As populations age and lung cancer screening identifies more small, potentially curable tumors, clinicians are increasingly faced with a difficult question: should adults aged 80 years and older undergo lung cancer surgery when early-stage disease is found? Concerns about frailty, postoperative complications, and long-term recovery often influence treatment decisions, yet prospective evidence in this population has remained limited. A new cohort study now adds important data to this discussion, showing that surgery in octogenarians with early-stage NSCLC can be feasible, with favorable long-term outcomes in carefully selected patients (Gros et al., 2026).
In this prospective analysis from the Initiative for Early Lung Cancer Research on Treatment, investigators compared octogenarians with younger patients who underwent resection for stage IA non-small cell lung cancer. The study found that older adults had somewhat higher postoperative complication rates, particularly cardiovascular, urologic, and neurologic events, but hospital stay, readmission patterns, long-term quality of life, and survival were broadly similar between groups. These findings suggest that chronological age alone should not automatically exclude older adults from surgical evaluation (Gros et al., 2026).
Read About Non-Small Cell Lung Cancer on OncoDaily
Why This Study Matters
The number of adults aged 80 years and older diagnosed with small, early-stage lung cancers is rising. This reflects both longer life expectancy and broader use of imaging and lung cancer screening. Yet this same group is often underrepresented in clinical trials and sometimes excluded from screening pathways because of assumptions about surgical risk and postoperative recovery. As a result, evidence guiding treatment decisions has been incomplete.
This makes the current report especially relevant. According to the authors, prospective data directly comparing younger patients and octogenarians with stage IA non-small cell lung cancer have been scarce, especially for patient-reported quality of life after surgery. The present study addresses this gap and provides one of the clearest prospective looks at surgery in octogenarians with early-stage NSCLC in a modern clinical setting (Gros et al., 2026).
Study Design And Patient Population
The investigators analyzed patients from the Mount Sinai Health System who were prospectively enrolled in the IELCART cohort and underwent surgery between 2016 and December 2024 for first primary stage IA non-small cell lung cancer measuring 30 mm or less on preoperative CT. The study included 884 patients in total, of whom 114, or 12.9%, were octogenarians. The remaining 770 patients were younger than 80 years (Gros et al., 2026).
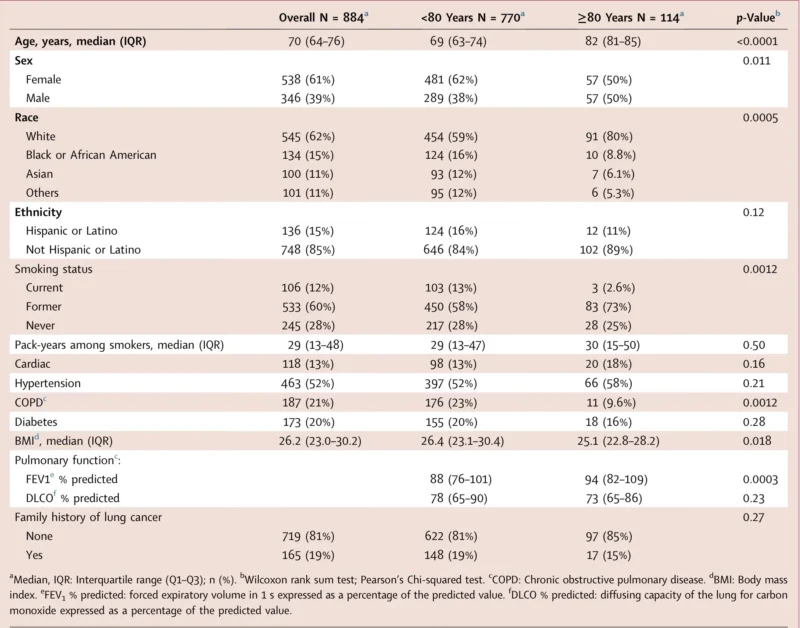
Median age was 82 years in the octogenarian group and 69 years in the younger group. Among octogenarians, the sex distribution was evenly split, with 50% women and 50% men. In contrast, women represented 62% of the younger cohort. Race also differed between age groups. Octogenarians were more frequently White, accounting for 80% of older patients compared with 59% of younger patients. Black or African American patients accounted for 8.8% of octogenarians and 16% of younger patients, while Asian patients accounted for 6.1% and 12%, respectively (Gros et al., 2026).
Smoking history also varied. Only 2.6% of octogenarians were current smokers compared with 13% of younger patients. Former smokers made up 73% of the older group and 58% of the younger group, while never-smokers represented 25% and 28%, respectively. Median pack-years among smokers were similar, at 30 in octogenarians and 29 in younger patients (Gros et al., 2026).
The Lancet Regional Health – Americas, 2026; 56
Baseline Health Status And Pulmonary Function
One of the more interesting observations was that the older surgical group did not appear substantially more burdened by self-reported comorbidity. Hypertension was present in 58% of octogenarians and 52% of younger patients, while diabetes was reported in 16% and 20%, respectively. Chronic obstructive pulmonary disease was actually less frequent in octogenarians, seen in 9.6% compared with 23% of younger patients. Median body mass index was slightly lower in the older group, at 25.1 versus 26.4 (Gros et al., 2026).
