A new international analysis has taken a practical step toward more individualized treatment decision-making in early triple-negative breast cancer by incorporating stromal tumor-infiltrating lymphocytes into the widely used PREDICT prognostic model. The updated tool, called PREDICT sTILs, was developed using individual patient-level data from 3,698 women with early-stage TNBC and showed strong calibration, discrimination, and improved clinical utility compared with the original PREDICT model.
The core message is clinically important: adding sTILs may help identify low-risk TNBC patients who could safely avoid chemotherapy, while still recognizing those who remain at higher risk and require systemic treatment.
Why This Study Matters
Triple-negative breast cancer has historically been treated aggressively because of its higher recurrence risk and lack of endocrine or HER2-directed treatment options. Chemotherapy remains central to management, but not every patient with early-stage TNBC has the same prognosis. Some patients, especially those with favorable clinical features and immune-rich tumors, may already have excellent outcomes without intensive systemic treatment.
This is where stromal tumor-infiltrating lymphocytes matter. sTILs are assessed on standard hematoxylin and eosin-stained slides, making them inexpensive and widely available. Prior studies have consistently shown that higher sTIL levels are associated with better outcomes in TNBC. However, despite this strong level of evidence, sTILs have not been integrated into widely used clinical decision tools.
The current study addresses this gap by embedding immune biology directly into a validated prognostic framework.
Study Design and Model Development
The analysis included 3,698 patients with early-stage TNBC, drawn from two large pooled cohorts of chemotherapy-treated and untreated patients. The updated model combined the original PREDICT prognostic index with sTILs, modeled as a continuous variable, and evaluated breast cancer-specific survival at both 5 and 10 years.
The model underwent rigorous internal-external validation using a leave-one-region-out approach, ensuring robustness across geographic populations.
The primary endpoint was breast cancer-specific survival, with model performance assessed through calibration and discrimination metrics.
© 2026 Published by Elsevier Ltd on behalf of European Society for Medical Oncology.
Key Findings
One of the most important findings was the strong prognostic impact of sTILs. Each 10% increase in sTILs was associated with a 15% reduction in breast cancer mortality (HR 0.85; 95% CI 0.82–0.88).
The updated PREDICT sTILs model demonstrated:
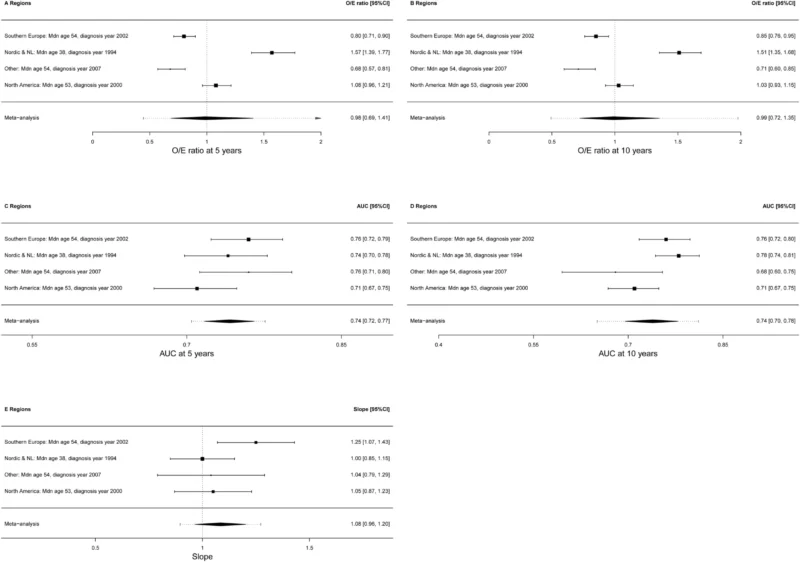
- Strong calibration, with observed-to-expected ratios of 0.98 at 5 years and 0.99 at 10 years
- Consistent discrimination, with AUC values of 0.74 at both 5 and 10 years
- Improved performance compared with the original PREDICT model, which showed lower discriminative ability
These results confirm that integrating immune biomarkers meaningfully improves prognostic accuracy in TNBC.
