The lung oncology field continues to move forward through more than trial results alone. It is also shaped by the physicians, scientists, and advocates who draw attention to the questions that still need answers, from screening gaps and biomarker testing to young-onset disease, never-smoker lung cancer, radiotherapy innovation, and the future of precision oncology.
This selection of posts reflects the breadth of today’s lung oncology conversation. Some focus on research milestones and newly published data, while others highlight clinical realities that remain underrecognized in everyday practice. Together, they offer a timely snapshot of where the field stands now and where it is heading next.
Here are the posts you should not miss from experts helping define the future of lung oncology.
Narjust Florez M.D. FASCO –Assistant Professor of Medicine, Dana-Farber Cancer Institute
It is truly an honor to be named a 2026 honoree by the Lung Cancer Research Foundation.
Thankful for the recognition and for the chance to be part of a community driving progress in lung cancer research.

Watch post here
Corinne Faivre-Finn – Professor of Thoracic Radiation Oncology at University of Manchester
Delighted to have contributed to the JTO 20th Anniversary Series: The Optimization of Radiotherapy in Lung Cancer Treatment: 20 Years of Progress.
- Over the past two decades, the treatment landscape for both NSCLC and SCLC has evolved dramatically, driven by advances in imaging, radiotherapy technology, tumour biology, and systemic therapies.
- This review reflected on key prospective trials that have shaped modern lung cancer management and highlighted how radiotherapy has continued to play a central role within increasingly multidisciplinary and personalised treatment strategies.
- A timely look back at how far we have come and forward to the next generation of innovation in thoracic oncology.
Great collaboration with Joseph Salama, Michael Mix, Andrea Bezjak, Jeffrey Bogart
Watch post here
Aakash Desai, MD, MPH, FASCO – Physician Leader, Medical Oncology
Translation of ADCs targeting TROP-2 and cMET into NSCLC clinical practice is currently hindered by subjective visual scoring and inconsistent reproducibility in biomarker assessment. New publication in AACR Journals shows AI can enable this biomarker quantification: https://lnkd.in/egthbvZ6
Key findings:
- Primary endpoint: Recapitulated pathologist annotations for TROP-2 with r = 0.98-0.99
- Key efficacy: Zero-shot generalization to cMET with r = 0.99 and CCC = 0.96 ▪ Safety signal: Not applicable (computational pathology study)
How this fits: Foundation model-based scoring produces expert-level, scalable biomarker quantification.
The resulting TME phenotypes – TROP-2-high immune-deserted vs cMET-high, immune-active – reveal therapeutic implications for combining ADCs with immunotherapies or kinase inhibitors.
What’s next: These findings suggest that automated, modular AI pipelines could potentially standardize ADC biomarker quantification across different protein targets in non-small cell lung cancer research.

Watch post here
Ankit Bharat– Professor & Chief, Executive Director, Canning Thoracic Institute
Every year, lung cancer kills more women than breast cancer. Yet most people don’t know this.
Here’s what keeps me up at night: our current screening guidelines are failing. They focus almost exclusively on heavy smokers ‚ missing never-smokers, young women, and minorities who are dying of advanced lung cancer because they were never eligible for a screening CT.
Our team at Northwestern published data in JAMA Network Open showing that age-based screening would catch ~94% of lung cancers, dramatically reduce disparities, and remain cost-effective.
If we can screen for breast cancer based on age alone, why not lung cancer ‚ the #1 cancer killer?
5 facts most people don’t know about lung cancer:
1. It kills >70,000 women/year in the US (vs ~40,000 for breast cancer)
2. 20% of lung cancers occur in never-smokers
3. Current screening misses the majority of cases
4. When caught early, 5-year survival exceeds 80%
5. A low-dose CT scan takes 5 minutes and costs less than most co-pays
Early detection saves lives. We need to fix lung cancer screening. Now.
Watch post here
Emil Lagumdzic, PhD – PhD in Immunology | Hematology & Oncology
𝐇𝐮𝐠𝐞 𝐥𝐮𝐧𝐠-𝐜𝐚𝐧𝐜𝐞𝐫 𝐬𝐜𝐫𝐞𝐞𝐧𝐢𝐧𝐠 𝐜𝐚𝐦𝐩𝐚𝐢𝐠𝐧 𝐛𝐨𝐨𝐬𝐭𝐬 𝐞𝐚𝐫𝐥𝐲 𝐝𝐢𝐚𝐠𝐧𝐨𝐬𝐢𝐬
A national screening programme increased the number of people diagnosed with early-stage lung cancer in England over half a decade.
In 2019, the English National Health Service (NHS) launched the Lung Cancer Screening Programme, a national initiative that offers scans to people between 55 and 74 years old who have smoked.
Richard Lee at the Royal Marsden NHS Foundation Trust in London and his colleagues analysed data from this programme and calculated that by March last year, more than two million people had been invited for lung-cancer screening, almost one-third of the estimated number of people eligible to take part.
Overall, 1.4% of people scanned were diagnosed with lung cancer.
Roughly three-quarters of those diagnosed had stage 1 or 2 cancers, which are relatively early forms of the disease.
The programme also led to an increase in the number of lung cancers diagnosed at an early stage in people from low-income areas.
The national programme offers an approach for improving early cancer-detection rates that could be adapted by other nations.
Watch post here
Eric Singhi – Thoracic Medical Oncologist Focused on Patient Education & Young-Onset Lung Cancer
Awareness Week matters. Let’s build on it. Together.
There’s a group we don’t talk about enough: young patients with lung cancer under 50, many of whom are caught between “AYA” and traditional “older adult” care models. They are:
-Building careers
-Raising families
-Planning long futures
Navigating a cancer experience that wasn’t designed with them in mind…
These patients are not just younger versions of older adults.
-The biology can be different.
-The life impact is different.
-The support they need is different.
And yet, we’re still catching up…
This is an area I’m deeply committed to…working to better understand it and help shape care that truly reflects these patients and their families. I’m honored to do it with colleagues like Dr. Mara Antonoff & with the support of patient advocacy groups like Rexanna’s Foundation & Young Lung Cancer Initiative.
AYA Week raises awareness. Let’s expand that awareness, so no patient falls in between.

