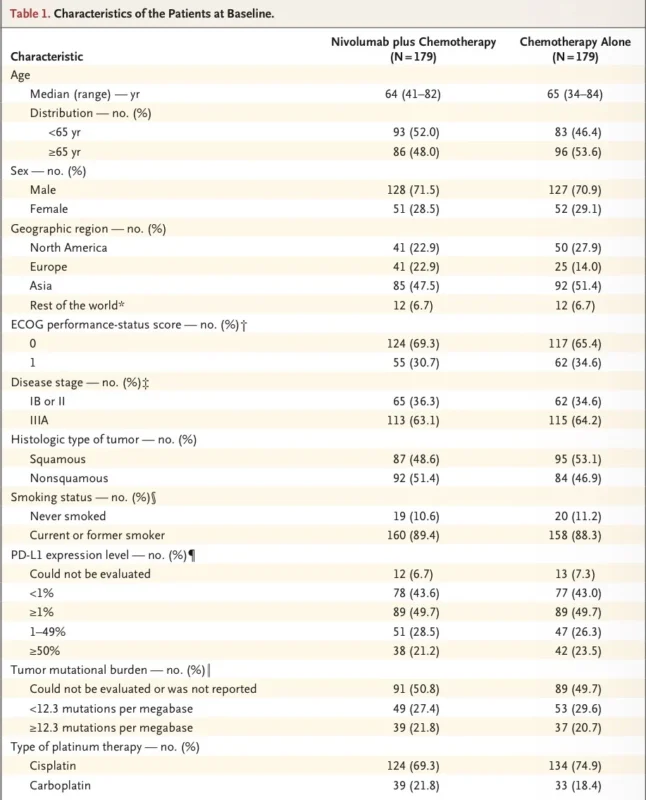
Neoadjuvant immunotherapy has changed the treatment landscape for resectable non small cell lung cancer. The strongest example remains CheckMate 816, where nivolumab plus chemotherapy improved long term outcomes over chemotherapy alone. In the final overall survival analysis, the 5 year overall survival rate was 65.4% with nivolumab plus chemotherapy versus 55.0% with chemotherapy alone, reinforcing the clinical relevance of early pathological response in this setting (Forde et al., 2025).
Against that background, the next question becomes more important, not less. If pathologic complete response, or pCR, is associated with better outcomes, can it truly stand in for survival in trials of resectable NSCLC, or is it better understood as a favorable prognostic marker rather than a validated surrogate endpoint? That is the central issue addressed by Bardoni and colleagues in their systematic review, titled Is Pathologic Complete Response a Reliable Surrogate Endpoint for Survival After Neoadjuvant Immunotherapy in Resectable NSCLC? A Systematic Review.
Read About Non-Small Cell Lung Cancer on OncoDaily
Why This Question Matters
In early lung cancer, overall survival remains the most meaningful endpoint. The problem is that it takes years to mature. That delay slows trial interpretation and complicates drug development in a setting where perioperative strategies are evolving quickly. For that reason, surrogate endpoints such as pCR and major pathologic response, or MPR, have taken on increasing importance in neoadjuvant studies. At the same time, the field has remained cautious, because a marker can correlate with survival at the patient level without functioning as a true surrogate at the trial level (Bertolaccini et al., 2024).
This distinction has become even more relevant in the immunotherapy era. A Nature Medicine analysis of CheckMate 816 showed that the depth of pathologic response, measured by residual viable tumor, correlated with event free survival after neoadjuvant nivolumab plus chemotherapy. The same analysis suggested that pathological response may function as an important biomarker of benefit, but it also emphasized that the most clinically meaningful response thresholds beyond classic pCR and MPR are still being defined (Deutsch et al., 2024).
What The Review Examined
The systematic review by Bardoni et al. 2026 focused on the prognostic value of pCR after neoadjuvant immunotherapy in resectable NSCLC and explored whether pCR could reliably predict survival endpoints such as disease free survival, event free survival, and overall survival. The review also examined recurrence after pCR and compared the predictive value of pCR with MPR.
According to the review, the analysis included 23 studies involving 3,487 patients with resectable NSCLC treated with neoadjuvant immunotherapy with or without chemotherapy before surgery. The clinical question was straightforward, but highly relevant: does achieving pCR actually capture long term benefit well enough to serve as a standalone endpoint?