Clinical Utility: Moving Beyond “Treat All”
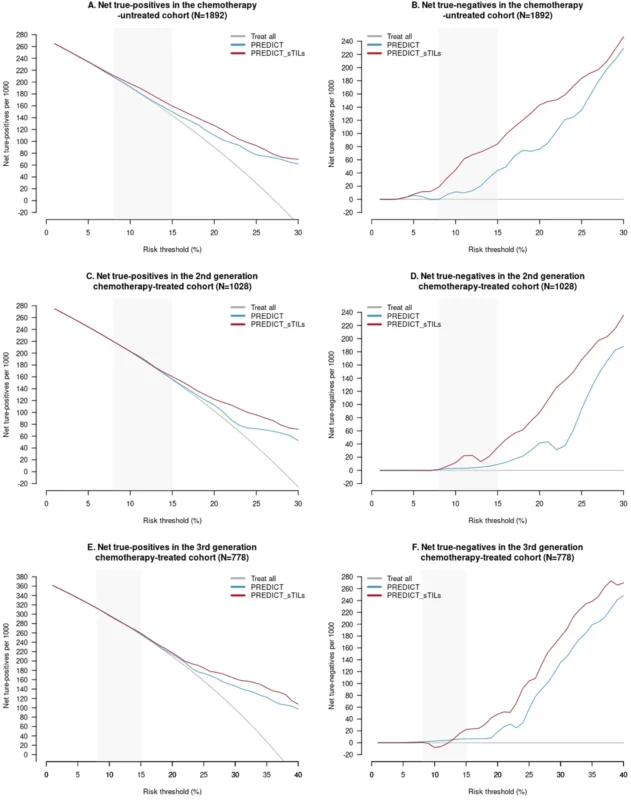
The most practice-relevant finding comes from the decision curve analysis. Compared with the original PREDICT model, PREDICT sTILs provided greater clinical utility across clinically relevant risk thresholds (8–15% 10-year mortality).
Among chemotherapy-naïve patients:
- The model identified 3–10 additional true high-risk patients per 1000, ensuring appropriate treatment escalation
- More importantly, it identified 19–60 additional true low-risk patients per 1000, who could potentially avoid chemotherapy
This is a critical shift. For decades, TNBC has largely been approached with a “chemotherapy-for-all” strategy. These findings suggest that a subset of patients may safely de-escalate treatment based on tumor immune biology.
Interpreting the Results in Modern Practice
The relevance of this work is amplified by the evolving treatment landscape. With the integration of immunotherapy into early TNBC management, particularly in high-risk disease, the need for accurate risk stratification is more important than ever.
PREDICT sTILs does not replace current guidelines but provides a more refined estimate of baseline risk, which can support shared decision-making. For example, in a patient with node-negative disease and high sTILs, the predicted risk of breast cancer mortality may fall below the threshold where chemotherapy provides meaningful benefit.
At the same time, patients with low sTILs and higher clinical risk features remain appropriate candidates for systemic therapy escalation.
© 2026 Published by Elsevier Ltd on behalf of European Society for Medical Oncology.
Strengths and Limitations
This study has several notable strengths. It leverages large, well-characterized cohorts, includes both treated and untreated patients, and uses a robust validation strategy across multiple regions. Importantly, sTILs assessment follows standardized international guidelines, supporting reproducibility in clinical practice.
However, several limitations should be considered. The model does not incorporate modern neoadjuvant immunotherapy regimens, such as those used in KEYNOTE-522. Additionally, cause-of-death attribution relied on surrogate definitions, which may introduce some uncertainty, particularly in older populations. Regional variation in calibration also suggests that local validation may be required before widespread implementation.
What This Means for Clinicians
The integration of sTILs into PREDICT represents more than a technical update. It reflects a broader shift toward immune-informed oncology, where treatment decisions are guided not only by tumor burden and histopathology, but also by the host immune response.
For clinicians, this model offers a practical and accessible way to refine chemotherapy decisions in TNBC, particularly in borderline cases where the benefit of treatment is uncertain.
The Bottom Line
PREDICT sTILs improves prognostic accuracy and clinical decision-making in early-stage TNBC by incorporating a validated immune biomarker.
By identifying more patients who may safely avoid chemotherapy, while preserving the ability to detect high-risk disease, this model moves the field closer to truly personalized care in triple-negative breast cancer.
Read full article here