Retroperitoneal sarcomas are rare malignancies arising in a complex anatomical space that makes complete surgical management particularly challenging. Among these tumors, liposarcoma represents the most common histologic subtype, and well-differentiated liposarcoma (WDLPS) accounts for a large proportion of primary retroperitoneal cases.
Primary retroperitoneal WDLPS (pRP-WDLPS) exhibits a distinctive clinical course characterized by frequent local recurrence and an extremely low risk of distant metastasis. As a result, long-term outcomes depend predominantly on achieving durable local disease control rather than preventing systemic spread.
Radiotherapy For Soft Tissue Sarcomas: Types, Success Rate, Side Effects And More

Surgical resection with curative intent remains the cornerstone of treatment. However, even after macroscopically complete resections, local relapse rates remain high, often necessitating repeated operations associated with significant morbidity. The potential role of radiotherapy as an adjunct to surgery has therefore been extensively investigated.
While postoperative radiotherapy is limited by toxicity to surrounding organs, preoperative (neoadjuvant) radiotherapy offers theoretical advantages. Nevertheless, evidence regarding its efficacy in retroperitoneal sarcomas has been inconsistent, particularly following the phase III STRASS trial, which showed no overall benefit across heterogeneous histologies but suggested a possible advantage in liposarcoma subgroups.
To address this uncertainty with histology-specific data, the Transatlantic Australasian Retroperitoneal Sarcoma Working Group (TARPSWG) conducted the largest study to date evaluating the impact of neoadjuvant radiotherapy in patients undergoing surgery for pRP-WDLPS.
Study Design and Methods
This multicenter retrospective analysis included patients treated between January 2002 and December 2017 at 24 high-volume sarcoma centers participating in TARPSWG. Only patients with pathologically confirmed primary retroperitoneal WDLPS who underwent curative-intent resection were included, while cases with any dedifferentiated component were excluded to maintain a biologically uniform cohort.
Because treatment assignment was not randomized, the investigators employed propensity score matching to reduce selection bias and create comparable treatment groups. Patients receiving neoadjuvant radiotherapy followed by surgery were matched in a 1:2 ratio with patients undergoing surgery alone based on age, sex, tumor size, multifocality, and completeness of resection.
The primary endpoint of the study was the cumulative incidence of local recurrence, reflecting the dominant failure pattern of this disease. Overall survival served as a secondary endpoint. Competing-risk analysis was used to account for events such as distant recurrence or death without recurrence, ensuring a more accurate assessment of local failure risk.
Patient Population and Treatment Characteristics
A total of 582 patients met inclusion criteria. Most patients underwent surgery alone, while a smaller proportion received neoadjuvant radiotherapy prior to resection. After propensity matching, 208 patients formed the analytic cohort, including 70 patients treated with neoadjuvant radiotherapy followed by surgery and 138 treated with surgery alone.
Patients in the matched cohort had a median age of approximately 60 years, and tumors were typically very large, with a median size of about 25 centimeters. The majority of tumors were unifocal, and all patients underwent macroscopically complete resection. The median radiation dose delivered preoperatively was approximately 50 Gy, consistent with contemporary practice.
Effect on Local Recurrence
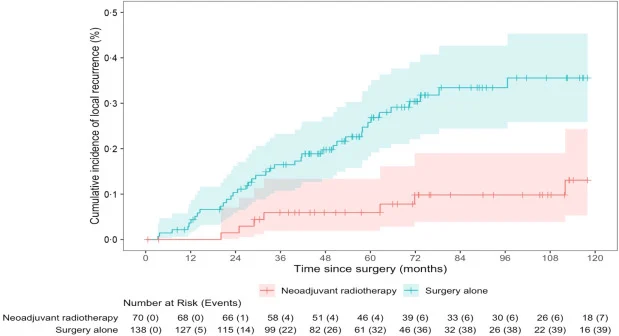
The most striking finding of the study was the substantial reduction in local recurrence associated with neoadjuvant radiotherapy. With a median follow-up of more than six years, patients who received preoperative radiotherapy experienced markedly lower rates of local failure compared with those treated with surgery alone.
