Craniopharyngiomas are rare, benign brain tumors that develop near the pituitary gland and hypothalamus, which are critical regions for hormone regulation and other vital functions. Despite being non-cancerous, these tumors can be aggressive and cause significant morbidity due to their location and potential impact on surrounding structures.
Prevalence and Epidemiology
Craniopharyngiomas are relatively rare, with an incidence rate of approximately 0.5 to 2 cases per million people annually. They account for about 1-3% of all brain tumors in children and 1-2% of all primary intracranial neoplasms in adults. These tumors exhibit a bimodal age distribution, primarily affecting children aged 5-14 years and adults aged 50-74 years. There is no significant gender or racial bias in the occurrence of craniopharyngiomas.
Types
Craniopharyngiomas are classified into two main histological subtypes:
- Adamantinomatous Craniopharyngioma (ACP): This type is more common in children and is characterized by cystic and solid components with calcifications. Mutations in the CTNNB1 gene (plays a crucial role in cell adhesion and signaling) are often present in ACP.
- Papillary Craniopharyngioma (PCP): This type is more common in adults and is typically solid with fewer cystic elements. BRAF V600E mutations (lead to the production of an abnormal protein that drives cell growth and division) are commonly found in PCP.
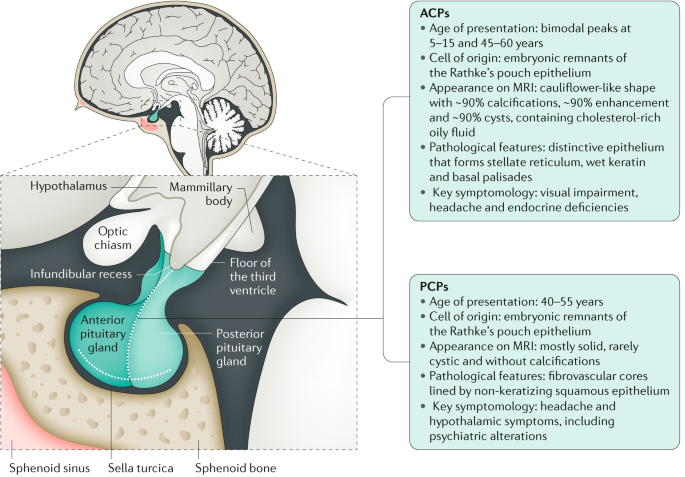
The image is taken from a paper authored by Müller et al. (2019).
Causes and Risk Factors
The exact cause of craniopharyngiomas is unknown. These tumors are thought to arise from embryonic remnants of Rathke’s pouch, a structure involved in the development of the pituitary gland. There are no known definitive risk factors, and craniopharyngiomas are considered sporadic tumors, meaning they occur randomly without a clear genetic or environmental cause.
Symptoms
Craniopharyngiomas can cause a wide range of symptoms due to their proximity to critical brain structures. Symptoms often develop slowly and may include:
- Headaches: Commonly due to increased intracranial pressure.
- Visual Disturbances: Including blurred vision, double vision, and loss of peripheral vision, caused by pressure on the optic nerves.
- Balance and coordination problems: Due to pressure on nearby brain structures.
- Cognitive and behavioral changes: Such as memory issues, mood swings, and personality changes.
- Endocrine Dysfunction: Symptoms such as growth failure, delayed puberty, hypothyroidism, adrenal insufficiency, and diabetes insipidus due to pituitary gland involvement.
- Neurological Symptoms: Including balance problems, confusion, mood swings, and behavioral changes.
- Increased Thirst and Urination: Due to diabetes insipidus (disease caused by either low vasopressin or resistance to it).
- Nausea and Vomiting: Often related to increased intracranial pressure.
- Appetite changes: Either increased or decreased appetite, depending on the specific hormonal imbalances.
