Shikha Jain, Founder, Chair of the Board (Former CEO) at Women in Medicine and Associate Professor of Medicine at The University of Illinois Cancer Center, shared a post on LinkedIn:
“Last week in clinic, I cared for a patient whose cancer was diagnosed at an advanced stage. The biology was not unusual. What stood out was the path that led there. A delayed screening referral. An abnormal test without timely follow-up. Care spread across multiple systems without clear coordination.
In oncology, much of our attention is rightly focused on therapeutic innovation-targeted therapies, immunotherapy, precision medicine. Those advances matter. But long before treatment decisions are made, the structure of the healthcare system often determines when disease is discovered and how quickly care moves forward.
Variability in outcomes is often attributed to complexity. In reality, it is rarely random. More often, it reflects the way systems are built.
Variability Is a System Signal
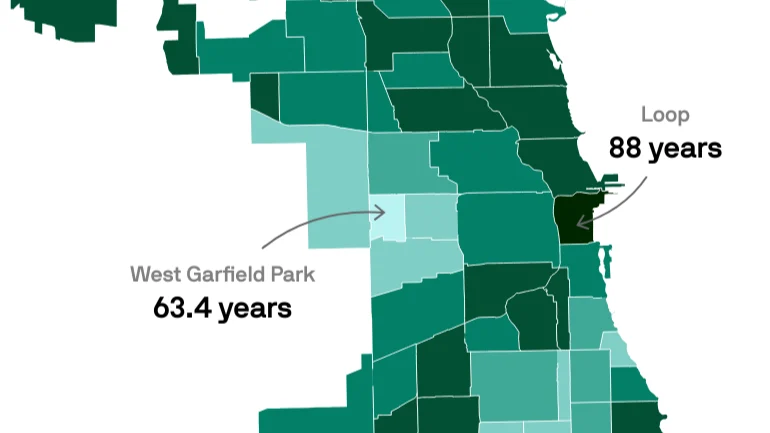
Across the United States, outcomes vary widely by geography, access pathways, and system integration In Chicago, this phenomenon has been described as the “Green Line Effect” (see map above). Traveling along the city’s Green Line, life expectancy shifts dramatically from neighborhood to neighborhood-illustrating how structural conditions surrounding care can shape health outcomes long before a patient enters a clinic. Screening adherence differs dramatically between communities. In colorectal cancer, early-stage detection carries a five-year survival rate above 90%, yet many patients are still diagnosed at later stages where outcomes are significantly worse. These patterns are not isolated lapses. They are signals.
When similar patients experience different outcomes under different system conditions, the explanation is rarely biology alone. It is structure-referral processes, reimbursement incentives, workflow design, data integration, and accountability mechanisms. Healthcare systems reliably produce the outcomes their structures incentivize.
Incentives and Alignment
Much of modern healthcare remains organized around episodic intervention rather than longitudinal prevention. Reimbursement structures frequently reward procedures more clearly than continuity of care. Preventive infrastructure-navigation programs, screening outreach, follow-up systems-often receives less investment than acute treatment delivery.
The consequences are predictable. When screening follow-up is not operationally prioritized, variability increases. When continuity is difficult to coordinate across systems, fragmentation grows. When accountability for missed handoffs is diffuse, delays become normalized.
These outcomes do not reflect individual failure. They reflect structural alignment. Incentives shape behavior. Behavior shapes outcomes. Leadership ultimately determines incentives.
Governance and Predictability
From a governance perspective, the central question is not whether variability exists. The question is whether that variability is predictable under the current structure. When late-stage diagnoses cluster in certain populations or regions, that pattern should be understood as a system output. When workforce constraints lead to delayed access, it reflects decisions about capacity, workflow, and resource allocation.
High-performing industries outside healthcare treat outcome variability as a signal of structural design. Performance improves when leaders examine the architecture that produces results. Healthcare should be no different.
Prevention as Infrastructure
In oncology, early detection remains one of the strongest determinants of survival. Yet preventive systems often receive less strategic attention than treatment innovation.
This imbalance is understandable in an environment where interventions are easier to measure than crises avoided. But prevention is not ancillary to care delivery-it is foundational.
When preventive infrastructure is strong-clear referral pathways, integrated data systems, reliable follow-up mechanisms-variability narrows. When it is fragmented, late diagnosis becomes more likely. Performance follows structure.
The Leadership Question
For healthcare leaders, the most important questions are structural.
What outcomes are our systems currently designed to produce? Where is accountability anchored when follow-through fails? Which metrics truly reflect system health? What variability should we expect under the structures we have built?
Clinicians deliver care within the systems around them. Leadership determines how those systems function.
Closing
Healthcare systems do not drift into better outcomes.
They are structured to produce them. When outcomes vary widely, it is rarely random. It reflects design-and design is ultimately a leadership decision.
If these ideas are useful to your work, you can subscribe to receive future issues of Designing Modern Healthcare here on LinkedIn.”
Other articles featuring Shikha Jain on OncoDaily.


