For many women, the first radiotherapy planning appointment is not what they expected. They arrive prepared for treatment. They leave having received none. And in between, something difficult to describe happens: a moment where medicine becomes real — but not yet visible.
This is where confusion begins.
“Why am I here today?”
“Why a CT scan again?”
“Did something change?”
These are not naïve questions. They are the natural result of a process that is clinically precise but often poorly explained.
Because the truth is simple: Nothing therapeutic happens that day. And that is intentional.
Planning Is Not a Delay It Is the Treatment Before the Treatment
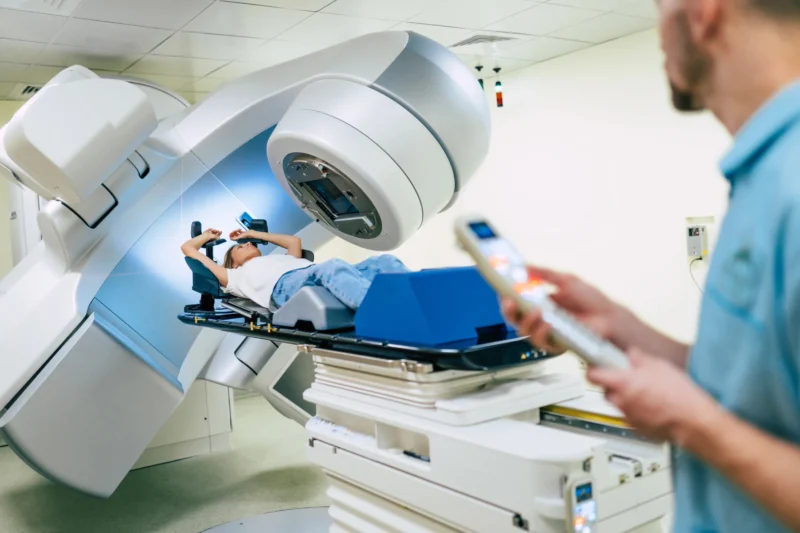
Modern radiotherapy is not something that is “started.” It is something that is built. The planning CT does not aim to diagnose disease or evaluate response. It exists for a different purpose entirely: to map the patient’s anatomy in the exact position in which treatment will be delivered.
Position is not a detail.
It is geometry.
And geometry determines dose.
In breast radiotherapy, arm positioning, chest wall contour, breast mobility, and in selected cases breathing patterns, directly influence dose distribution to both target and organs at risk. Without this step, radiotherapy would be approximation. With it, it becomes precision.
What Happens After the Patient Leaves the Room
From the patient’s perspective, the process appears to stop after the scan. In reality, this is where the most technical phase begins. Target volumes are defined. Organs at risk are contoured. Dose distributions are calculated. Plans are evaluated and verified. This is not administrative work. It is clinical decision-making translated into physics. Radiotherapy depends on pre-treatment accuracy more than intra-treatment correction. Once delivery begins, the plan must already be right.
This is why time is required. Not because the system is slow. But because it is designed to reduce error before exposure.
The Invisible Gap That Patients Feel
Between planning and first treatment lies a space that clinicians often underestimate. Patients describe it as waiting. Clinically, it is preparation. Emotionally, it is uncertainty. This gap matters more than we acknowledge. Because when patients are not told what is happening, they interpret the silence. And silence in oncology is rarely neutral. It becomes doubt or fear.
Or the sense that something is being delayed. In reality, the opposite is happening. Radiotherapy is one of the most protocol-driven treatments in oncology. Every step from simulation to verification exists to minimize risk and variability.
Nothing is rushed.
Nothing is improvised.
Why This Appointment Is Often Misunderstood
Part of the problem lies in language. Calling it “just a CT” reduces its significance. Presenting it as a routine step removes its meaning. But for the patient, this is the first moment where treatment becomes embodied.
They are positioned.
They are marked.
They are aligned to a system they do not yet understand. And then they leave. Without context, this feels incomplete. With context, it becomes reassuring.
The Shift Toward Patient-Centered Oncology
Modern oncology increasingly recognizes that outcomes are not defined solely by survival or imaging. Patient-reported outcomes (PROs) — including quality of life, symptoms, and functional status are now considered critical endpoints in cancer care and research.
Frameworks developed by organizations such as the EORTC aim to ensure that the patient voice is not an afterthought, but a structured and measurable component of treatment evaluation. This shift has consequences.
It means that how patients experience treatment including how they understand it is no longer peripheral. It is part of the quality of care.
What Patients Actually Need to Hear
Not technical explanations. Not contouring theory. Not DVHs.
Just this: Today was not the start of your treatment.
It was the start of designing it. That sentence alone can transform the experience. Because it replaces uncertainty with structure.
A Final Thought
Radiotherapy is one of the few areas in medicine where doing things quickly is rarely a virtue. Precision requires pause. Safety requires preparation. And planning is not an interruption of treatment. It is what makes treatment possible. So when nothing “happens” on that first day, something essential is already underway. The treatment is being made worthy of delivery.
Written by Eftychia Tataridou, MD


