- At the European Lung Cancer Congress 2026, Caichen Li and colleagues presented important prospective data from the LUNG-CARE project, evaluating the clinical impact of one-time low-dose computed tomography (LDCT) screening in a non–risk-based population. While LDCT screening has been well established in high-risk populations, primarily defined by age and smoking history, this study addresses a critical gap by exploring its benefit in a broader, real-world cohort. The findings suggest that restricting screening to traditional risk groups may overlook a substantial number of patients who could benefit from early detection.

Study Design and Population
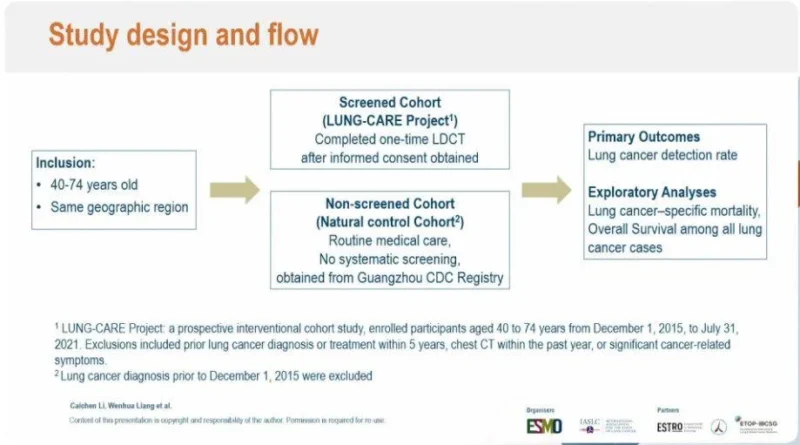
The LUNG-CARE project was designed as a prospective, interventional, non-randomized controlled study, reflecting real-world clinical conditions rather than tightly controlled trial environments. Participants aged 40–74 years from the same geographic region were included, ensuring comparability between groups.
The study consisted of two cohorts. The screened cohort underwent a one-time LDCT scan after informed consent, while the non-screened cohort represented a natural control group derived from a regional registry, receiving routine medical care without systematic screening. This design allowed investigators to assess the real-world effectiveness of LDCT screening while minimizing artificial selection bias.
The primary endpoint was lung cancer detection rate, while key exploratory endpoints included lung cancer–specific mortality and overall survival (OS) among diagnosed cases.
Stage Shift: Earlier Diagnosis as a Key Mechanism
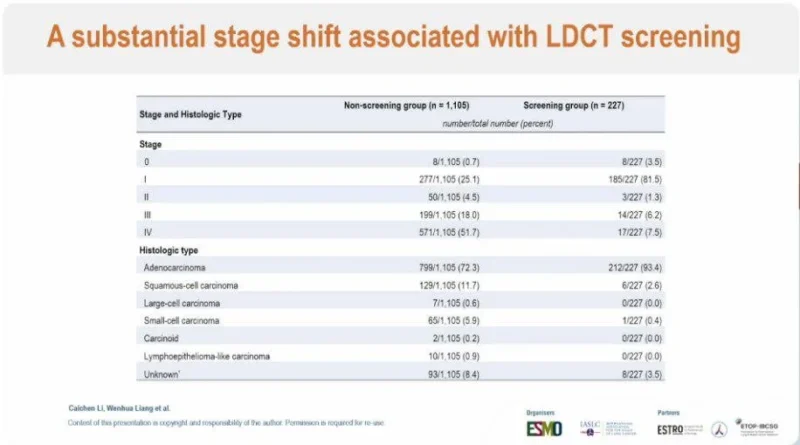
One of the most clinically meaningful observations was the significant stage shift associated with LDCT screening. In the screened population, 81.5% of cases were diagnosed at Stage I, compared with only 25.1% in the non-screened cohort. Conversely, advanced disease was markedly reduced, with Stage IV disease observed in 7.5% of screened patients versus 51.7% in non-screened individuals.
This redistribution toward early-stage disease is central to the survival benefit observed. Early-stage lung cancer is more likely to be treated with curative intent, including surgical resection or stereotactic radiotherapy, whereas advanced disease is typically associated with limited long-term survival. The magnitude of this stage migration highlights LDCT screening as a powerful tool for altering the natural history of lung cancer at a population level.
