Pleural mesothelioma remains one of the most aggressive thoracic malignancies, with historically limited survival and few reliable biomarkers to guide prognosis. While clinical stage and histologic subtype have traditionally served as the primary predictors of outcomes, emerging molecular insights are beginning to reshape how clinicians understand the disease. A large multi-institutional analysis from the IASLC staging database now provides important evidence that pleural mesothelioma molecular alterations significantly influence survival and may enhance prognostic modeling beyond conventional clinical parameters.
The analysis evaluated genomic and immunohistochemical biomarkers across a carefully curated cohort drawn from three major cancer centers participating in the IASLC pleural mesothelioma staging project. By integrating next-generation sequencing (NGS) data with clinical information and immunohistochemistry results, investigators explored whether pleural mesothelioma molecular alterations could provide additional prognostic value when combined with traditional staging systems.
Why Prognostic Biomarkers Are Needed in Pleural Mesothelioma
Pleural mesothelioma is a rare but highly lethal cancer of the pleural lining. Without treatment, median overall survival ranges from 7 to 9 months, and even with multimodal therapy, outcomes remain poor for many patients.
Historically, clinicians have relied primarily on:
- Tumor stage
- Histologic subtype
- Performance status
to estimate prognosis. Patients with epithelioid tumors and earlier-stage disease generally have the most favorable outcomes, while non-epithelioid histologies such as biphasic or sarcomatoid subtypes are associated with worse survival.
However, outcomes vary widely even among patients with the same stage and histology. This variability has prompted growing interest in genomic biomarkers that may refine prognostic stratification. In particular, tumor suppressor genes frequently altered in mesothelioma have emerged as potential determinants of clinical outcomes.
The IASLC study was designed to determine whether pleural mesothelioma molecular alterations could improve survival prediction beyond the existing TNM staging framework.
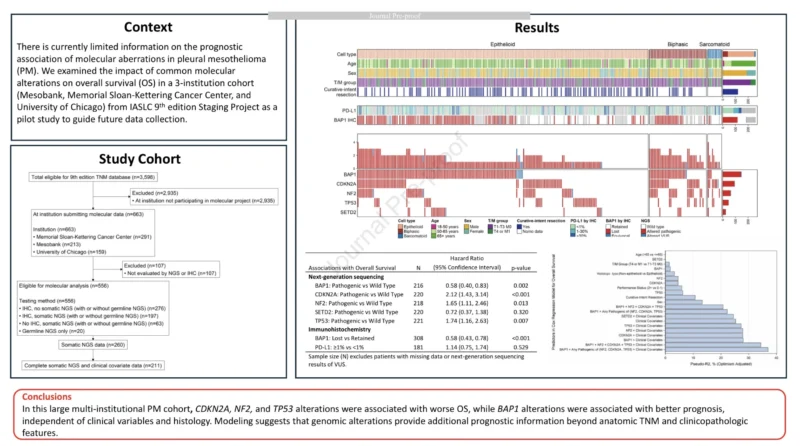
Study Cohort and Patient Characteristics
The study analyzed 556 patients with pleural mesothelioma diagnosed between 2013 and 2022 whose clinical and molecular data were included in the IASLC 9th edition staging database.
Key characteristics of the cohort included:
- 77.7% of patients were older than 65 years (432 of 556 cases).
- 72.7% were male (404 of 556 patients).
- 77.5% had epithelioid mesothelioma (431 cases).
- 13.1% had biphasic tumors and 9.4% had sarcomatoid tumors.
Treatment patterns reflected real-world management:
- 29.3% underwent curative-intent surgical resection.
- 82.0% received systemic therapy.
Most patients presented with relatively advanced disease, though 69.6% were classified as T1–T3 M0, indicating locally advanced but non-metastatic disease at diagnosis.
This large and clinically annotated cohort provided an important foundation for evaluating pleural mesothelioma molecular alterations and their impact on survival.
The Genomic Landscape of Pleural Mesothelioma
Next-generation sequencing was performed in 260 tumors, allowing investigators to characterize the frequency of key genetic events associated with mesothelioma.