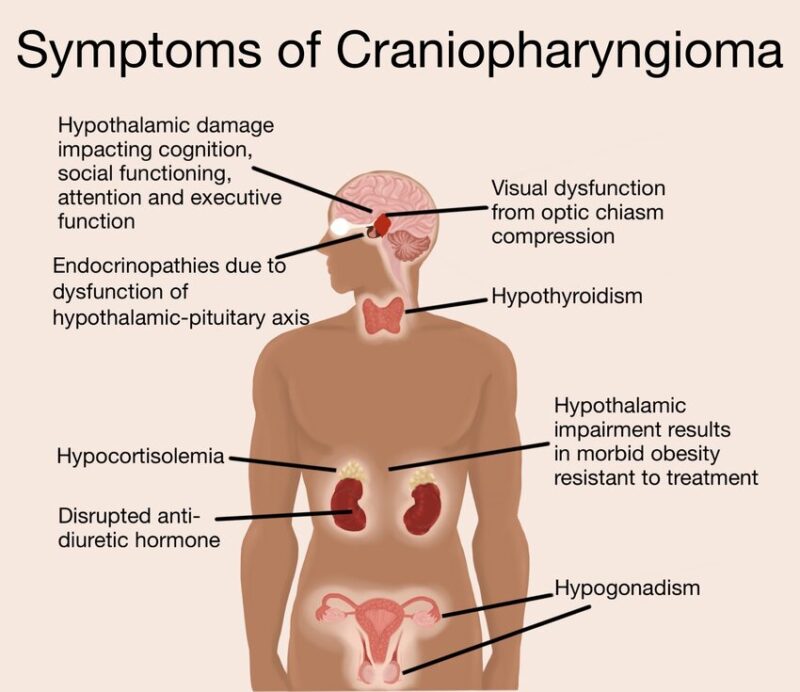
The image is taken from a paper authored by Reyes et al. (2022).
Diagnosis
Craniopharyngiomas are typically diagnosed through a combination of clinical evaluation, imaging studies, and, in some cases, biopsy or surgical removal of the tumor.
- Clinical evaluation: A detailed medical history and physical examination, including assessment of vision, neurological function, and endocrine status, can provide important clues for diagnosis.
- Imaging studies:
- Magnetic Resonance Imaging (MRI): MRI is the preferred imaging modality for detecting and characterizing craniopharyngiomas. It can reveal the tumor’s size, location, and relationship to surrounding structures.
- Computed Tomography (CT) scan: CT scans can also be useful, particularly for detecting calcifications within the tumor, which are common in craniopharyngiomas.
- Biopsy or surgical removal: In some cases, a biopsy or surgical removal of the tumor may be necessary for definitive diagnosis and to distinguish craniopharyngiomas from other types of brain tumors or lesions.
Craniopharyngioma Treatment Options
The treatment of craniopharyngiomas typically involves a multidisciplinary approach, combining surgical intervention, radiotherapy, and hormonal replacement therapy. The specific treatment plan is tailored to each individual patient, considering factors such as age, tumor characteristics, and potential risks and benefits.
Surgical Treatment
Surgery is often the primary treatment modality for craniopharyngiomas, with the goal of maximizing tumor removal while minimizing damage to surrounding critical structures. Surgical approaches include:
- Transcranial approaches: These involve creating an opening in the skull (craniotomy) to access the tumor. Common approaches include the pterional, subfrontal, and interhemispheric routes.
- Transsphenoidal (endonasal endoscopic) approach: This minimally invasive approach involves accessing the tumor through the nose and sphenoid sinus, using an endoscope for visualization.
Extent of resection
- Gross total resection: Complete removal of the visible tumor. This approach may increase the risk of treatment-related morbidity but can improve long-term outcomes and reduce the risk of recurrence.
- Subtotal resection: Partial removal of the tumor, often performed when the tumor is adherent to critical structures or complete resection carries an unacceptable risk. This approach is typically followed by adjuvant radiotherapy.
Radiotherapy
Radiotherapy is commonly used as an adjuvant treatment after subtotal resection or for recurrent tumors. It can help control residual or recurrent tumor growth and improve long-term tumor control rates.
