By Dr. Buga Charles George Kenyi Intern Doctor, Al-Sabbah Children’s Hospital & Juba Teaching Hospital, Juba, South Sudan
Abstract
Pediatric leukemia is among the most treatable malignancies globally, with survival rates exceeding 80% in high-resource settings. However, in South Sudan, outcomes remain poor due to a fundamental lack of chemotherapy and radiotherapy. This case series of three pediatric patients managed at major referral hospitals in Juba illustrates a critical gap: while these malignancies are diagnosable using available hematologic tools, they remain largely untreatable due to a lack of definitive therapy and oncology infrastructure.

The Frontline Reality
In Juba, Al-Sabbah Children’s Hospital and Juba Teaching Hospital serve as the nation’s primary pediatric referral centers, managing an overwhelming volume of approximately 200 daily admissions. Practicing as an intern doctor in these wards exposes the stark realities of a healthcare system where diagnostic capacity exists, but the “cure” remains structurally out of reach.
While both facilities have established bone marrow biopsy capacity to confirm diagnoses, South Sudan currently lacks specialized pediatric oncology units. Critical life-saving treatments—specifically chemotherapy and radiotherapy—are not yet established domestically. This creates a devastating “treatment void” where outcomes are determined by health system limitations rather than disease biology.
Clinical Case Series: The Cost of the Treatment Gap
The following cases illustrate the systemic barriers encountered in pediatric leukemia care within this resource-limited setting:
● Case 1: Acute Myeloid Leukemia (AML):
A 4-year-old presented with unilateral proptosis and was diagnosed with AML via bone marrow biopsy. Despite the confirmed diagnosis, no chemotherapy or radiotherapy was available, and management was restricted to supportive care.
● Case 2: B-cell Acute Lymphoblastic Leukemia (B-ALL):
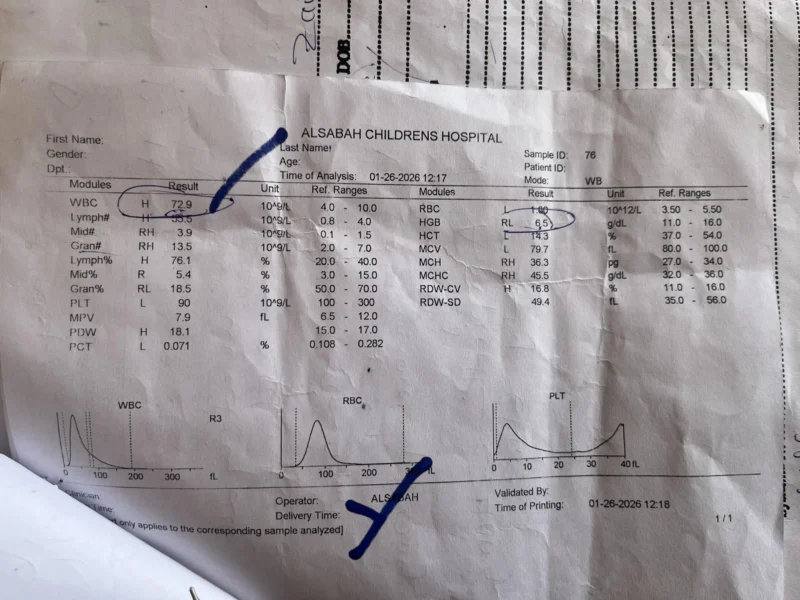
A child was initially treated for malaria for three weeks before a diagnosis of B-ALL with 90% peripheral blasts was confirmed. This case highlights how diagnostic delays, combined with an absolute absence of treatment options, prevent the initiation of life-saving therapy.
● Case 3: T-cell Acute Lymphoblastic Leukemia (T-ALL):
A patient presented with respiratory distress due to a mediastinal mass. While the diagnosis of T-ALL was confirmed, no induction therapy could be initiated due to the complete lack of oncology resources.
The Burden of International Referral
Because specialized cancer care and radiotherapy are not fully established domestically, families are often forced to seek treatment in neighboring Uganda or as far as India. For many, these options are financially and logistically out of reach. Consequently, patients are often managed in general pediatric wards without the benefit of isolation or specialized oncology protocols.
Conclusion: A Call for Urgent Investment
Pediatric leukemia in South Sudan remains a diagnosable but untreatable condition. This series underscores the urgent need for the establishment of domestic oncology services, consistent access to chemotherapy, and strengthened international collaboration. As I prepare to speak at the ESMO Breast Cancer 2026 congress in Berlin, I am committed to highlighting these realities. We must bridge this gap to ensure that a child’s survival is not dictated by their geography, but by the medicine they deserve.
Explore more oncology news and features on OncoDaily


