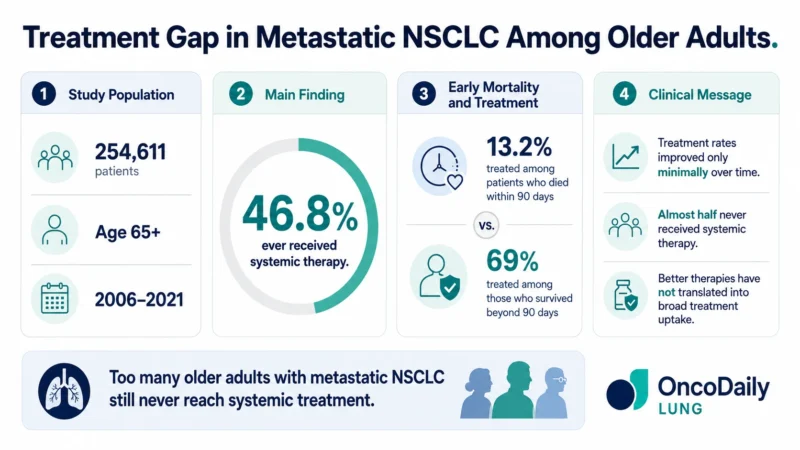
A large population-based study published in JAMA Oncology delivers a sobering message for thoracic oncology: despite major advances in metastatic non–small cell lung cancer, systemic treatment still does not reach a large proportion of older adults. In an analysis of more than 250,000 patients aged 65 years and older with metastatic NSCLC, only 46.8% ever received systemic therapy, and treatment rates improved only minimally between 2006 and 2021.
The study, led by Fox and colleagues, used linked SEER-Medicare data to evaluate real-world treatment patterns in older adults diagnosed with metastatic NSCLC over a 15-year period. The investigators included 254,611 patients diagnosed from January 2006 through December 2021 and examined both temporal trends and clinical or sociodemographic factors associated with treatment receipt.
A Treatment Gap That Persists Despite Therapeutic Progress
This finding is striking because the study period spans one of the most transformative eras in lung cancer care. Over those years, metastatic NSCLC treatment moved from largely cytotoxic chemotherapy toward biomarker-driven targeted therapy and immunotherapy, with clear gains in efficacy and tolerability for many patients. Yet at the population level, these advances did not translate into a major increase in the proportion of older adults who actually received systemic treatment.
The investigators found that 119,197 of 254,611 patients received systemic therapy, corresponding to 46.8% of the entire cohort. That means more than half of older adults with metastatic NSCLC were never treated systemically at all. Even more concerning, the proportion treated increased only slightly over time.
Early Mortality Was A Major Barrier
One of the clearest explanations for underuse of treatment was very early mortality. Among the 100,367 patients who died within 90 days of diagnosis, only 13.2% received systemic therapy. By contrast, among patients who survived longer than 90 days, 69% received treatment. This sharp difference highlights how many patients are either diagnosed too late, deteriorate too quickly, or fail to enter oncology care early enough to receive active treatment.
This is an important point clinically. The treatment gap is not explained only by patient preference or treatment intolerance. It also reflects a system-level problem of timing, access, and referral in a disease where delays can eliminate the opportunity for therapy altogether.
Referral To Oncology Was One Of The Strongest Predictors
Among all the variables examined, referral to an oncology specialist stood out as one of the strongest factors associated with treatment receipt. In the competing risk model, oncology referral had a hazard ratio of 2.5 and corresponded to a 30.3% greater cumulative incidence of treatment at 180 days compared with no referral. Biomarker testing was also strongly associated with treatment, corresponding to a 17.8% greater cumulative incidence of treatment at 180 days.
That finding carries major practical relevance. In modern NSCLC, biomarker testing is not only a diagnostic step. It is increasingly a gateway to treatment. Patients who are evaluated in a setting where biomarker testing is performed and oncology referral happens promptly are far more likely to receive systemic therapy.
Who Was Less Likely To Be Treated?
The study also identified several characteristics associated with lower treatment rates. Patients older than 80 years had a 15.4% lower cumulative incidence of treatment at 180 days compared with those aged 65 to 69 years. Histology also mattered: patients with NSCLC not otherwise specified had a 12.8% lower cumulative incidence of treatment than those with adenocarcinoma. Additional factors associated with treatment differences included comorbidity burden, marital status, Medicare Part C or Part D coverage, rurality, and race and ethnicity.
These data suggest that under-treatment is not random. It is shaped by age, pathology quality, social support, insurance structure, and healthcare access. In other words, this is not only a biologic problem. It is a care-delivery problem.
Why This Study Matters Now
The timing of this paper is important. The lung cancer field increasingly focuses on sophisticated questions such as optimal first-line sequencing, resistance biology, and use of novel antibody-drug conjugates or targeted combinations. But this study brings attention back to a more basic and uncomfortable reality: many patients never even reach the point where those treatment decisions can be made.
That is especially relevant in older adults, who make up a large proportion of the metastatic NSCLC population. If nearly half remain untreated despite the availability of more effective and better tolerated systemic options, then the main challenge is not only drug development. It is implementation.

The Bigger Clinical Message
This study does not argue that every older patient with metastatic NSCLC should automatically receive systemic therapy. Fitness, comorbidity burden, patient goals, and expected benefit still matter. But it strongly suggests that many patients who could potentially benefit are not reaching treatment, and that the gap begins early, often before oncology referral or biomarker testing have even occurred.
The most important clinical takeaway may be simple: improving treatment rates in metastatic NSCLC will require more than better drugs. It will require earlier recognition, faster specialist referral, more complete diagnostic workup, and a more reliable pathway from diagnosis to treatment initiation.
Read full article here