At five years, the cumulative incidence of local recurrence was only 6 percent in the neoadjuvant radiotherapy group, compared with 26 percent in the surgery-alone group. At eight years, recurrence rates remained significantly lower in the radiotherapy group, at 10 percent versus 33 percent. Statistical analysis confirmed that neoadjuvant radiotherapy was associated with a significantly reduced risk of local recurrence.
These findings underscore the biological reality that pRP-WDLPS behaves predominantly as a locally aggressive disease. Improved local control has important clinical implications, as repeated recurrences often lead to complex reoperations, progressive organ involvement, and cumulative morbidity.
Overall Survival Outcomes
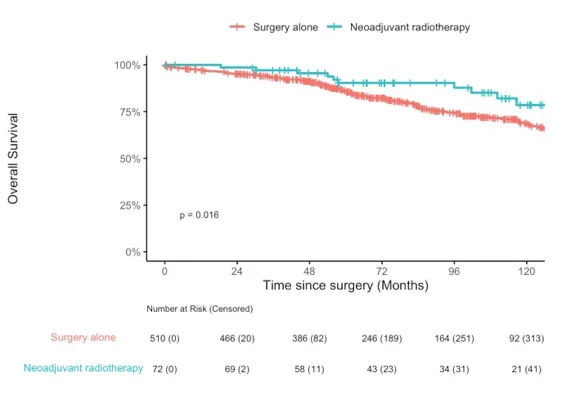
Despite the clear benefit in local control, the study did not demonstrate a statistically significant improvement in overall survival associated with neoadjuvant radiotherapy. Survival rates were numerically higher in the radiotherapy group, but the difference did not reach statistical significance. Median overall survival was not reached in either group, reflecting the relatively indolent natural history of WDLPS even when recurrence occurs.
The absence of a survival benefit should be interpreted cautiously. Because deaths in this disease often occur many years after diagnosis, follow-up exceeding a decade may be required to detect meaningful differences. Furthermore, improved local control may translate into better quality of life and reduced need for repeated surgery, outcomes not fully captured by overall survival alone.
Relationship to Prior Evidence
The TARPSWG analysis provides important context for interpreting earlier studies. The STRASS randomized trial, which included multiple histologic subtypes of retroperitoneal sarcoma, did not show a benefit of neoadjuvant radiotherapy in the overall population. However, exploratory subgroup analyses suggested improved outcomes in liposarcoma, particularly well-differentiated tumors. The subsequent STREXIT study, combining randomized and observational data, also indicated improved local control in WDLPS with preoperative radiotherapy.
By focusing exclusively on pRP-WDLPS and including a large international cohort, the TARPSWG study offers robust evidence supporting a histology-specific approach to treatment. It represents one of the clearest demonstrations that therapeutic strategies in sarcoma must be tailored to tumor biology rather than applied uniformly across heterogeneous subtypes.
Rationale for Preoperative Radiotherapy
Delivering radiotherapy before surgery offers several technical and biological advantages in retroperitoneal tumors. The intact tumor mass displaces surrounding organs, allowing radiation to be delivered more precisely while sparing sensitive structures such as the small intestine.
Preoperative treatment also requires lower radiation doses than postoperative therapy and may sterilize microscopic disease at the tumor margins, which are often difficult to define surgically in the retroperitoneum. Importantly, the goal of neoadjuvant radiotherapy in WDLPS is not tumor shrinkage but prevention of local regrowth from residual microscopic disease.
Clinical Implications
The results of this large international study support the integration of neoadjuvant radiotherapy into the multidisciplinary management of selected patients with pRP-WDLPS. While surgery remains the primary curative modality, preoperative radiotherapy appears to substantially improve local disease control. Given the complexity of treatment and the need to balance benefits against potential toxicity, decisions should be individualized and made within specialized sarcoma centers.
As a retrospective study, the analysis is subject to inherent limitations, including potential residual confounding despite propensity matching. Variability in surgical techniques, surveillance practices, and institutional protocols may also influence outcomes. Additionally, detailed information on perioperative morbidity and extent of organ resection was not available. Nonetheless, the large sample size and rigorous methodology provide compelling evidence in a disease where randomized trials are difficult to conduct.
Neoadjuvant Radiotherapy in Soft Tissue Sarcomas
Find more exclusive Radiation Oncology content on OncoDaily.
Written by Nare Hovhannisyan, MD