Watch post here
Mihaela Aldea – Medical Oncologist, Gustave Roussy
What happens when patients with RET+ NSCLC are retreated with a same-class selective RET inhibitor?
Among 41 patients included in the RET-MAP registry:
– Switch after toxicity → ORR 67%, mPFS 9.9m. Effective, but toxicity often recurs → monitor closely and consider starting at lower doses;
– Rechallenge after progression → modest overall; signal with selpercatinib in isolated CNS progression on pralsetinib or oligoprogression
– Bypass combos (mostly MET amp) → ORR 39%, mPFS 4m; benefit mainly in patients with prior durable response
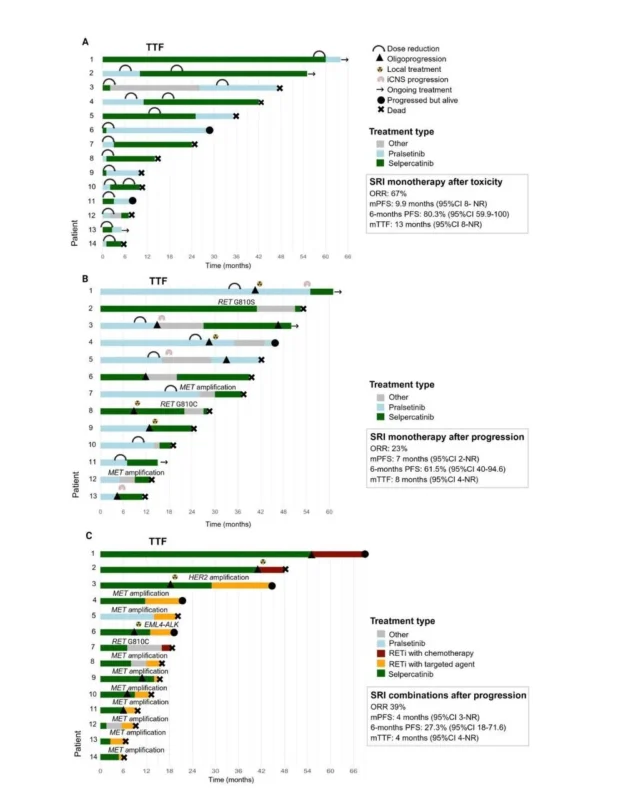
Watch post here
Federico Pio Fabrizio – Associate Professor in Molecular Biology
I’m pleased to share our editorial on the role of tumor-associated macrophages (TAMs) in the response to neoadjuvant chemo-immunotherapy in patients with resectable non small cell lung cancer (NSCLC) published in Cancer Letters.
In this work, we propose that the phenotypic polarization and spatial distribution of TAMs, integrated through spatial transcriptomics approaches, may serve as predictive biomarkers of resistance and contribute to more accurate patient stratification.
Emerging evidence in breast cancer further supports this paradigm, suggesting important translational implications also for NSCLC.
This work is the result of an excellent collaboration among colleagues, enabling the integration of diverse expertise on such a complex topic.

Watch post here
Jeffrey Velotta, MD, FACS – Thoracic Surgeon at Kaiser Permanente
2 Day summit on lung cancer in never smokers, thank you Stanford Center for Asian Health Research and Education It was so great to talk in depth with so many experts in the field, but really great as always to catch up with our international colleagues from Taiwan and leaders from the TALENT study and lung cancer in never smoker Asians Dr. James Yang and Dr. PC Yang and LEARN from their vast experience!!!

Watch post here
Alessandro Russo– MD, PhD Medical Oncologist
A major new dataset strengthens the case for biomarker testing in all NSCLC.
Drawing on molecular profiling data from more than 82,000 people with lung cancer, the study found enough biomarker prevalence across many histological subtypes to support biomarker workup in all NSCLC cases.
For Lung Cancer Europe, this is about getting the diagnosis right from the start. Biomarker testing should be routine in NSCLC across Europe.

Watch post here


