast-conserving surgery plus radiation was associated with a higher risk of second primary breast cancer events, defined as ipsilateral breast recurrence or contralateral breast cancer, compared with mastectomy alone.
The adjusted hazard ratio was 1.33 with a 95% confidence interval of 1.07 to 1.66. Event rates reflected the same pattern: patients treated with breast-conserving therapy had higher rates of loco-regional relapse and second primary breast cancers than those treated with mastectomy alone.
This is the core message of the paper. Breast conservation did not worsen overall survival, but it did carry a higher burden of future breast events. That distinction matters, because the local-treatment discussion in BRCA carriers is not only about mortality. It is also about surveillance intensity, additional procedures, psychological burden, and the possibility of later risk-reducing surgery.
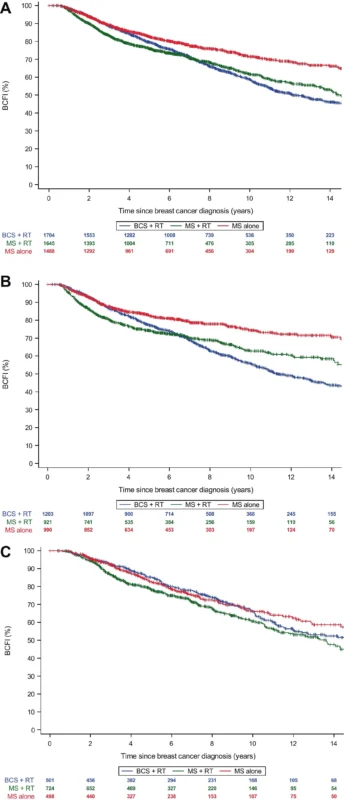
Breast Cancer–Free Interval Was Broadly Comparable Across Groups
Another useful result is that breast cancer–free interval did not differ significantly across loco-regional treatment groups in the overall cohort. In adjusted analyses, breast-conserving surgery plus radiation and mastectomy alone had comparable BCFI outcomes, despite the higher rate of second primary breast events in the breast-conserving group.
That may sound contradictory at first, but it reflects the fact that survival and broader recurrence patterns are shaped by more than ipsilateral or contralateral breast events alone, especially in a population where systemic risk varies substantially by subtype, stage, and BRCA gene.
BRCA1 and BRCA2 Did Not Behave Exactly the Same
One of the more interesting parts of the paper is the subgroup signal. The authors observed heterogeneity by BRCA gene. For second primary breast cancer events, the excess risk associated with breast-conserving surgery plus radiation seemed more pronounced in BRCA1 carriers, whereas BRCA2 carriers showed more favorable or at least numerically less concerning patterns in some subgroup analyses.
The same general divergence appeared in breast cancer–free interval analyses, where the direction of effect seemed less favorable for BRCA1-associated disease and more favorable for BRCA2-associated disease.
These findings should not be overinterpreted as proof that BRCA1 and BRCA2 carriers should automatically be managed differently, but they are biologically plausible. BRCA1-associated cancers are more often triple-negative and high grade, whereas BRCA2-associated tumors are more commonly hormone receptor-positive and may follow a different recurrence trajectory. The study authors themselves caution that residual confounding remains possible, but the gene-specific pattern is difficult to ignore and reinforces the need for more individualized counseling.
Why Timing of Genetic Testing Still Changes Everything
A major practical lesson from the study is not only about surgery or radiation, but about when BRCA testing happens. Patients in the breast-conserving group were more likely to have been diagnosed in earlier years and more likely to have undergone BRCA testing after the initial local-treatment decision. By contrast, mastectomy-based groups included more patients tested before or at diagnosis. This likely influenced treatment selection and helps explain part of the difference in later second primary breast cancer events.
That makes the paper especially relevant in current practice, where access to faster germline testing is improving. The more often BRCA status is known at diagnosis, the better clinicians can frame local treatment around both oncologic safety and future risk-reduction options. This is one of the reasons the authors emphasize that early genetic testing is essential to meaningful shared decision-making.
What This Means for Clinical Practice
The most useful interpretation of this study is not that mastectomy is unnecessary, and not that breast-conserving therapy should be preferred. It is that both are legitimate options in selected young BRCA1/2 carriers, but they come with different trade-offs.
Mastectomy reduces future breast event risk more effectively, especially when bilateral risk-reducing surgery is part of the plan. Breast-conserving surgery plus radiation, however, appears to preserve overall survival, which is a critical reassurance for patients who strongly value organ preservation or who learn their BRCA status only after initial treatment.
This is why the paper’s conclusion is deliberately measured. The authors do not advocate breast conservation universally, nor do they suggest that BRCA status is irrelevant. Instead, they support individualized, multidisciplinary loco-regional decision-making, balancing age, BRCA gene, stage, grade, timing of testing, willingness to undergo later risk-reducing surgery, and the patient’s own priorities regarding body image, future pregnancy, breastfeeding, and surveillance.
The Bottom Line
This study brings needed scale and nuance to a long-debated question. In the largest reported international cohort of BRCA1/2 carriers diagnosed with breast cancer at age 40 or younger, breast-conserving surgery plus radiation therapy was not associated with worse overall survival compared with mastectomy alone. At the same time, it was linked to a higher risk of second primary breast cancer events, particularly in analyses driven by BRCA1-associated disease.
For OncoDaily readers, the message is practical. BRCA status should shape the conversation, but it should not end it. Young BRCA carriers need early testing, careful counseling, and a truly multidisciplinary discussion. For some, mastectomy will remain the preferred choice.
For others, breast conservation plus radiation remains an oncologically defensible option, provided the patient understands the higher likelihood of future breast events and accepts the surveillance and risk-reduction implications that come with it.
Read full article here


