Muna Al-Khaifi, Lead of Breast Cancer Survivorship Program and GP Oncologist at the Mount Sinai Hospital (Toronto), Sinai Health, presents this article on the role of physical activity across the cancer continuum. This piece explores the growing evidence supporting exercise as a core component of cancer care, highlighting its impact on treatment tolerance, quality of life, survivorship outcomes, and long-term cancer-related outcomes.
The Missing Prescription – Why Physical Activity Should Be Standard Cancer Care
Reframing physical activity as a core component of high-quality cancer care: bridging the gap between evidence, implementation, and patient outcomes
If we measure success in cancer care by survival alone, we are only telling half the story. The future of oncology must be defined not only by how long patients live, but by how well they live.
Physical activity is a safe and feasible intervention across the cancer continuum, including before, during, and after treatment. Pre-treatment optimization (‘prehabilitation’) is associated with improved treatment tolerance, fewer complications, and faster recovery. Increasingly, physical activity is recognized as more than supportive care; it is a core component of comprehensive cancer management with the potential to improve clinical outcomes, enhance quality of life, and even influence survival.
The evidence supporting exercise oncology is now substantial. Physically active individuals demonstrate approximately 10-20% lower overall cancer risk and nearly 20% lower cancer mortality compared with inactive individuals. Emerging evidence also suggests that exercise may influence tumor biology and metastatic potential.
High-intensity aerobic activity has been associated with an approximately 72% lower risk of metastatic cancer in both human cohort and experimental studies. Furthermore, among breast cancer survivors, every additional 10 MET-hours/week of activity, equivalent to several brisk walks weekly, is associated with an estimated 14% reduction in breast cancer mortality.
The current literature consistently demonstrates that exercise improves cardiorespiratory fitness, muscular strength, and body composition, outcomes that directly influence treatment tolerance, functional independence, and recovery. Higher fitness levels are associated with improved surgical outcomes and fewer complications, while resistance training mitigates treatment-related deconditioning. Exercise also alleviates common and distressing symptoms such as fatigue, anxiety, and depression.
Fatigue, one of the most prevalent and debilitating symptoms experienced by cancer patients, has particularly strong evidence supporting exercise as an effective intervention. Moderate-intensity aerobic training performed regularly significantly reduces cancer-related fatigue, with additional benefits observed when combined with resistance training. Improvements in mental health outcomes, including anxiety and depression, are also consistently demonstrated across cancer populations.
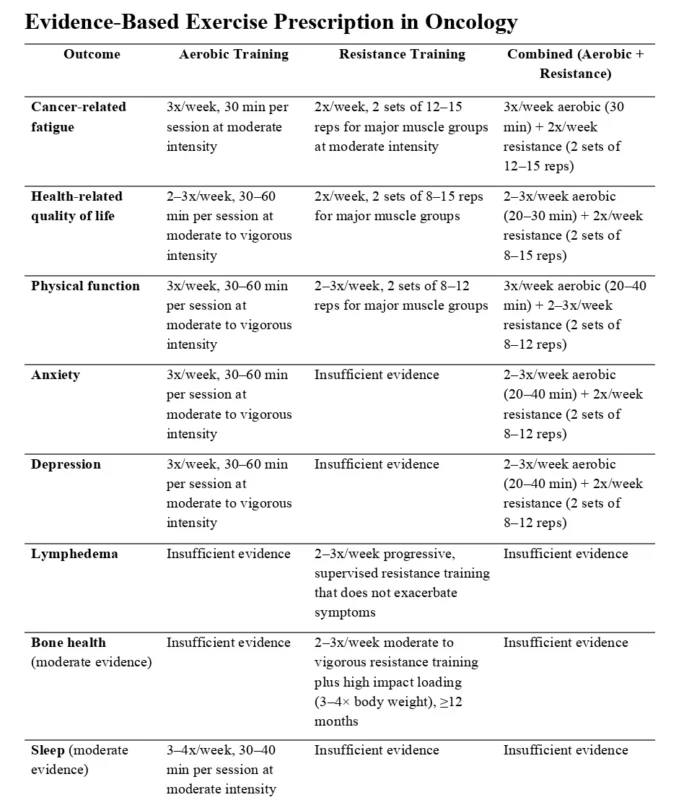
Exercise prescriptions in oncology generally align with public health recommendations but should be individualized based on patient capacity, treatment phase, comorbidities, and symptom burden. Most guidelines support approximately 150 minutes per week of moderate-intensity aerobic activity combined with resistance training twice weekly.