The most common genomic alterations were:
- BAP1 mutations: 55.0% (143 of 260 tumors)
- CDKN2A alterations: 36.2% (94 tumors)
- NF2 alterations: 23.8% (62 tumors)
- TP53 alterations: 18.1% (47 tumors)
- SETD2 alterations: 8.8% (23 tumors)
These findings confirm that tumor suppressor gene disruption represents a dominant feature of mesothelioma biology. Unlike many other cancers driven by oncogenic mutations, mesothelioma typically arises from loss of tumor suppressor pathways.
The distribution of alterations also showed relationships with tumor subtype. For example, CDKN2A and NF2 alterations occurred more frequently in non-epithelioid tumors, which are known to carry worse clinical outcomes.
Understanding these patterns helps explain how pleural mesothelioma molecular alterations may influence disease behavior.
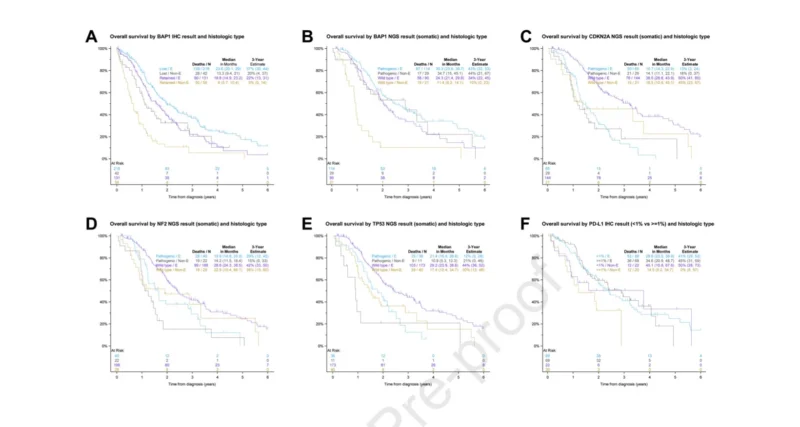
BAP1 Alterations and Expression Patterns
BAP1 emerged as the most frequently altered gene in the cohort. Mutations were detected in 55% of tumors, and immunohistochemistry revealed loss of BAP1 expression in 57.5% of cases.
The concordance between NGS and immunohistochemistry was high:
- 90.1% agreement between BAP1 IHC and sequencing results.
Loss of BAP1 expression was also more common in epithelioid tumors:
- 62.5% in epithelioid tumors
- 41.6% in non-epithelioid tumors.
These findings highlight the importance of integrating both genomic and protein-level testing when evaluating pleural mesothelioma molecular alterations.
PD-L1 Expression in Mesothelioma
The study also evaluated immune biomarker expression. PD-L1 staining was assessed in 200 tumors, with the following findings:
- 44.5% of tumors were PD-L1 positive (≥1% tumor cells staining).
- 55.5% were PD-L1 negative.
Most PD-L1–positive tumors showed relatively low expression levels:
- 69.7% of PD-L1–positive cases had staining in 30% or fewer tumor cells.
Importantly, PD-L1 expression did not demonstrate a statistically significant association with overall survival, suggesting that this immune biomarker may have limited prognostic value in pleural mesothelioma.
Molecular Alterations Associated With Survival
The most clinically relevant findings emerged from survival analyses.