Mortality Reduction: A Robust and Consistent Signal
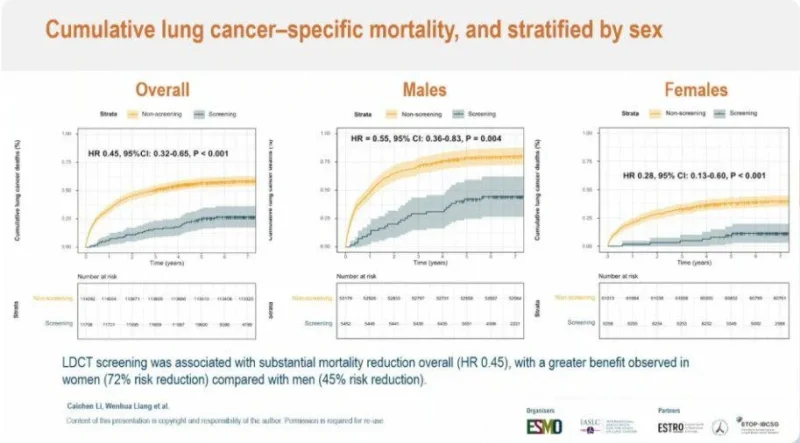
After a median follow-up of 7.0 years, LDCT screening was associated with a significant reduction in lung cancer–specific mortality. The hazard ratio for death was 0.45 (95% CI, 0.32–0.65; P<0.001), corresponding to a 55% relative reduction in mortality.
Importantly, this benefit was consistent across sex-based subgroups. Among men, the hazard ratio was 0.55 (95% CI, 0.36–0.83; P=0.004), while in women, a more pronounced effect was observed with a hazard ratio of 0.28 (95% CI, 0.13–0.60; P<0.001). This suggests that LDCT screening may confer particularly strong benefits in female populations, although the biological and epidemiological reasons for this difference remain to be fully understood.
Overall Survival: Substantial Benefit in Screen-Detected Cases
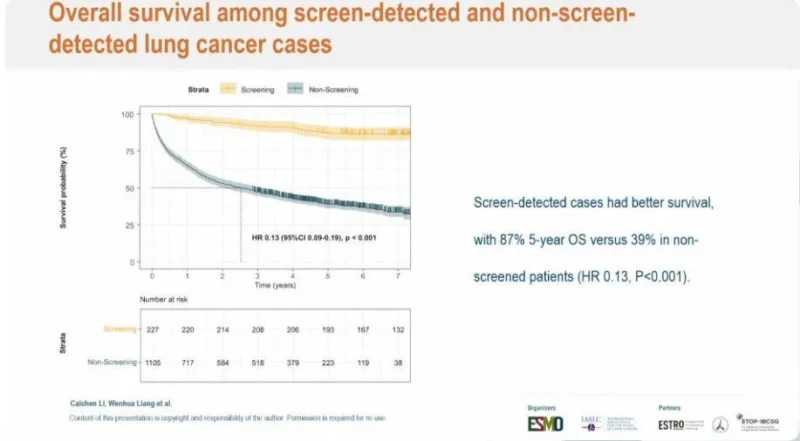
The survival advantage associated with screening extended beyond mortality reduction. Among patients diagnosed with lung cancer, those identified through LDCT screening demonstrated markedly improved outcomes.
The 5-year overall survival rate reached 87% in screened patients, compared with 39% in non-screened individuals. The hazard ratio for death was 0.13 (95% CI, 0.09–0.19; P<0.001), indicating a profound survival benefit associated with early detection.
These findings emphasize that screening not only reduces mortality at a population level but also transforms the prognosis of individual patients by enabling earlier, more effective treatment.
Risk Stratification Within the Screened Cohort
Despite the overall benefits of screening, not all patients experienced the same outcomes. Within the screened population, individuals classified as high risk according to NCCN and Chinese guidelines demonstrated significantly worse survival compared with lower-risk individuals.
Key adverse prognostic factors included heavy smoking history and chronic obstructive pulmonary disease (COPD), both of which were associated with poorer outcomes (P<0.001). Interestingly, other potential risk factors, such as environmental exposures or family history, did not show a statistically significant association with survival in this analysis.
These findings suggest that while screening improves outcomes broadly, underlying patient characteristics continue to influence prognosis and should be considered in post-detection management strategies.
Clinical Implications: Expanding the Scope of Screening
The results of the LUNG-CARE study challenge the current paradigm of strictly risk-based LDCT screening. Existing guidelines, largely developed from Western populations, may not fully capture the complexity of lung cancer epidemiology in other regions, particularly in Asia, where a substantial proportion of patients develop lung cancer without traditional risk factors.
By demonstrating significant mortality reduction and survival improvement in a non–risk-based population, this study supports the potential value of broadening screening eligibility criteria. A more inclusive approach could enable earlier detection across a wider population, ultimately improving outcomes at a population level.
Conclusion
The LUNG-CARE project demonstrates that one-time LDCT screening significantly reduces lung cancer mortality (HR 0.45) and improves overall survival in a non–risk-based population. The observed stage shift toward early disease and the substantial survival advantage in screen-detected cases highlight the transformative potential of screening beyond traditional risk groups.
These findings provide strong evidence to reconsider current screening strategies and support further investigation into more inclusive, population-based approaches to lung cancer detection.