Combined aerobic and resistance programs appear to provide the greatest benefit across multiple outcomes, including fatigue, physical function, and quality of life. Importantly, both supervised and home-based interventions have demonstrated effectiveness, highlighting flexibility and scalability.
Beyond symptom management, emerging evidence suggests that exercise may influence cancer outcomes. The phase III CHALLENGE trial (NCT00819208) evaluated whether structured exercise after adjuvant chemotherapy could improve outcomes in patients with resected colon cancer. In this multicenter randomized trial involving 889 patients across 55 centers, participants were assigned to either a 3-year structured exercise program or health-education materials alone.
After a median follow-up of 7.9 years, the exercise group demonstrated a 28% lower risk of disease recurrence, new primary cancer, or death compared with controls (HR 0.72; 95% CI 0.55-0.94; P=0.02). Five-year disease-free survival improved from 73.9-80.3%, while 8-year overall survival increased from 83.2-90.3%, corresponding to a 37% reduction in mortality risk. The findings provide strong level I evidence that structured physical activity can significantly improve long-term oncologic outcomes in colon cancer survivors.
Despite this strong evidence base, implementation remains inconsistent. Barriers include limited access to programs, variability in clinician knowledge, and competing demands within clinical care. Addressing these gaps requires a coordinated, system-level approach to integrate physical activity into routine oncology practice.
Here Are My Thoughts
Start early with structured assessment.
A pre-exercise assessment should evaluate baseline functional status, treatment phase, comorbidities, and potential contraindications. Where feasible, physical activity should be introduced early-ideally prior to treatment initiation-as part of a prehabilitation strategy to optimize outcomes.
Integrate into routine care with clear accountability.
Exercise counseling should be embedded within standard oncology workflows rather than addressed opportunistically. At a system level, clear ownership-whether through physicians, nurses, or allied health professionals-is essential to ensure consistent, evidence-based delivery.
Adopt a practical, scalable approach.
Implementation does not need to be complex. Brief, structured discussions-often requiring no more than one to two minutes-supported by concise, evidence-based handouts or community resources can be highly effective. When time constraints exist, this responsibility should be intentionally delegated within the care team to ensure consistency.
Leverage multidisciplinary and community partnerships.
Collaboration with physiotherapy, rehabilitation services, and multidisciplinary teams is critical. Referral to structured or cancer-specific exercise programs should be standard practice where available, with community-based programs serving as an important and scalable extension of care.
Individualize and prescribe with intention.
Physical activity should be prescribed with the same level of rigor as pharmacologic therapies. Recommendations must be tailored to cancer type, treatment phase, symptom burden, comorbidities, and patient preferences, with combined aerobic and resistance training generally offering the greatest benefit.
Ensure progression, monitoring, and engagement.
Exercise should begin at an appropriate intensity and progress gradually based on tolerance and clinical status. Ongoing reassessment is essential to adapt to changes over time. Framing physical activity as a meaningful component of treatment-rather than a lifestyle recommendation-enhances engagement, adherence, and sustained behavioral change across the cancer continuum.
Physical activity should not be optional – it should be systematically integrated as a standard of care in oncology.
Figure 1. The figure highlights the benefits of regular exercise in cancer prevention and survivorship, including lower cancer risk, reduced recurrence and metastasis, and improved survival outcomes.

References (Selected)
1. National Comprehensive Cancer Network (NCCN). NCCN Clinical Practice Guidelines in Oncology: Survivorship. Version 2025.
2. American College of Sports Medicine Roundtable. Campbell KL, Winters-Stone KM, Wiskemann J, et al. Exercise Guidelines for Cancer Survivors. Med Sci Sports Exerc. 2019.
3. American College of Sports Medicine. ACSM’s Essentials of Exercise Oncology. 2024.
4. American Society of Clinical Oncology. Ligibel JA, et al. Physical Activity and Exercise Recommendations for Cancer Survivors. 2022.
5. Cormie P, Zopf EM, Zhang X, Schmitz KH. The Impact of Exercise on Cancer Outcomes. Lancet Oncology.
6. Cao C, et al. The Multidisciplinary Community of Exercise Oncology Practice. JNCI Monographs. 2025.
7. Courneya KS, Vardy JL, O’Callaghan CJ, et al. Structured Exercise after Adjuvant Che.
You can also read: Muna Al-Khaifi: Development and Launch of a New Quality Standard for Cancer Survivorship 