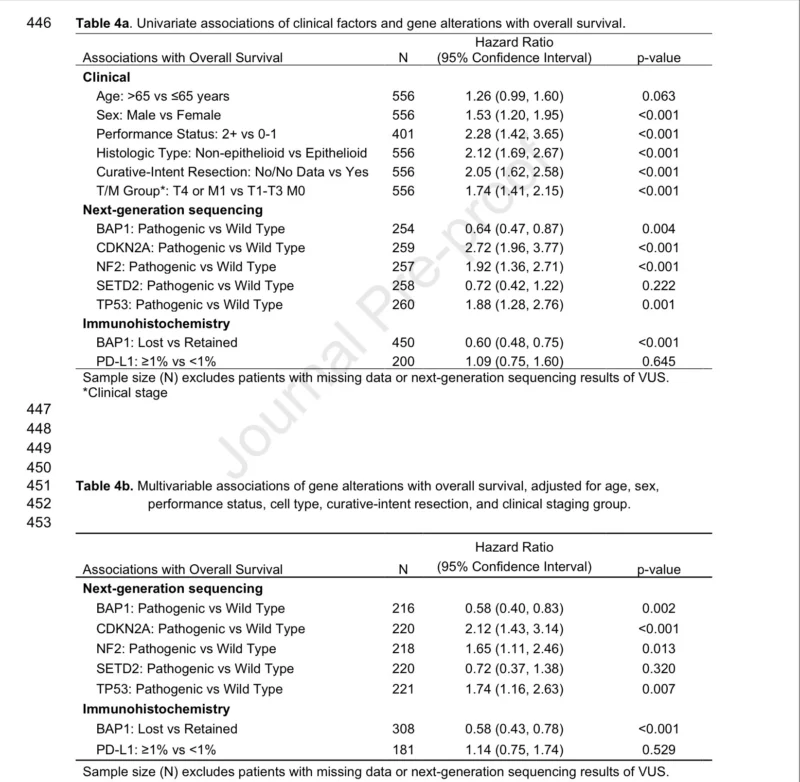
In univariate analysis, several pleural mesothelioma molecular alterations were significantly associated with overall survival.
Genomic alterations linked to worse survival included:
- CDKN2A mutations (HR 2.72; 95% CI 1.96–3.77; p < 0.001)
- NF2 mutations (HR 1.92; 95% CI 1.36–2.71; p < 0.001)
- TP53 mutations (HR 1.88; 95% CI 1.28–2.76; p = 0.001)
Conversely, BAP1 alterations were associated with better survival:
- BAP1 mutation HR 0.64 (p = 0.004)
- BAP1 loss by IHC HR 0.60 (p < 0.001).
These associations remained significant after adjusting for clinical factors in multivariable models.
Adjusted hazard ratios included:
- CDKN2A: HR 2.12
- NF2: HR 1.65
- TP53: HR 1.74
- BAP1 mutation: HR 0.58
- BAP1 loss by IHC: HR 0.58.
These results suggest that CDKN2A loss may be one of the strongest molecular predictors of poor survival in pleural mesothelioma.
Combining Molecular and Clinical Data Improves Prognostic Models
Investigators also compared predictive models using clinical variables alone versus molecular biomarkers.
Clinical factors alone produced:
- C-statistic: 0.67
- Pseudo-R²: 25.3.
Genomic biomarkers alone were slightly less predictive:
- C-statistic: 0.65
- Pseudo-R²: 20.8.
However, the best predictive model combined both clinical and molecular features.
When BAP1 alterations and any mutation in CDKN2A, NF2, or TP53 were integrated with clinical variables, predictive performance improved to:
- C-statistic: 0.70
- Pseudo-R²: 37.0.
This demonstrates that pleural mesothelioma molecular alterations provide complementary prognostic information beyond TNM staging alone.
Implications for Future Mesothelioma Staging
These findings have important implications for the future of mesothelioma classification and patient management.
While traditional staging remains essential, genomic biomarkers may help:
- refine prognostic stratification
- guide treatment selection
- improve pathology reporting
- inform future staging systems.
The IASLC staging project aims to incorporate larger genomic datasets in future revisions of the TNM classification. Integrating molecular data into staging could ultimately lead to more personalized risk assessment for patients with mesothelioma.
A New Layer of Prognostic Insight
This large multi-institutional analysis demonstrates that pleural mesothelioma molecular alterations significantly influence patient survival and can strengthen prognostic models when combined with clinical variables.
Alterations in CDKN2A, NF2, and TP53 identify patients with poorer outcomes, while BAP1 alterations are associated with improved survival, highlighting the complexity of mesothelioma biology.
As molecular testing becomes increasingly routine in thoracic oncology, these biomarkers may play a central role in future staging systems and clinical decision-making for pleural mesothelioma.
You can read full article in Journal of Thoracic Oncology. 2026. Journal Pre-Proof