What The Authors Found
The results were clinically important. Reported pCR rates ranged from 6% to 38%, with higher rates generally seen in chemoimmunotherapy regimens. Patients who achieved pCR had better outcomes, with 2 year disease free survival rates of 85% to 92%, compared with 55% to 70% in patients without pCR.
That would normally support a very strong argument for pCR. But the review did not stop there. The authors also found that recurrence still occurred in 8% to 15% of cases despite pCR, most often as distant relapse. That single observation is enough to shift the discussion. It means that even when no viable tumor is identified pathologically, pCR does not fully eliminate the risk of later clinical failure.
Another important finding was that MPR showed a similar or in some studies stronger association with survival than pCR. This adds nuance to a conversation that often becomes too binary. In practice, pCR is the most dramatic response category, but it may not always be the most informative one.
Why pCR Is Not the Whole Story
The main conclusion of the review is both balanced and useful: pCR is prognostic, but not sufficient as a standalone surrogate endpoint. That is very much in line with the broader literature.
A 2024 systematic literature review and meta analysis found a strong and consistent association between pathological response and survival in resectable NSCLC. Patients with pCR had better overall survival than those without pCR, and patients with MPR also had clearly better outcomes. However, the same study found something just as important: while event free survival showed a moderate to strong correlation with overall survival at the trial level, treatment effects on pCR did not show a meaningful correlation with treatment effects on overall survival or event free survival (Waser et al., 2024).
That is exactly why this topic remains unsettled. At the patient level, pCR is clearly good news. At the trial level, it may still be too incomplete to serve as a definitive substitute for survival. Those are not contradictory statements. They simply describe two different levels of evidence.
The review by Bardoni et al. also highlights another important issue: heterogeneity. The authors observed substantial variation across included studies in design, treatment regimens, pathologic assessment, and even the definitions used for pCR and MPR. That heterogeneity makes it harder to compare results across studies and weakens confidence in any universal claim that pCR alone should be treated as a robust surrogate endpoint.
Where MPR Fits Into the Discussion
One of the most interesting aspects of this review is the emphasis on MPR. In lung cancer, MPR has long been considered a practical and biologically meaningful endpoint because it captures a broader population of responders than pCR. Bardoni et al. note that several studies reported a similar or stronger association between MPR and survival compared with pCR.
That observation is supported by larger meta analytic data. In the 2024 systematic review, the association between MPR and overall survival was numerically stronger than the association between pCR and overall survival, although the authors appropriately noted that the MPR analysis included fewer studies and should be interpreted carefully (Waser et al., 2024).
This does not mean MPR should replace pCR. It means the field may need a more integrated framework. Pathologic response after neoadjuvant immunotherapy is probably better interpreted on a spectrum rather than as a single all or nothing event.

What This Means for Clinical Practice
For clinicians, the practical interpretation is straightforward. Achieving pCR after neoadjuvant immunotherapy in resectable NSCLC remains an excellent sign and should be viewed as a strong indicator of benefit. But it should not be treated as the entire story. Some patients still recur. Not all studies define pathological endpoints in the same way. And the formal requirements for surrogate endpoint validation are higher than simple prognostic association.
That is why the conclusion of this review feels clinically mature rather than cautious. The authors do not dismiss pCR. They place it where it belongs. It is a meaningful marker of response and a strong prognostic signal, but not yet a sufficient standalone substitute for survival.
What Comes Next
The most forward looking part of the review is its final implication. The authors suggest that integrating pCR with MPR and additional clinical or molecular biomarkers may provide a stronger framework for outcome prediction. That direction is consistent with the broader movement in thoracic oncology, where ctDNA, nodal clearance, radiographic response, and residual viable tumor burden are increasingly being studied together rather than in isolation (Deutsch et al., 2024).
In that sense, this review captures where the field stands today. Pathologic complete response matters. It is associated with improved survival outcomes after neoadjuvant immunotherapy in resectable NSCLC. But recurrence despite pCR, along with persistent variability in pathological assessment, limits its value as a standalone surrogate endpoint. For now, the more reliable path is not to abandon pCR, but to interpret it within a broader and more biologically informed framework.
You can read about CheckMate 816 Trial here