- External beam radiation therapy: This involves delivering radiation from an external source to the tumor site. Various techniques, such as intensity-modulated radiation therapy and proton beam therapy, can be used to minimize radiation exposure to surrounding healthy tissues.
- Stereotactic radiosurgery: This highly precise form of radiation therapy delivers a high dose of radiation to the tumor in a single or few fractionated sessions, minimizing exposure to surrounding tissues.
- Hormonal Replacement Therapy: Due to the potential impact of craniopharyngiomas and their treatment on the pituitary gland and hypothalamus, many patients require long-term hormonal replacement therapy to manage endocrine deficiencies. Common hormonal replacements include:
- Growth hormone for children with growth failure
- Thyroid hormone for hypothyroidism
- Cortisol or hydrocortisone for adrenal insufficiency
- Sex hormones (estrogen, testosterone) for hypogonadism
- Desmopressin (an analogue of vasopressin) for diabetes insipidus
Emerging Targeted Therapies
Recent advancements in the molecular understanding of craniopharyngiomas have led to the development of targeted therapies, particularly for tumors with specific genetic mutations.
- BRAF Inhibitors: The discovery of the BRAF V600E mutation in papillary craniopharyngiomas has led to the use of BRAF inhibitors. These drugs have shown remarkable efficacy in shrinking tumors and improving clinical outcomes, offering a less invasive alternative to traditional treatments.
- MEK Inhibitors: Often used in combination with BRAF inhibitors, MEK inhibitors (MEK gene encodes a protein kinase involved in the MAPK/ERK signaling pathway, which regulates cell growth, division, and differentiation) have demonstrated significant tumor reduction and improved patient outcomes.
This video, produced by the Pacific Neuroscience Institute, presents surgical techniques for the endoscopic endonasal approach.
Patient Survivorship
While survival rates for craniopharyngioma patients have improved significantly in recent decades, long-term survivorship and quality of life remain major challenges due to the potential for treatment-related morbidities and the chronic nature of the condition.
Long-term Follow-up and Monitoring
Regular follow-up and monitoring are essential for craniopharyngioma survivors to detect and manage any potential complications or recurrences. This typically involves:
- Periodic imaging studies (MRI or CT scans) to monitor for tumor recurrence or progression.
- Regular assessment of endocrine function and adjustment of hormonal replacement therapy as needed.
- Monitoring of visual function and neurological status.
- Evaluation of cognitive and psychosocial well-being.
Quality of Life Considerations
Despite advances in treatment, many craniopharyngioma survivors experience significant long-term morbidities that can impact their quality of life, including:
- Endocrine disorders (e.g., obesity, growth failure, sexual dysfunction)
- Visual impairments
- Neurological deficits (e.g., cognitive impairment, balance issues)
- Psychosocial challenges (e.g., depression, anxiety, social isolation)
- Increased risk of cardiovascular disease and metabolic disorders
Problems During and After Treatment and How to Manage Them
Craniopharyngioma treatment and the tumor itself can lead to various complications and problems that require careful management:
- Hormonal imbalances: As mentioned earlier, pituitary and hypothalamic dysfunction can result in various hormonal deficiencies, such as growth hormone deficiency, hypothyroidism, adrenal insufficiency, and diabetes insipidus. These conditions require appropriate hormonal replacement therapy and regular monitoring to ensure optimal management.
- Visual impairments: Damage to the optic nerves or chiasm can lead to visual field defects, double vision, or even blindness. Regular ophthalmological evaluations and, in some cases, vision therapy or assistive devices may be necessary.
- Neurological complications: Craniopharyngiomas and their treatment can potentially cause neurological issues such as cognitive impairment, memory problems, balance and coordination difficulties, and seizures. Rehabilitation services, including physical therapy, occupational therapy, and cognitive therapy, may be beneficial in managing these complications.
- Obesity and metabolic disorders: Hypothalamic dysfunction can lead to severe obesity, insulin resistance, and other metabolic disorders. A multidisciplinary approach involving endocrinologists, dietitians, and exercise specialists may be required to manage these issues effectively.