Pulmonary function also showed some differences. Forced expiratory volume in one second percent predicted was higher in octogenarians, at 94% versus 88% in younger patients, while diffusing capacity of the lung for carbon monoxide percent predicted was similar, at 73% versus 78%. These findings likely reflect selection of fitter older adults for surgery, an important point when interpreting the outcomes of surgery in octogenarians with early-stage NSCLC (Gros et al., 2026).
Tumor Features And Surgical Approach
Tumor presentation was largely similar across groups. Nodule consistency, location, and preoperative nodule diameter did not differ significantly. However, resected tumors were slightly larger in octogenarians, with a median size of 18 mm compared with 16 mm in younger patients.
Histology differed significantly. Adenocarcinoma accounted for 88% of tumors in octogenarians versus 75% in younger patients, while squamous cell carcinoma represented 8.8% and 10%, respectively. Angiolymphatic invasion was more frequent in octogenarians, occurring in 40% versus 29% of younger patients. Yet vascular invasion, margin status, margin-to-tumor ratio, pathological stage distribution, and number of lymph nodes resected were similar across age groups.
The most notable treatment difference was surgical extent. Octogenarians underwent fewer lobectomies and more sublobar resections. Lobectomy was performed in 21% of octogenarians compared with 35.3% of younger patients. Wedge resection was performed in 71% of octogenarians and 56% of younger patients, while segmentectomy occurred in 7.9% and 6.5%, respectively. Overall, sublobar resection was more common in the older cohort, reflecting a more conservative surgical approach in surgery in octogenarians with early-stage NSCLC.
Postoperative Outcomes And Complications
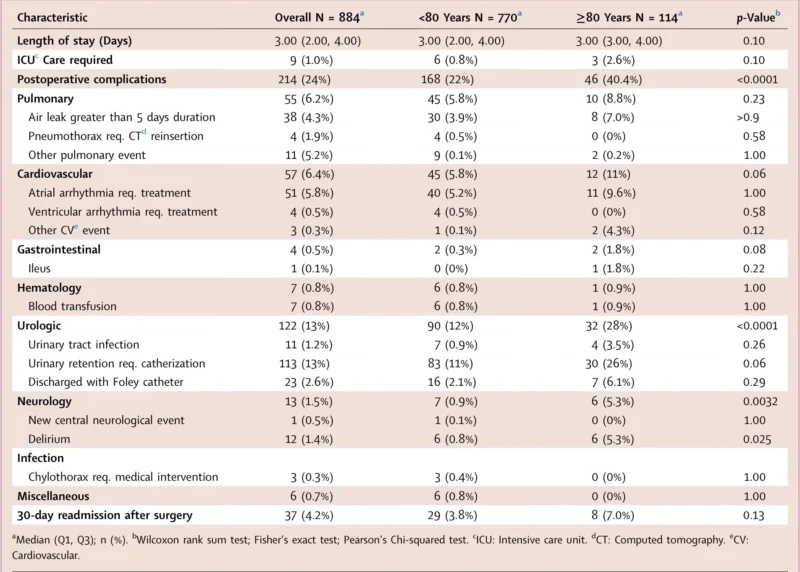
A key question in this study was whether older adults experience markedly worse postoperative recovery. The answer was mixed. Median hospital stay was 3 days in both groups, with no significant difference. Intensive care unit admission was slightly more frequent in octogenarians, at 2.6% versus 0.8%, but this difference was not statistically significant. Thirty-day readmission occurred in 7.0% of octogenarians and 3.8% of younger patients, again without a statistically significant difference (Gros et al., 2026).
Complications, however, were clearly more common in the older group. Overall postoperative complications occurred in 40.4% of octogenarians compared with 22% of younger patients. Urologic complications were especially increased, occurring in 28% of octogenarians and 12% of younger patients. Neurologic complications were also more frequent, at 5.3% versus 0.9%, while cardiovascular complications occurred in 11% of octogenarians and 5.8% of younger patients. Pulmonary complications occurred in 8.8% of octogenarians and 5.8% of younger patients, though this difference was not significant (Gros et al., 2026).
Delirium was more common in older adults, occurring in 5.3% versus 0.8%. Urinary retention requiring catheterization occurred in 26% of octogenarians and 11% of younger patients. Despite this higher complication burden, perioperative mortality remained low. No deaths occurred within 30 days of surgery, and within 90 days there were 3 deaths total, including 1 among octogenarians and 2 among younger patients.
The Lancet Regional Health – Americas, 2026; 56
These findings suggest that surgery in octogenarians with early-stage NSCLC does carry more postoperative morbidity, but not necessarily more prolonged hospitalization or clearly worse short-term recovery when patients are carefully selected.
Quality Of Life After Surgery
The quality-of-life analysis is one of the most valuable parts of the study. Among 884 patients, quality-of-life data were available for 835, representing 94.5% of the cohort. Completion rates were high and did not differ significantly between age groups at any time point.
