Sami Mansfield, Founder, Oncology Exercise and Lifestyle Medicine Consultant, Operations and Implementation Expert, shared a post on LinkedIn:
“This might be one of the most fascinating cancer + lifestyle medicine intersections I’ve read in a while.
“The brain is an exquisite sensor of what’s going on in your body… But it requires balance.”
– Jeremy Borniger, Cold Spring Harbor Laboratory
- In mouse models, Borniger’s lab found something remarkable:
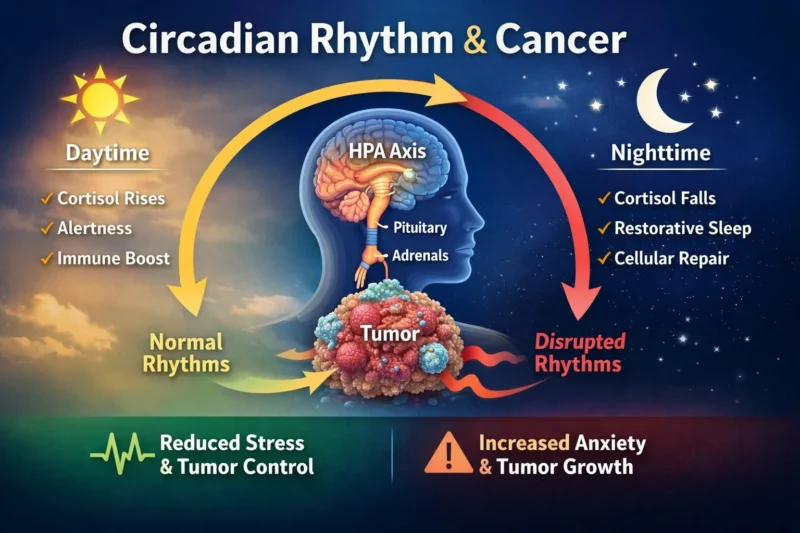
- Breast cancer disrupted normal day–night rhythms of corticosterone (the rodent version of cortisol). Instead of rising and falling predictably, levels became “flattened.”
- That blunted rhythm was associated with reduced quality of life and increased mortality.
And here’s what really caught my attention:
Even before tumors were palpable, stress hormone rhythms were already 40–50% blunted – within just three days of inducing cancer.
Let that sink in.
Cancer wasn’t just growing in the body.
It was altering the brain’s stress regulation circuitry almost immediately.
Why This Matters for Humans?
In humans, cortisol follows a diurnal rhythm – higher in the morning, lower at night.
- When that rhythm flattens, we often see:
- Insomnia
- Anxiety
- Fatigue
- Immune dysregulation
- Poorer outcomes in chronic disease
- The HPA axis (hypothalamus-pituitary-adrenal) is the feedback loop responsible for maintaining this rhythm. In the mouse model, key hypothalamic neurons were essentially “locked” into a hyperactive but ineffective state. But here’s the most intriguing part:
When researchers restored the normal rhythm at the correct time of day:
- Stress hormone patterns normalized
- Anti-cancer immune cells increased in the tumor
- Tumors shrank
When they stimulated at the wrong time of day?
No anti-cancer effect.
- Timing mattered.
- Rhythm mattered.
- Balance mattered.
As a Lifestyle Medicine and Exercise Oncology Consultant, Here’s What I See.
We often talk about:
- Nutrition
- Exercise
- Body composition
- Weight loss
But this research reinforces something we don’t emphasize enough:
Circadian rhythm is not a “nice to have.”
It may be a therapeutic lever.
Simple implementations that support rhythm:
- Morning light exposure
- Consistent sleep/wake timing
- Strength training earlier in the day
- Reducing eating late at night
- Reducing late-night light and stimulation
- Practicing breathwork
These aren’t fringe ideas.
They are biologically grounded interventions that influence the HPA axis, immune function, and potentially tumor biology.
We are getting better at precision oncology.
But this reminds us that physiology is rhythmic.
And when rhythm is lost, systems unravel.
Small shifts.
Consistent timing.
Restoring balance.
This is why lifestyle medicine isn’t “extra.”
It’s foundational.
I’ll be watching this research closely.
Curious – how often are you talking about sleep in oncology care?”
Other articles on OncoDaily.