- Psychosocial challenges: The physical and cognitive impacts of craniopharyngiomas can take a toll on mental health, leading to conditions such as depression, anxiety, and social isolation. Psychological counseling, support groups, and other psychosocial interventions can be invaluable in addressing these challenges.
- Tumor recurrence: Despite treatment, craniopharyngiomas can recur in up to 25% of cases. Regular follow-up and monitoring are crucial for early detection and management of recurrences, which may require additional surgery, radiotherapy, or other interventions.
Recommendations for Patients
Coping with a craniopharyngioma diagnosis and its long-term implications can be challenging. Here are some recommendations for patients and their caregivers:
- Seek care from a multidisciplinary team: Due to the complex nature of craniopharyngiomas and their potential impact on various body systems, it is essential to receive care from a team of specialists, including neurosurgeons, endocrinologists, ophthalmologists, neurologists, and others as needed.
- Educate yourself: Learn as much as they can about craniopharyngiomas, treatment options, and potential complications. This knowledge will help them make informed decisions and better understand the challenges they may face.
- Advocate for yourself: Feel empowered to ask questions, voice concerns, and participate in shared decision-making regarding their treatment plan.
- Seek support: Connect with support groups, counselors, or other resources to help you cope with the emotional and practical challenges of living with a craniopharyngioma.
- Maintain a healthy lifestyle: While it may be challenging, try to maintain a balanced diet, regular exercise (as tolerated), and good sleep habits. These can help manage some of the potential complications, such as obesity and metabolic disorders.
- Stay vigilant: Attend all follow-up appointments and report any new or concerning symptoms to healthcare team promptly. Early detection and management of complications or recurrences can improve outcomes.
- Plan for the future: Discuss long-term care plans and advance directives with their healthcare team and loved ones, ensuring their wishes are understood and respected.
Prognosis
The prognosis for craniopharyngioma patients is generally good, with high survival rates. The 5-year survival rate ( the percentage of patients alive after a set period post-diagnosis or treatment) is around 80-90%, but recurrence is common, occurring in about one-third of patients. Several factors can influence the prognosis and outcomes of craniopharyngioma patients, including:
- Age at diagnosis: Younger age at diagnosis, particularly in childhood, is associated with a higher risk of long-term morbidity and impaired quality of life.
- Tumor size and location: Larger tumors and those invading critical structures like the hypothalamus or optic pathways are more challenging to treat and carry a higher risk of complications.
- Extent of surgical resection: Gross total resection, when feasible, is associated with improved survival and reduced risk of recurrence compared to subtotal resection. However, gross total resection may increase the risk of treatment-related morbidity.
- Use of adjuvant radiotherapy: Radiotherapy, often used after subtotal resection, can improve tumor control but may also contribute to long-term endocrine and cognitive deficits, particularly in younger patients.
- Tumor recurrence: Recurrence of the tumor, which can occur in up to 25% of cases, is associated with poorer outcomes and increased treatment-related morbidity.
Conclusion
Craniopharyngiomas, though benign, pose significant challenges due to their location and potential impact on critical brain structures. Understanding the prevalence, types, symptoms, and treatment options is crucial for patients and their families. Advances in surgical techniques, radiotherapy, and particularly emerging targeted therapies like BRAF and MEK inhibitors, offer new hope for improved outcomes and quality of life. Ongoing research and clinical trials continue to enhance our understanding and management of this complex condition, promising a brighter future for those affected. With comprehensive care and support, many patients can lead fulfilling lives despite the challenges posed by craniopharyngiomas.
Resources
- American Cancer Society – cacner.org
- National Cancer Institute – cancer.gov
- American Brain Foundation
- American Society of Clinical Oncology – asco.org
- American Brain Tumor Association – abta.org
- Craniopharyngioma – Endocrine Reviews
- Advancing Craniopharyngioma Management: A Systematic Review of Current Targeted Therapies and Future Perspectives – International Journal of Molecular Sciences
- Radiopaedia – radiopedia.org
- Canadian Cancer Society – cancer.ca