Quality of life was assessed using the SF-12 physical component summary and mental component summary. At baseline, physical scores were similar: 46.29 in octogenarians and 45.86 in younger patients. At 2 months after surgery, both groups declined, to 43.76 and 41.96, respectively. By 12 months, both groups had recovered, reaching 47.29 in octogenarians and 47.87 in younger patients.
Mental health scores followed a similar pattern of overall stability. Baseline mental component scores were 50.75 in octogenarians and 50.09 in younger patients. At 2 months, scores were 49.56 and 50.76, respectively. By 12 months, mental scores improved to 51.34 in octogenarians and 52.20 in younger patients.
Importantly, none of the pairwise differences between age groups were statistically significant, and all absolute differences were less than 2 points, below the 3-point threshold generally considered clinically meaningful. In practical terms, this means surgery in octogenarians with early-stage NSCLC did not result in worse long-term physical or mental quality of life compared with younger adults in this cohort.
Long-Term Survival Outcomes
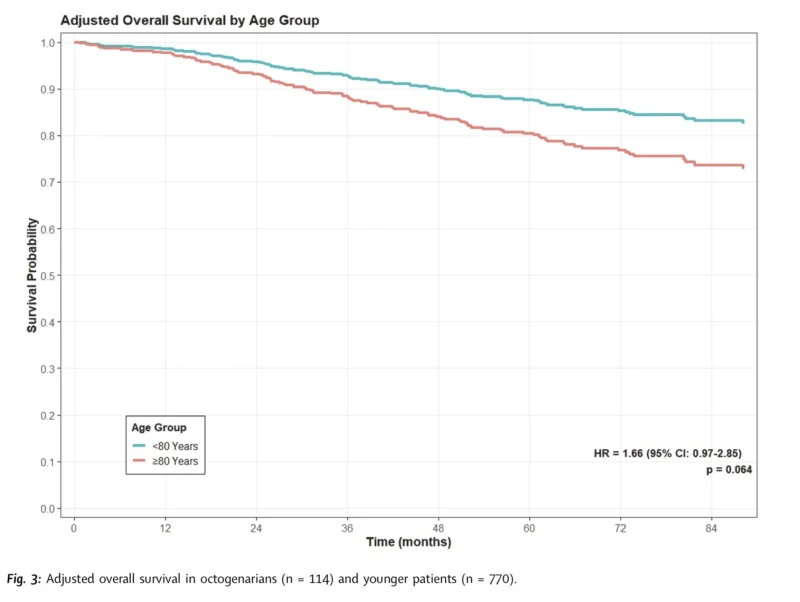
The survival data were also reassuring. Median follow-up was 4.28 years. During this time, 103 patients died, including 37 from lung cancer. The 5-year overall survival rate was 84.2% in octogenarians and 87.3% in younger patients. Although numerically lower in the older group, this difference was not statistically significant. Five-year lung cancer-specific survival was nearly identical, at 94.4% in octogenarians and 94.5% in younger patients.
Adjusted analysis supported these findings. For overall mortality, the adjusted hazard ratio for octogenarians versus younger patients was 1.66, with a 95% confidence interval of 0.97 to 2.85, which did not reach statistical significance. For lung cancer-specific mortality, the subdistribution hazard ratio was 1.16 with a 95% confidence interval of 0.43 to 3.12, again not significant.
These results suggest that in a selected surgical population, surgery in octogenarians with early-stage NSCLC can produce long-term cancer outcomes comparable to those seen in younger adults.
What These Findings Mean For Clinical Practice
The message from this study is not that every octogenarian with early-stage lung cancer should automatically undergo resection. Rather, it shows that age alone should not be used as a reason to deny surgical evaluation. In this prospective cohort, older adults were more likely to receive limited resections and had more postoperative complications, but they still achieved similar hospital stays, similar quality-of-life recovery, and similar 5-year lung cancer-specific survival.
This is highly relevant in modern thoracic oncology. As more older adults are diagnosed through imaging and screening, multidisciplinary teams will need better frameworks for deciding who can benefit from surgery. This study supports individualized assessment based on functional status, pulmonary reserve, comorbidities, tumor features, and patient preferences, rather than relying on chronological age alone.
The Lancet Regional Health – Americas, 2026; 56
The Bottom Line
This prospective cohort study provides strong support for surgery in octogenarians with early-stage NSCLC when patients are carefully selected. Among 114 octogenarians and 770 younger patients with stage IA disease, older adults experienced more postoperative complications, especially urologic, neurologic, and cardiovascular events, but they had similar hospital stays, similar recovery in physical and mental quality of life, and nearly identical 5-year lung cancer-specific survival at 94.4% versus 94.5% (Gros et al., 2026).
For clinicians, these findings challenge the assumption that surgery is inherently too risky in patients aged 80 years and older. For patients and families, they offer an important message: with careful evaluation and appropriate perioperative care, curative-intent surgery can remain a realistic and effective option even in later life.
Read full article on Lancet